Facet joint disorders: from diagnosis to treatment
- PMID: 38072795
- PMCID: PMC10764212
- DOI: 10.3344/kjp.23228
Facet joint disorders: from diagnosis to treatment
Abstract
One of the most common sources of spinal pain syndromes is the facet joints. Cervical, thoracic, and lumbar facet joint pain syndromes comprise 55%, 42%, and 31% of chronic spinal pain syndromes, respectively. Common facet joint disorders are degenerative disorders, such as osteoarthritis, hypertrophied superior articular process, and facet joint cysts; septic arthritis; systemic and metabolic disorders, such as ankylosing spondylitis or gout; and traumatic dislocations. The facet pain syndrome from osteoarthritis is suspected from a patient's history (referred pain pattern) and physical examination (tenderness). Other facet joint disorders may cause radicular pain if mass effect from a facet joint cyst, hypertrophied superior articular process, or tumors compress the dorsal root ganglion. However, a high degree of morphological change does not always provoke pain. The superiority of innervating nerve block or direct joint injection for diagnosis and treatment is still a controversy. Treatment includes facet joint injection in facet joint osteoarthritis or whiplash injury provoking referred pain or decompression in mass effect in cases of hypertrophied superior articular process or facet joint cyst eliciting radicular pain. In addition, septic arthritis is treated using a proper antibiotic, based on infected tissue or blood culture. This review describes the diagnosis and treatment of common facet joint disorders.
Keywords: Arthritis; Ganglia; Hypertrophy; Infectious; Intervertebral Disc; Osteoarthritis; Pain; Physical Examination; Referred; Spinal; Synovial Cyst; Weight-Bearing; Zygapophyseal Joint.
Conflict of interest statement
Kyung-Hoon Kim is an editorial board member of the Korean Journal of Pain; however, he has not been involved in the peer reviewer selection, evaluation, or decision process of this article. No other potential conflict of interest relevant to this article was reported.
Figures

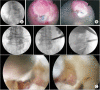
References
-
- Kim KH, Kim DH. In: Minimally invasive percutaneous spinal techniques. 1st ed. Kim DH, Kim KH, Kim YC, editors. Elsevier Saunders; 2011. Diagnosis and treatment of spinal pain; pp. 1–28. - DOI
Publication types
LinkOut - more resources
Full Text Sources
Research Materials

