Wound healing after therapy of oral potentially malignant disorders with a 445-nm semiconductor laser: a randomized clinical trial
- PMID: 38147181
- PMCID: PMC10751250
- DOI: 10.1007/s00784-023-05438-9
Wound healing after therapy of oral potentially malignant disorders with a 445-nm semiconductor laser: a randomized clinical trial
Abstract
Objectives: Oral potentially malignant disorders (OPMDs) are the most clinically relevant precursor lesions of the oral squamous cell carcinoma (OSCC). OSCC is one of the 15 most common cancers worldwide. OSCC is with its high rate of mortality an important cause of death worldwide. The diagnosis and therapy of clinically relevant precursor lesions of the OSCC is one of the main parts of prevention of this malignant disease. Targeted therapy is one of the main challenges concerning an oncologically safe tissue removal without overwhelming functional and aesthetic impairment.
Materials and methods: In this randomized controlled trial, a newly introduced intraoral 445-nm semiconductor laser (2W; cw-mode; SIROLaser Blue, Dentsply Sirona, Bensheim, Germany) was used in the therapy of OPMDs. Duration and course of wound healing, pain, and scar tissue formation were compared to classical cold blade removal with primary suture by measuring remaining wound area, tissue colorimetry, and visual analogue scale. The study includes 40 patients randomized using a random spreadsheet sequence in two groups (n1 = 20; n2 = 20).
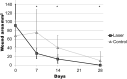
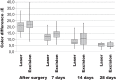
Results: This comparative analysis revealed a significantly reduced remaining wound area after 1, 2, and 4 weeks in the laser group compared to the cold blade group (p < 0.05). In the laser group, a significantly reduced postoperative pain after 1 week was measured (p < 0.05).
Conclusion: Laser coagulation of OPMDs with the investigated 445-nm semiconductor laser is a safe, gentle, and predictable surgical procedure with beneficial wound healing and reduced postoperative discomfort.
Clinical relevance: Compared to the more invasive and bloody cold blade removal with scalpel, the 445-nm semiconductor laser could be a new functional less traumatic tool in the therapy of OPMDs. The method should be further investigated with regard to the identification of further possible indications.
Trail registration: German Clinical Trials Register No: DRKS00032626.
Keywords: Diode laser; Leukoplakia; OPMD; OSCC; Oral precursor lesion; Oral squamous cell carcinoma; Oral surgery.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures


Similar articles
-
Expression of Human Papillomavirus and the p16 Gene in Oral Potentially Malignant Disorders (OPMD): a Comparative Study With Oral Squamous Cell Carcinoma.Appl Immunohistochem Mol Morphol. 2023 May-Jun 01;31(5):331-338. doi: 10.1097/PAI.0000000000001124. Epub 2023 Apr 11. Appl Immunohistochem Mol Morphol. 2023. PMID: 37036407
-
Assessment of serum synuclein-γ and squamous cell carcinoma antigen as diagnostic biomarkers in patients with oral squamous cell carcinoma and oral potentially malignant disorders.J Oral Pathol Med. 2021 Feb;50(2):165-174. doi: 10.1111/jop.13115. Epub 2020 Oct 29. J Oral Pathol Med. 2021. PMID: 33064859
-
Maxillary labial frenectomy: a randomized, controlled comparative study of two blue (445 nm) and infrared (980 nm) diode lasers versus surgical scalpel.BMC Oral Health. 2024 Jul 25;24(1):843. doi: 10.1186/s12903-024-04364-w. BMC Oral Health. 2024. PMID: 39054510 Free PMC article. Clinical Trial.
-
Consensus guidelines on management of oral potentially malignant disorders.Indian J Cancer. 2022 Jul-Sep;59(3):442-453. doi: 10.4103/ijc.IJC_128_21. Indian J Cancer. 2022. PMID: 36412324 Review.
-
Hypovitaminosis D, oral potentially malignant disorders, and oral squamous cell carcinoma: a systematic review.Med Oral Patol Oral Cir Bucal. 2022 Mar 1;27(2):e135-e141. doi: 10.4317/medoral.25049. Med Oral Patol Oral Cir Bucal. 2022. PMID: 35218642 Free PMC article.
Cited by
-
Wound healing and pain evaluation following diode laser surgery vs. conventional scalpel surgery in the surgical treatment of oral leukoplakia: a randomized controlled trial.Front Oral Health. 2025 Mar 3;6:1568425. doi: 10.3389/froh.2025.1568425. eCollection 2025. Front Oral Health. 2025. PMID: 40098816 Free PMC article.
References
-
- Kaatsch P, Spix C, Hentschel S, Katalinic A, Luttmann S, Stegmaier C, Caspritz S, Cernaj J, Ernst A, Folkerts J (2013) Krebs in Deutschland 2009/2010; 9. Ausgabe. Robert Koch-Institut (Hrsg) und die Gesellschaft der epidemiologischen Krebsregister in Deutschland e.V. (Hrsg), Berlin
-
- Sobin LH, Gospodarowicz MK, Wittekind C and International Union against Cancer (2010) TNM classification of malignant tumours. Wiley-Blackwell, Chichester, West Sussex, UK; Hoboken, NJ
-
- Sobin LH, Wittekind C and International Union against Cancer (2002) TNM: classification of malignant tumours. Book title, 6th edn. Wiley-Liss, New York
-
- Kämmerer PW, Morbach T, Schneider D, Liese J. Diagnostik potenziell maligner Mundschleimhautveränderungen in der Zahnarztpraxis. wissen kompakt. 2017;11:105–120. doi: 10.1007/s11838-017-0045-z. - DOI
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

