A multi-center prospective study of plant-based nutritional support in adult community-based patients at risk of disease-related malnutrition
- PMID: 38024371
- PMCID: PMC10667471
- DOI: 10.3389/fnut.2023.1297624
A multi-center prospective study of plant-based nutritional support in adult community-based patients at risk of disease-related malnutrition
Abstract
Introduction: There is an emerging need for plant-based, vegan options for patients requiring nutritional support.
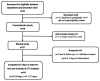
Methods: Twenty-four adults at risk of malnutrition (age: 59 years (SD 18); Sex: 18 female, 6 male; BMI: 19.0 kg/m2 (SD 3.3); multiple diagnoses) requiring plant-based nutritional support participated in a multi-center, prospective study of a (vegan suitable) multi-nutrient, ready-to-drink, oral nutritional supplement (ONS) [1.5 kcal/mL; 300 kcal, 12 g protein/200 mL bottle, mean prescription 275 mL/day (SD 115)] alongside dietary advice for 28 days. Compliance, anthropometry, malnutrition risk, dietary intake, appetite, acceptability, gastrointestinal (GI) tolerance, nutritional goal(s), and safety were assessed.
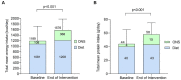
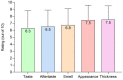
Results: Patients required a plant-based ONS due to personal preference/variety (33%), religious/cultural reasons (28%), veganism/reduce animal-derived consumption (17%), environmental/sustainability reasons (17%), and health reasons (5%). Compliance was 94% (SD 16). High risk of malnutrition ('MUST' score ≥ 2) reduced from 20 to 16 patients (p = 0.046). Body weight (+0.6 kg (SD 1.2), p = 0.02), BMI (+0.2 kg/m2 (SD 0.5), p = 0.03), total mean energy (+387 kcal/day (SD 416), p < 0.0001) and protein intake (+14 g/day (SD 39), p = 0.03), and the number of micronutrients meeting the UK reference nutrient intake (RNI) (7 vs. 14, p = 0.008) significantly increased. Appetite (Simplified Nutritional Appetite Questionnaire (SNAQ) score; p = 0.13) was maintained. Most GI symptoms were stable throughout the study (p > 0.06) with no serious adverse events related.
Discussion: This study highlights that plant-based nutrition support using a vegan-suitable plant-based ONS is highly complied with, improving the nutritional outcomes of patients at risk of malnutrition.
Keywords: disease-related malnutrition; oral nutritional supplement; plant-based diet; plant-based nutritional support; vegan ONS.
Copyright © 2023 Delsoglio, Griffen, Syed, Cookson, Saliba, Vowles, Davies, Willey, Thomas, Millen, Odeh, Longstaff, Westran, Allan, Offer, Howell, Sanders, Gaffigan, Garrett, Foster, Salt, Carter, Moore, Bergin, Roper, Alvarez, Voss, Connolly, MacDonald, Thrower, Sills, Baxter, Manning, Gray, Voas, Richardson, Hurren, Murphy, Blake, McArdle, Walsh, Booth, Albrich, Ashley-Maguire, Allison, Brook, Capener, Hubbard and Stratton.
Conflict of interest statement
MD, CG, RC, GPH and RJS were employed by Nutricia Ltd. The authors declare that this study received funding from Nutricia Ltd. The funder had the following involvement in the study: study design, data analysis, preparation of the manuscript and decision to publish. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures



References
-
- Elia M. Screening for malnutrition: a multidisciplinary responsibility. Development and use of the ‘malnutrition universal screening tool’ (‘MUST’) for adults Malnutrition Advisory Group (MAG), a Standing Committee of BAPEN; (2003).
-
- Stratton RJ, Green CJ, Elia M. Disease-related malnutrition: an evidence-based approach to treatment. Oxford: CABI publishing; (2003).
-
- Ljungqvist O, Man F. Under nutrition: a major health problem in Europe. Nutri Hosp. (2009) 24:369–70. - PubMed
-
- Russell C.A., Elia M. (2015). Nutrition screening surveys in care homes in the UK, 2007–2011. Available at: https://malnutritionandfoodfirst.rdash.nhs.uk/wp-content/uploads/2020/11... (Accessed January 5, 2021)
LinkOut - more resources
Full Text Sources

