Management Strategies in Arrhythmogenic Cardiomyopathy across the Spectrum of Ventricular Involvement
- PMID: 38137480
- PMCID: PMC10740984
- DOI: 10.3390/biomedicines11123259
Management Strategies in Arrhythmogenic Cardiomyopathy across the Spectrum of Ventricular Involvement
Abstract
Improved disease recognition through family screening and increased life expectancy with appropriate sudden cardiac death prevention has increased the burden of heart failure in arrhythmogenic cardiomyopathy (ACM). Heart failure management guidelines are well established but primarily focus on left ventricle function. A significant proportion of patients with ACM have predominant or isolated right ventricle (RV) dysfunction. Management of RV dysfunction in ACM lacks evidence but requires special considerations across the spectrum of heart failure regarding the initial diagnosis, subsequent management, monitoring for progression, and end-stage disease management. In this review, we discuss the unique aspects of heart failure management in ACM with a special focus on RV dysfunction.
Keywords: arrhythmogenic cardiomyopathy; arrhythmogenic right ventricular cardiomyopathy; guideline-directed medical therapy; heart failure.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

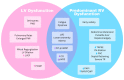


References
-
- Corrado D., Basso C., Thiene G., McKenna W.J., Davies M.J., Fontaliran F., Nava A., Silvestri F., Blomstrom-Lundqvist C., Wlodarska E.K., et al. Spectrum of clinicopathologic manifestations of arrhythmogenic right ventricular cardiomyopathy/dysplasia: A multicenter study. J. Am. Coll. Cardiol. 1997;30:1512–1520. doi: 10.1016/S0735-1097(97)00332-X. - DOI - PubMed
-
- Marcus F.I., Fontaine G.H., Guiraudon G., Frank R., Laurenceau J.L., Malergue C. Myocarditis Cardiomyopathy. Springer; Berlin/Heidelberg, Germany: 1983. Right ventricular dysplasia: A report of 24 adult cases; pp. 81–93. - DOI
Publication types
LinkOut - more resources
Full Text Sources

