Novel Interventional Radiology for the Treatment of Various Lymphatic Leakages: Lymphatic Intervention and Embolization
- PMID: 38155105
- PMCID: PMC10754830
- DOI: 10.5758/vsi.230082
Novel Interventional Radiology for the Treatment of Various Lymphatic Leakages: Lymphatic Intervention and Embolization
Abstract
Little progress has been made in modern lymphatic medicine since Dr. Kinmonth first described pedal lymphangiography in the 1950s. The clinical need for an effective treatment modality for managing lymphatic leakage greatly increased only after intranodal lymphangiography, which enabled the depiction of the exact location of the leakage. This review introduces five hypotheses that have been proposed while addressing various clinical scenarios involving lymphatic leakage: (1) various embolization techniques can be used to prevent lymphatic leakage; (2) lymph node embolization can treat postoperative pelvic lymphoceles that are refractory to sclerotherapy; (3) the technical success rate of thoracic duct cannulation can be improved by using retrograde thoracic duct access as a bail-out method; (4) non-traumatic chylothorax can be managed by understanding the underlying pathophysiology; and (5) chylous ascites can be managed by understanding the underlying pathophysiology. Five retrospective observational studies, one randomized prospective clinical trial, and two case reports (letters to the editor) were published after the hypotheses were validated. We provide a new systematic approach to lymphatic intervention by describing the process of the current comprehensive research.
Keywords: Chylous; Lymph; Lymphangiography; Lymphatic system; Therapeutic embolization.
Conflict of interest statement
The author has nothing to disclose.
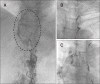
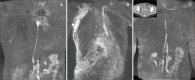
Figures




Similar articles
-
Novel interventional radiological management for lymphatic leakages after gynecologic surgery: lymphangiography and embolization.Gland Surg. 2021 Mar;10(3):1260-1267. doi: 10.21037/gs-2019-ursoc-10. Gland Surg. 2021. PMID: 33842273 Free PMC article. Review.
-
Thoracic duct embolization in treating postoperative chylothorax: does bail-out retrograde access improve outcomes?Eur Radiol. 2022 Jan;32(1):377-383. doi: 10.1007/s00330-021-08145-9. Epub 2021 Jul 10. Eur Radiol. 2022. PMID: 34247305
-
Retrograde transvenous lymphatic embolization for postoperative chylous ascites: A report of three cases and literature review.Radiol Case Rep. 2020 Jul 13;15(9):1623-1628. doi: 10.1016/j.radcr.2020.06.052. eCollection 2020 Sep. Radiol Case Rep. 2020. PMID: 32685083 Free PMC article.
-
Interventional treatment of refractory non-traumatic chylous effusions in patients with lymphoproliferative disorders.Clin Exp Med. 2024 Mar 30;24(1):63. doi: 10.1007/s10238-024-01312-4. Clin Exp Med. 2024. PMID: 38554229 Free PMC article.
-
Chylous Ascites and Lymphoceles: Evaluation and Interventions.Semin Intervent Radiol. 2020 Aug;37(3):274-284. doi: 10.1055/s-0040-1713445. Epub 2020 Jul 31. Semin Intervent Radiol. 2020. PMID: 32773953 Free PMC article. Review.
Cited by
-
Role of Lipiodol® lymphangiography in the diagnosis and management of post-operative chylous ascites.Front Radiol. 2025 Jun 2;5:1537744. doi: 10.3389/fradi.2025.1537744. eCollection 2025. Front Radiol. 2025. PMID: 40530349 Free PMC article.
References
-
- Mortimer PS, Rockson SG. New developments in clinical aspects of lymphatic disease. J Clin Invest. 2014;124:915–921. doi: 10.1172/JCI71608. https://doi.org/10.1172/JCI71608. - DOI - PMC - PubMed
-
- Kinmonth JB, Taylor GW, Harper RK. Lymphangiography; a technique for its clinical use in the lower limb. Br Med J. 1955;1:940–942. doi: 10.1136/bmj.1.4919.940. https://doi.org/10.1136/bmj.1.4919.940. - DOI - PMC - PubMed
-
- Cope C, Salem R, Kaiser LR. Management of chylothorax by percutaneous catheterization and embolization of the thoracic duct: prospective trial. J Vasc Interv Radiol. 1999;10:1248–1254. doi: 10.1016/S1051-0443(99)70227-7. https://doi.org/10.1016/s1051-0443(99)70227-7. - DOI - PubMed
-
- Rajebi MR, Chaudry G, Padua HM, Dillon B, Yilmaz S, Arnold RW, et al. Intranodal lymphangiography: feasibility and preliminary experience in children. J Vasc Interv Radiol. 2011;22:1300–1305. doi: 10.1016/j.jvir.2011.05.003. https://doi.org/10.1016/j.jvir.2011.05.003. - DOI - PubMed
-
- Alejandre-Lafont E, Krompiec C, Rau WS, Krombach GA. Effectiveness of therapeutic lymphography on lymphatic leakage. Acta Radiol. 2011;52:305–311. doi: 10.1258/ar.2010.090356. https://doi.org/10.1258/ar.2010.090356. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

