Current trends of minimally invasive therapy for cholecystocholedocholithiasis
- PMID: 38155666
- PMCID: PMC10753828
- DOI: 10.3389/fmed.2023.1277410
Current trends of minimally invasive therapy for cholecystocholedocholithiasis
Abstract
Introduction: The minimally invasive approach of endoscopic ultrasound (EUS)-guided procedures for cholecystocholedocholithiasis, such as EUS-guided gallbladder drainage (EUS-GBD), EUS-guided rendezvous (EUS-RV), and EUS-guided biliary drainage (EUS-BD), is affirmed as an effective treatment for patients with acute cholecystitis (AC) who are unfit for surgery and for patients with common bile duct stones (CBDSs) who have experienced a previous ERCP failure. Furthermore, in cases of difficult CBDS extraction during endoscopic retrograde cholangiopancreatography (ERCP), cholangioscopy-guided electrohydraulic lithotripsy (CS-EHL) has showed optimal results. The main objective of our study was to evaluate the effectiveness of EUS-GBD and percutaneous gallbladder drainage (PT-GBD) in patients with AC who are unfit for surgery. We also aimed to evaluate the efficacy of EUS-GBD, EUS-BD, and EUS-RV following ERCP failure and the effectiveness of CS-EHL for difficult CBDS extraction in our hospital. The secondary aim was to examine the safety of these procedures.
Materials and methods: We conducted a retrospective evaluation of all the EUS-GBD, PT-GBD, EUS-BD, EUS-RV, and CS-EHL procedures, which were prospectively collected in the gastroenterology and digestive endoscopy unit and the general surgery unit from January 2020 to June 2023. The efficacy was expressed in terms of technical and clinical success rates, while safety was assessed based on the rate of adverse events (AEs).
Results: We enrolled 83 patients with AC and high surgical risk. Among them, 57 patients (68.7%, 24/57 male, median age 85 ± 11 years) underwent EUS-GBD, and 26 (31.3%, 19/26 male, median age 83 ± 7 years) underwent PT-GBD. The technical and clinical success rates were 96.5 and 100% for EUS-GBD, and 96.1 and 92% for PT-GBD. The AEs for EUS-GBD were 1.7%, and for PT-GBD, it was 12%. ERCP for CBDS extraction failed in 77 patients. Among them, 73 patients (94.8%) underwent EUS-RV with technical and clinical success rates of 72.6% (53/73) and 100%, respectively. No AEs were reported. Four out of 77 patients were directly treated with EUS-BD for pyloric inflammatory stenosis. In 12 patients (16.4%), following unsuccessful EUS-RV with a CBD diameter ≥ 12 mm, an EUS-BD was performed. Both technical and clinical success rates for EUS-BD were 100%, and no AEs were reported. EUS-GBD was the treatment of choice for the remaining 8 (10.9%) patients after failure of both ERCP and EUS-RV. The procedure had high technical and clinical success rates (both at 100%), and no AEs were reported. The 12 difficult CBDS extraction treated with CS-EHL also showed high technical and clinical success rates (both at 100%), with no reported AEs.
Conclusion: The minimally invasive approach for cholecystocholedocholithiasis, especially EUS-guided procedures, had high efficacy and safety in treating AC in high-risk surgical patients and CBDS extraction after a previously unsuccessful ERCP.
Keywords: cholangioscopy; cholecystocholedocholithiasis; endoscopic retrograde cholangiopancreatography; endoscopic ultrasound-guided drainage; gallbladder drainage.
Copyright © 2023 Cominardi, Aragona, Cattaneo, Arzù, Capelli and Banchini.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
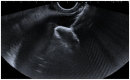
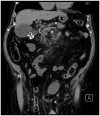
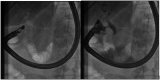
References
LinkOut - more resources
Full Text Sources

