Accuracy of a Dual-Sensor Heat-Flux (DHF) Non-Invasive Core Temperature Sensor in Pediatric Patients Undergoing Surgery
- PMID: 38002632
- PMCID: PMC10672443
- DOI: 10.3390/jcm12227018
Accuracy of a Dual-Sensor Heat-Flux (DHF) Non-Invasive Core Temperature Sensor in Pediatric Patients Undergoing Surgery
Abstract
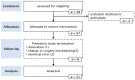
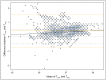
Accurate temperature measurement is crucial for the perioperative management of pediatric patients, and non-invasive thermometry is necessary when invasive methods are infeasible. A prospective observational study was conducted on 57 patients undergoing elective surgery. Temperatures were measured using a dual-sensor heat-flux (DHF) thermometer (Tcore™) and a rectal temperature probe (TRec), and the agreement between the two measurements was assessed. The DHF measurements showed a bias of +0.413 °C compared with those of the TRec. The limits of agreement were broader than the pre-defined ±0.5 °C range (-0.741 °C and +1.567 °C). Although the DHF sensors tended to overestimate the core temperature compared to the rectal measurements, an error grid analysis demonstrated that 95.81% of the DHF measurements would not have led to a wrong clinical decision, e.g., warming or cooling when not necessary. In conclusion, the low number of measurements that would have led to incorrect decisions suggests that the DHF sensor can be considered an option for continuous temperature measurement when more invasive methods are infeasible.
Keywords: anesthesia; hypothermia; pediatric; perioperative care; temperature management; temperature measurement.
Conflict of interest statement
O.K. was a member of the advisory board of ZOLL Medical Österreich GmbH (Vienna, Austria) until 2019. M.Z., M.W., P.M., D.L., F.H., A.G. and S.Z. declare that they have no conflicts of interest.
Figures

Similar articles
-
Zero-heat-flux core temperature monitoring system: an observational secondary analysis to evaluate agreement with naso-/oropharyngeal probe during anesthesia.J Clin Monit Comput. 2020 Oct;34(5):1121-1129. doi: 10.1007/s10877-019-00411-y. Epub 2019 Nov 6. J Clin Monit Comput. 2020. PMID: 31696391
-
Agreement of zero-heat-flux thermometry with the oesophageal and tympanic core temperature measurement in patient receiving major surgery.J Clin Monit Comput. 2024 Feb;38(1):197-203. doi: 10.1007/s10877-023-01078-2. Epub 2023 Oct 4. J Clin Monit Comput. 2024. PMID: 37792140 Free PMC article.
-
Evaluation of the novel non-invasive zero-heat-flux Tcore™ thermometer in cardiac surgical patients.J Clin Monit Comput. 2019 Feb;33(1):165-172. doi: 10.1007/s10877-018-0143-2. Epub 2018 Apr 17. J Clin Monit Comput. 2019. PMID: 29667096
-
Accuracy and precision of zero-heat-flux temperature measurements with the 3M™ Bair Hugger™ Temperature Monitoring System: a systematic review and meta-analysis.J Clin Monit Comput. 2021 Feb;35(1):39-49. doi: 10.1007/s10877-020-00543-6. Epub 2020 Jun 2. J Clin Monit Comput. 2021. PMID: 32488679
-
Skin Temperature Measurement Using Contact Thermometry: A Systematic Review of Setup Variables and Their Effects on Measured Values.Front Physiol. 2018 Jan 30;9:29. doi: 10.3389/fphys.2018.00029. eCollection 2018. Front Physiol. 2018. PMID: 29441024 Free PMC article. Review.
Cited by
-
What is the minimum time interval for reporting of intraoperative core body temperature measurements in pediatric anesthesia? A secondary analysis.J Clin Monit Comput. 2024 Dec 19. doi: 10.1007/s10877-024-01254-y. Online ahead of print. J Clin Monit Comput. 2024. PMID: 39702838
-
Accuracy of non-invasive core temperature monitoring in infant and toddler patients: a prospective observational study.J Anesth. 2024 Dec;38(6):848-854. doi: 10.1007/s00540-024-03404-7. Epub 2024 Sep 11. J Anesth. 2024. PMID: 39256231 Free PMC article.
-
Thermal mapping: Assessing the optimal sites for temperature measurement in the human body and emerging technologies.Physiol Rep. 2024 Jul;12(14):e16155. doi: 10.14814/phy2.16155. Physiol Rep. 2024. PMID: 39039617 Free PMC article. Review.
References
-
- Kiekkas P., Fligou F., Igoumenidis M., Stefanopoulos N., Konstantinou E., Karamouzos V., Aretha D. Inadvertent hypothermia and mortality in critically ill adults: Systematic review and meta-analysis. Aust. Crit. Care Off. J. Confed. Aust. Crit. Care Nurses. 2018;31:12–22. doi: 10.1016/j.aucc.2017.01.008. - DOI - PubMed
-
- Torossian A. AWMF S3 Guidelines on Preventing Inadvertant Perioperative Hypothermia. Deutsche Gesellschaft für Anästhesiologie und Intensivmedizin e.V. (DGAI) 2019. [(accessed on 2 August 2023)]. Available online: https://www.awmf.org/leitlinien/detail/ll/001-018.html.
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

