Association of COVID-19 Vaccinations With Flares of Systemic Rheumatic Disease: A Case-Crossover Study
- PMID: 38163750
- PMCID: PMC11039379
- DOI: 10.1002/acr.25288
Association of COVID-19 Vaccinations With Flares of Systemic Rheumatic Disease: A Case-Crossover Study
Abstract
Objective: We aimed to determine the association of COVID-19 vaccination with flares of systemic rheumatic disease (SRD).
Methods: Adults with systemic rheumatic disease (SRD) in a single-center COVID-19 Rheumatology Registry were invited to enroll in a study of flares. COVID-19 vaccine information from March 5, 2021, to September 6, 2022, was obtained from chart review and self-report. Participants self-reported periods of SRD flare and periods without SRD flare. "Hazard periods" were defined as the time before a self-report of flare and "control periods" as the time before a self-report of no flare. The association between flare and COVID-19 vaccination was evaluated during hazard and control periods through univariate conditional logistic regression stratified by participant, using lookback windows of 2, 7, and 14 days.
Results: A total of 434 participants (mean ± SD age 59 ± 13 years, 84.1% female, 81.8% White, 64.5% with inflammatory arthritis, and 27.0% with connective tissue diseases) contributed to both the hazard and control periods and were included in analysis. A total of 1,316 COVID-19 vaccinations were identified (58.5% Pfizer-BioNTech, 39.5% Moderna, and 1.4% Johnson & Johnson); 96.1% of participants received at least one dose and 93.1% at least two doses. There was no association between COVID-19 vaccination and flares in the subsequent 2, 7, or 14 days (odds ratio [OR] 1.46, 95% confidence interval [CI] 0.86-2.46; OR 1.09, 95% CI 0.76-1.55; and OR 0.85, 95% CI 0.64-1.13, respectively). Analyses stratified on sex, age, SRD subtype, and vaccine manufacturer similarly showed no association between vaccination and flare.
Conclusion: COVID-19 vaccination was not associated with flares in this cohort of participants with SRD. These data are reassuring and can inform shared decision-making on COVID-19 immunization.
© 2024 American College of Rheumatology.
Figures
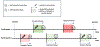
Similar articles
-
Flares of Systemic Autoimmune Rheumatic Disease Following Coronavirus Disease 2019 Vaccination: A Narrative Review.Rheum Dis Clin North Am. 2025 Feb;51(1):75-92. doi: 10.1016/j.rdc.2024.08.005. Epub 2024 Oct 15. Rheum Dis Clin North Am. 2025. PMID: 39550108 Review.
-
Association of COVID-19 vaccinations with osteoarthritis flares: A case-crossover study.Osteoarthritis Cartilage. 2025 Apr;33(4):500-508. doi: 10.1016/j.joca.2024.12.010. Epub 2025 Jan 22. Osteoarthritis Cartilage. 2025. PMID: 39855291
-
Baseline factors associated with self-reported disease flares following COVID-19 vaccination among adults with systemic rheumatic disease: results from the COVID-19 global rheumatology alliance vaccine survey.Rheumatology (Oxford). 2022 Jun 28;61(SI2):SI143-SI150. doi: 10.1093/rheumatology/keac249. Rheumatology (Oxford). 2022. PMID: 35460240 Free PMC article.
-
Factors associated with disease flare following SARS-CoV-2 vaccination in people with inflammatory rheumatic and musculoskeletal diseases: results from the physician-reported EULAR Coronavirus Vaccine (COVAX) Registry.Ann Rheum Dis. 2024 Oct 21;83(11):1584-1595. doi: 10.1136/ard-2024-225869. Ann Rheum Dis. 2024. PMID: 38816065 Free PMC article.
-
The Flare of Rheumatic Disease After SARS-CoV-2 Vaccination: A Review.Front Immunol. 2022 Jul 4;13:919979. doi: 10.3389/fimmu.2022.919979. eCollection 2022. Front Immunol. 2022. PMID: 35860285 Free PMC article. Review.
Cited by
-
Flares of Systemic Autoimmune Rheumatic Disease Following Coronavirus Disease 2019 Vaccination: A Narrative Review.Rheum Dis Clin North Am. 2025 Feb;51(1):75-92. doi: 10.1016/j.rdc.2024.08.005. Epub 2024 Oct 15. Rheum Dis Clin North Am. 2025. PMID: 39550108 Review.
-
Association of COVID-19 vaccinations with osteoarthritis flares: A case-crossover study.Osteoarthritis Cartilage. 2025 Apr;33(4):500-508. doi: 10.1016/j.joca.2024.12.010. Epub 2025 Jan 22. Osteoarthritis Cartilage. 2025. PMID: 39855291
References
-
- Organization WH. WHO Coronavirus (COVID-19) Dashboard 2023 [updated September 27, 2023]. Available from: https://covid19.who.int.
-
- Machado PM, Lawson-Tovey S, Strangfeld A, et al. Safety of vaccination against SARS-CoV-2 in people with rheumatic and musculoskeletal diseases: results from the EULAR Coronavirus Vaccine (COVAX) physician-reported registry. Ann Rheum Dis. 2022;81:695–709. - PubMed
-
- Furer V, Eviatar T, Zisman D, et al. Immunogenicity and safety of the BNT162b2 mRNA COVID-19 vaccine in adult patients with autoimmune inflammatory rheumatic diseases and in the general population: a multicentre study. Ann Rheum Dis. 2021;80:1330–8. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

