Drug-Resistant Aspergillus spp.: A Literature Review of Its Resistance Mechanisms and Its Prevalence in Europe
- PMID: 38003770
- PMCID: PMC10674884
- DOI: 10.3390/pathogens12111305
Drug-Resistant Aspergillus spp.: A Literature Review of Its Resistance Mechanisms and Its Prevalence in Europe
Abstract
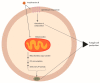
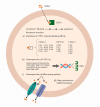
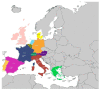
Infections due to the Aspergillus species constitute an important challenge for human health. Invasive aspergillosis represents a life-threatening disease, mostly in patients with immune defects. Drugs used for fungal infections comprise amphotericin B, triazoles, and echinocandins. However, in the last decade, an increased emergence of azole-resistant Aspergillus strains has been reported, principally belonging to Aspergillus fumigatus species. Therefore, both the early diagnosis of aspergillosis and its epidemiological surveillance are very important to establish the correct antifungal therapy and to ensure a successful patient outcome. In this paper, a literature review is performed to analyze the prevalence of Aspergillus antifungal resistance in European countries. Amphotericin B resistance is observed in 2.6% and 10.8% of Aspergillus fumigatus isolates in Denmark and Greece, respectively. A prevalence of 84% of amphotericin B-resistant Aspergillus flavus isolates is reported in France, followed by 49.4%, 35.1%, 21.7%, and 20% in Spain, Portugal, Greece, and amphotericin B resistance of Aspergillus niger isolates is observed in Greece and Belgium with a prevalence of 75% and 12.8%, respectively. The prevalence of triazole resistance of Aspergillus fumigatus isolates, the most studied mold obtained from the included studies, is 0.3% in Austria, 1% in Greece, 1.2% in Switzerland, 2.1% in France, 3.9% in Portugal, 4.9% in Italy, 5.3% in Germany, 6.1% in Denmark, 7.4% in Spain, 8.3% in Belgium, 11% in the Netherlands, and 13.2% in the United Kingdom. The mechanism of resistance is mainly driven by the TR34/L98H mutation. In Europe, no in vivo resistance is reported for echinocandins. Future studies are needed to implement the knowledge on the spread of drug-resistant Aspergillus spp. with the aim of defining optimal treatment strategies.
Keywords: Aspergillus; azole; drug; resistance.
Conflict of interest statement
The author declares no conflict of interest.
Figures



References
-
- Babic N., Gunde-Cimerman N., Vargha M., Tischnner Z., Magyar D., Verissimo C., Sabino R., Viegas C., Meyer W., Brandão J. Fungal contaminants in drinlink water regulaton? A tle of ecology, exposure, purification and clinical relevance. Int. J. Environ. Res. Public Health. 2017;14:636. doi: 10.3390/ijerph14060636. - DOI
-
- Warris A., Klaassen C.H.W., Meis J.F.G.M., de Ruiter M.T., de Valk H.A., Abrahamsen T.G., Gaustad P., Verweij P.E. Molecular epidemiology of Aspergillus fumigatus isolates recovered from water, air, and patients shows two clusters of genetically distinct strains. J. Clin. Microbiol. 2003;41:4101–4106. doi: 10.1128/JCM.41.9.4101-4106.2003. - DOI - PMC - PubMed
-
- Zanganeh E., Zarrinfar H., Rezaeetalab F., Fata A., Tohidi M., Najafzadeh M.J., Alizadeh M., Seyedmousavi S. Predominance of non-fumigatus Aspergillus species among patients suspectedto pulmonary aspergillosis in a tropical and subtropical region of the MiddleEast. Microb. Pathog. 2018;116:296–300. doi: 10.1016/j.micpath.2018.01.047. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

