Risk factors for super-refractory and mortality in generalized convulsive status epilepticus: a 10-year retrospective cohort study
- PMID: 38152090
- PMCID: PMC10752052
- DOI: 10.1177/17562864231214846
Risk factors for super-refractory and mortality in generalized convulsive status epilepticus: a 10-year retrospective cohort study
Abstract
Background: Generalized convulsive status epilepticus (GCSE) is one of the most challenging life-threatening neurological emergencies. If GCSE becomes super-refractory, it is associated with significant mortality. Although aggressive management of prolonged status epilepticus was conducted, the mortality has not decreased since the late 1990s.
Objectives: The present study aimed to explore the risk factors for progression to super-refractory in patients with generalized convulsive status epilepticus (GCSE). Moreover, we illustrated the risk factors for mortality in GCSE patients.
Design: An observational retrospective cohort study.
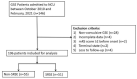
Methods: We conducted a retrospective study of patients with GCSE admitted to our neurocritical unit, in Guangzhou, China, from October 2010 to February 2021. The data of sociodemographic information, etiology, laboratory results, treatment, and prognosis were collected and analyzed.
Results: A total of 106 patients were enrolled; 51 (48%) of them developed super-refractory status epilepticus (SRSE). Multivariate logistic regression analysis demonstrated that patients with autoimmune encephalitis (p = 0.015) and intracranial infection (p = 0.019) are likely to progress to SRSE. The in-hospital mortality was 11.8% and 9.1% for patients in the SRSE and non-SRSE groups, respectively (p = 0.652). Multivariate logistic regression analysis showed that neutrophil-to-lymphocyte ratios (NLR) at admission were independently associated with in-hospital mortality. Up to 31.4% of SRSE patients and 29.1% of non-SRSE patients died within 6 months after discharge (p = 0.798). Multivariate logistic regression analysis showed that plasma exchange (PE) was a protective factor for 6-month mortality. A high NLR at discharge was a risk factor for 6-month mortality.
Conclusion: In the current study, about 48% of GCSE patients progressed to SRSE. Regarding etiology, autoimmune encephalitis or intracranial infection was prone to SRSE. No significant differences were observed in the in-hospital and 6-month mortality between SRSE and non-SRSE groups. Multivariate logistic regression analysis showed that NLR at admission and discharge was an independent predictor of in-hospital and 6-month mortality, respectively. Moreover, PE significantly reduced the 6-month mortality.
Keywords: generalized convulsive status epilepticus/etiology; generalized convulsive status epilepticus/therapy; humans; intensive care unit; outcome.
© The Author(s), 2023.
Conflict of interest statement
The authors declare that there is no conflict of interest.
Figures
Similar articles
-
A Study of Super Refractory Status Epilepticus from India.Front Neurol. 2017 Nov 28;8:636. doi: 10.3389/fneur.2017.00636. eCollection 2017. Front Neurol. 2017. PMID: 29234303 Free PMC article.
-
Super-refractory status epilepticus in West China.Acta Neurol Scand. 2015 Jul;132(1):1-6. doi: 10.1111/ane.12336. Epub 2014 Oct 14. Acta Neurol Scand. 2015. PMID: 25314275
-
Determinants and predictors of outcome in super refractory status epilepticus--a developing country perspective.Epilepsy Res. 2014 Nov;108(9):1609-17. doi: 10.1016/j.eplepsyres.2014.08.010. Epub 2014 Aug 30. Epilepsy Res. 2014. PMID: 25246354
-
Predicting the progression to super-refractory status epilepticus: A machine-learning study.J Neurol Sci. 2022 Dec 15;443:120481. doi: 10.1016/j.jns.2022.120481. Epub 2022 Oct 28. J Neurol Sci. 2022. PMID: 36332322 Review.
-
Pediatric refractory and super-refractory status epilepticus.Seizure. 2019 May;68:62-71. doi: 10.1016/j.seizure.2018.05.012. Epub 2018 May 19. Seizure. 2019. PMID: 29941225 Review.
Cited by
-
The Hemoglobin, Albumin, Lymphocyte, and Platelet (HALP) Score Predicts the Prognosis of Adults with Status Epilepticus: A Retrospective Study.J Inflamm Res. 2024 Nov 25;17:9625-9635. doi: 10.2147/JIR.S491666. eCollection 2024. J Inflamm Res. 2024. PMID: 39618925 Free PMC article.
-
Mortality in patients with epilepsy: a systematic review.J Neurol. 2025 Mar 25;272(4):291. doi: 10.1007/s00415-025-13002-6. J Neurol. 2025. PMID: 40133571 Free PMC article.
-
Predictive value of pan-immune-inflammation value in the prognosis of adults with status epilepticus: a retrospective study.Front Aging Neurosci. 2025 Jul 16;17:1601816. doi: 10.3389/fnagi.2025.1601816. eCollection 2025. Front Aging Neurosci. 2025. PMID: 40741043 Free PMC article.
References
-
- Brophy GM, Bell R, Claassen J, et al.. Guidelines for the evaluation and management of status epilepticus. Neurocrit Care 2012; 17: 3–23. - PubMed
-
- Lowenstein DH, Bleck T, Macdonald RL. It’s time to revise the definition of status epilepticus. Epilepsia 1999; 40: 120–122. - PubMed
-
- Shorvon S. Super-refractory status epilepticus: an approach to therapy in this difficult clinical situation. Epilepsia 2011; 52(Suppl. 8): 53–56. - PubMed
-
- Treiman DM, Walton NY, Kendrick C. A progressive sequence of electroencephalographic changes during generalized convulsive status epilepticus. Epilepsy Res 1990; 5: 49–60. - PubMed
LinkOut - more resources
Full Text Sources