Outcomes following major thoracoabdominal cancer resection in adults with congenital heart disease
- PMID: 38165963
- PMCID: PMC10760660
- DOI: 10.1371/journal.pone.0295767
Outcomes following major thoracoabdominal cancer resection in adults with congenital heart disease
Abstract
Background: While advances in medical and surgical management have allowed >97% of congenital heart disease (CHD) patients to reach adulthood, a growing number are presenting with non-cardiovascular malignancies. Indeed, adults with CHD are reported to face a 20% increase in cancer risk, relative to others, and cancer has become the fourth leading cause of death among this population. Surgical resection remains a mainstay in management of thoracoabdominal cancers. However, outcomes following cancer resection among these patients have not been well established. Thus, we sought to characterize clinical and financial outcomes following major cancer resections among adult CHD patients.
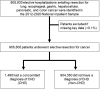
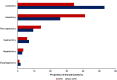
Methods: The 2012-2020 National Inpatient Sample was queried for all adults (CHD or non-CHD) undergoing lobectomy, esophagectomy, gastrectomy, pancreatectomy, hepatectomy, or colectomy for cancer. To adjust for intergroup differences in baseline characteristics, entropy balancing was applied to generate balanced patient groups. Multivariable models were constructed to assess outcomes of interest.
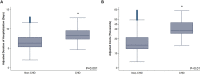
Results: Of 905,830 patients undergoing cancer resection, 1,480 (0.2%) had concomitant CHD. The overall prevalence of such patients increased from <0.1% in 2012 to 0.3% in 2012 (P for trend<0.001). Following risk adjustment, CHD was linked with greater in-hospital mortality (AOR 2.00, 95%CI 1.06-3.76), as well as a notable increase in odds of stroke (AOR 8.94, 95%CI 4.54-17.60), but no statistically significant difference in cardiac (AOR 1.33, 95%CI 0.69-2.59) or renal complications (AOR 1.35, 95%CI 0.92-1.97). Further, CHD was associated with a +2.39 day incremental increase in duration of hospitalization (95%CI +1.04-3.74) and a +$11,760 per-patient increase in hospitalization expenditures (95%CI +$4,160-19,360).
Conclusions: While a growing number of patients with CHD are undergoing cancer resection, they demonstrate inferior clinical and financial outcomes, relative to others. Novel screening, risk stratification, and perioperative management guidelines are needed for these patients to provide evidence-based recommendations for this complex and unique cohort.
Copyright: © 2024 Sakowitz et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

Similar articles
-
Major elective non-cardiac operations in adults with congenital heart disease.Heart. 2023 Jan 11;109(3):202-207. doi: 10.1136/heartjnl-2022-321512. Heart. 2023. PMID: 36175113
-
Association of chronic kidney disease with acute clinical outcomes and hospitalization costs of cancer resection.PLoS One. 2025 Jan 24;20(1):e0317085. doi: 10.1371/journal.pone.0317085. eCollection 2025. PLoS One. 2025. PMID: 39854408 Free PMC article.
-
The Association Between Race and Adverse Postoperative Outcomes in Children With Congenital Heart Disease Undergoing Noncardiac Surgery.Anesth Analg. 2022 Feb 1;134(2):357-368. doi: 10.1213/ANE.0000000000005571. Anesth Analg. 2022. PMID: 33999011
-
Cancer Risk in Congenital Heart Disease-What Is the Evidence?Can J Cardiol. 2019 Dec;35(12):1750-1761. doi: 10.1016/j.cjca.2019.09.023. Epub 2019 Oct 9. Can J Cardiol. 2019. PMID: 31813507 Review.
-
Clinical Outcomes of Acute Myocardial Infarction Hospitalizations With Systemic Lupus Erythematosus: An Analysis of Nationwide Readmissions Database.Curr Probl Cardiol. 2022 Nov;47(11):101086. doi: 10.1016/j.cpcardiol.2021.101086. Epub 2021 Dec 20. Curr Probl Cardiol. 2022. PMID: 34936910 Review.
Cited by
-
Perioperative Risk in Adults with Congenital Heart Disease Undergoing Non-Cardiac Surgery: Challenges and Tailored Strategies.J Clin Med. 2025 May 11;14(10):3340. doi: 10.3390/jcm14103340. J Clin Med. 2025. PMID: 40429336 Free PMC article. Review.
-
Risk of malignancy in adult patients with congenital heart disease: a clinical practice review.Cardiovasc Diagn Ther. 2025 Feb 28;15(1):195-206. doi: 10.21037/cdt-24-388. Epub 2025 Feb 25. Cardiovasc Diagn Ther. 2025. PMID: 40115083 Free PMC article. Review.
References
-
- Karazisi C, Dellborg M, Mellgren K, et al.. Risk of cancer in young and older patients with congenital heart disease and the excess risk of cancer by syndromes, organ transplantation and cardiac surgery: Swedish health registry study (1930−2017). Published online 2022. doi: 10.1016/j.lanepe.2022.100407 - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

