Follicle development and its prediction in patients with primary ovarian insufficiency: Possible treatments and markers to maximize the ability to conceive with residual follicles
- PMID: 38144239
- PMCID: PMC10746865
- DOI: 10.1002/rmb2.12556
Follicle development and its prediction in patients with primary ovarian insufficiency: Possible treatments and markers to maximize the ability to conceive with residual follicles
Abstract
Background: Primary ovarian insufficiency (POI) is characterized by the development of hypergonadotropic hypogonadism before 40 years of age and leads to intractable infertility. Although in vitro fertilization and embryo transfer with donated eggs enables pregnancy, not a few patients desire pregnancy using their oocytes. However, follicular development is rare and unpredictable in patients with POI. Thus, there is a need for treatments that promote the development of residual follicles and methods to accurately predict infrequent ovulation.
Methods: This review discusses the effects of various treatments for obtaining eggs from POI patients. Furthermore, this study focused a potential marker for predicting follicular growth in patients with POI.
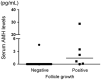
Main findings: Different treatments such as hormone-replacement therapy, dehydroepiandrosterone supplementation, platelet-rich plasma injection, and in vitro activation have shown varying degrees of effectiveness in retrieving oocytes from patients with POI. To predict follicle development in the cycle, elevated serum estradiol and reduced follicle-stimulating hormone (FSH) levels are important. However, these markers are not always reliable under continuous estradiol-replacement therapy. As a novel marker for predicting follicle growth, serum anti-Müllerian hormone (AMH) levels, measured using the picoAMH enzyme-linked immunosorbent assay, were found to predict follicle growth in patients and the cycle.
Conclusion: This review highlights the challenges and available interventions for achieving pregnancy using a patient's oocytes in cases of POI. We believe that a combination of currently available treatments and prediction methods is the best strategy to enable patients with POI to conceive using their own eggs. Although AMH levels may predict follicle growth, further research is necessary to improve the chances of successful follicular development and conception in patients with POI.
Keywords: anti‐Müllerian hormone; enzyme‐linked immunosorbent assay; hypogonadism; premature ovarian failure; primary ovarian insufficiency.
© 2023 The Authors. Reproductive Medicine and Biology published by John Wiley & Sons Australia, Ltd on behalf of Japan Society for Reproductive Medicine.
Conflict of interest statement
Akira Iwase is an Editorial Board member of Reproductive Medicine and Biology and a co‐author of this article. To minimize the bias, he was excluded from all editorial decision‐making related to the acceptance of this article for publication. Akira Iwase and Satoko Osuka have received a grant from Grant in Aid for the Scientific Research (20H0381, 23K08865) related to POI. Akira Iwase is a chairperson of the Reproductive and Endocrine Committee, Japan Society of Obstetrics and Gynecology. There are no conflicts of interest with other authors.
Figures

References
-
- Webber L, Davies M, Anderson R, Bartlett J, Braat D, Cartwright B, et al. ESHRE guideline: management of women with premature ovarian insufficiency. Hum Reprod. 2016;31(5):926–937. - PubMed
-
- Jiao X, Zhang H, Ke H, Zhang J, Cheng L, Liu Y, et al. Premature ovarian insufficiency: phenotypic characterization within different etiologies. J Clin Endocrinol Metab. 2017;102(7):2281–2290. - PubMed
-
- Golezar S, Ramezani Tehrani F, Khazaei S, Ebadi A, Keshavarz Z. The global prevalence of primary ovarian insufficiency and early menopause: a meta‐analysis. Climacteric. 2019;22(4):403–411. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
