Gastric adenocarcinoma of the fundic gland type: A review of the literature
- PMID: 38162862
- PMCID: PMC10757499
- DOI: 10.1002/jgh3.13014
Gastric adenocarcinoma of the fundic gland type: A review of the literature
Abstract
Background and aim: Gastric adenocarcinoma of the fundic gland type (GA-FG) is a newly described tumor entity but lacking consensus. This review summarizes the key features and controversies regarding this uncommon neoplasm.
Methods: We reviewed studies on GA-FG published in English from 2007 to 2021.
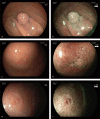
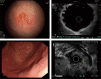
Results: We found that 327 cases (340 lesions) have been reported. GA-FG lesions originate from deep layers of the gastric mucosa, with the following characteristics on conventional white-light endoscopy examination. These lesions, macroscopically identified as submucosal tumor-like 0-IIa, tend to have a whitish discoloration without inflammation, atrophy, or intestinal metaplasia in the background mucosa. Tumors located in the upper third of the stomach are usually solitary, with an average size <10 mm. Contrastingly, magnifying endoscopy with narrow-band imaging mostly shows the absence of any demarcation line, with a regular microvascular pattern and regular microsurface pattern. GA-FGs are covered with normal foveolar epithelium, forming a so-called endless glands pattern in the deeper region, which are mainly composed of chief cells or parietal cells. Most tumors exhibit submucosal invasion, but lymphovascular invasion and nodal metastasis are rare. Regarding the treatment of GA-FG, endoscopic submucosal dissection (ESD) and endoscopic mucosal resection (EMR) are effective treatment methods.
Conclusions: GA-FG is a rare tumor that typically follows a benign course. This neoplasm has distinct endoscopic and pathological features and could be treated by ESD or EMR.
Keywords: chief cell; endoscopic mucosal resection; endoscopic submucosal dissection; gastric adenocarcinoma of the fundic gland type; magnifying endoscopy with narrow‐band imaging.
© 2023 The Authors. JGH Open published by Journal of Gastroenterology and Hepatology Foundation and John Wiley & Sons Australia, Ltd.
Figures
Similar articles
-
Gastric adenocarcinoma of the fundic gland type: clinicopathological features of eight patients treated with endoscopic submucosal dissection.Diagn Pathol. 2020 Oct 23;15(1):131. doi: 10.1186/s13000-020-01047-2. Diagn Pathol. 2020. PMID: 33097069 Free PMC article.
-
Gastric adenocarcinoma of the fundic gland (chief cell-predominant type): A review of endoscopic and clinicopathological features.World J Gastroenterol. 2016 Dec 28;22(48):10523-10531. doi: 10.3748/wjg.v22.i48.10523. World J Gastroenterol. 2016. PMID: 28082804 Free PMC article. Review.
-
Endoscopic submucosal dissection for gastric adenocarcinoma of the fundic gland type (chief cell predominate type): Four years' experience from a tertiary hospital.J Dig Dis. 2022 Nov;23(11):620-627. doi: 10.1111/1751-2980.13149. Epub 2023 Feb 2. J Dig Dis. 2022. PMID: 36546620
-
Twenty cases of gastric adenocarcinoma of the fundic gland type.Scand J Gastroenterol. 2023 Jul;58(7):744-750. doi: 10.1080/00365521.2022.2164213. Epub 2023 Jan 5. Scand J Gastroenterol. 2023. PMID: 36604805
-
Gastric Adenocarcinoma of the Fundic Gland Type: Update and Literature Review.Am J Clin Pathol. 2018 Apr 25;149(6):461-473. doi: 10.1093/ajcp/aqy019. Am J Clin Pathol. 2018. PMID: 29648578 Review.
Cited by
-
An emerging entity of gastric adenocarcinoma: clinicopathological features and differential diagnosis of gastric adenocarcinoma of fundic-gland type in 25 retrospective cases.Virchows Arch. 2025 Mar 18. doi: 10.1007/s00428-025-04075-9. Online ahead of print. Virchows Arch. 2025. PMID: 40100386
-
Diagnostic challenges of rarely well-differentiated adenocarcinoma of the stomach.Pathol Oncol Res. 2025 Jul 7;31:1612163. doi: 10.3389/pore.2025.1612163. eCollection 2025. Pathol Oncol Res. 2025. PMID: 40692725 Free PMC article.
-
Oxyntic Gland Neoplasms - From Adenoma to Advanced Gastric Cancer: A Review of 29 Cases.J Gastric Cancer. 2024 Oct;24(4):378-390. doi: 10.5230/jgc.2024.24.e30. J Gastric Cancer. 2024. PMID: 39375054 Free PMC article.
References
-
- Nakamura K, Sugano H, Takagi K. Carcinoma of the stomach in incipient phase: its histogenesis and histological appearances. Gan. 1968; 59: 251–258. - PubMed
-
- Tsukamoto T, Yokoi T, Maruta S et al. Gastric adenocarcinoma with chief cell differentiation. Pathol. Int. 2007; 57: 517–522. - PubMed
-
- Ueyama H, Yao T, Nakashima Y et al. Gastric adenocarcinoma of fundic gland type (chief cell predominant type): proposal for a new entity of gastric adenocarcinoma. Am. J. Surg. Pathol. 2010; 34: 609–619. - PubMed
-
- Singhi AD, Lazenby AJ. Gastric adenocarcinoma with chief cell differentiation. Am. J. Surg. Pathol. 2012; 36: 6. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

