Prevalence of Obstructive Sleep Apnea Using Home Sleep Test in Taiwan During the Coronavirus Disease Pandemic
- PMID: 38149042
- PMCID: PMC10750777
- DOI: 10.2147/NSS.S434278
Prevalence of Obstructive Sleep Apnea Using Home Sleep Test in Taiwan During the Coronavirus Disease Pandemic
Abstract
Background: Obstructive sleep apnea syndrome (OSAS) is a common disorder associated with serious sequelae. The current gold standard diagnostic method, polysomnography, is costly and time consuming and requires patients to stay overnight at a facility.
Aim: This study aimed to reveal the prevalence of OSAS in general adult population using a home sleep test (HST) during the coronavirus disease 2019 (COVID-19) pandemic.
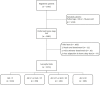
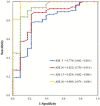
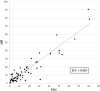
Methods: This prospective cohort study was conducted by the Department of Otolaryngology, Taipei City Hospital, Taipei, Taiwan, between January 2020 and December 2021. A total of 1372 patients aged 30-70 years completed an HST using a Type 3 portable sleep monitor (PM). The apnea-hypopnea index (AHI) was analyzed to assess the association of OSAS with age, body mass index (BMI), sex, Epworth Sleepiness Scale (ESS) and the Sleep Apnea Risk Assessment questionnaire (STOP-Bang questionnaire) rating.
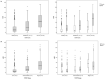
Results: The mean age of the patients (782 men, 57%; 590 women, 43%) was 49.24 ± 11.04 years. OSAS was detected in 954 (69.5%) patients with 399 (29.1%) mild OSAS; 246 (17.9%) moderate OSAS; and 309 (22.5%) severe OSAS. Among these, the prevalence of moderate-to-severe OSAS was 143 (10.4%) in women and 412 (30.0%) in men. The mean age was the highest (51.29 ± 11.29) in the mild OSAS group and lowest (47.08 ± 10.87) in the healthy group. OSAS severity was greater with increasing BMI, 23.39 ± 3.44 in the healthy group and 29.29 ± 5.01 in the severe OSAS group. A positive correlation was also noted between the ESS/STOP-Bang questionnaire rating and OSAS severity.
Conclusion: The prevalence of OSAS in Taiwan was 69.5% in our study. It showed strong evidence that OSAS has important public health consequences and PMs are simple, fast, feasible, and cost-effective tools for OSAS screening in the home environment, especially during the COVID-19 pandemic.
Keywords: COVID-19; apnea-hypopnea index; home sleep test; obstructive sleep apnea; portable sleep monitor.
© 2023 Chou et al.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures
References
LinkOut - more resources
Full Text Sources

