Seroprevalence of hepatitis B, C, and D and associated factors in the semi-isolated Yanomami Amazonian indigenous community
- PMID: 38166687
- PMCID: PMC10762995
- DOI: 10.1186/s12879-023-08928-z
Seroprevalence of hepatitis B, C, and D and associated factors in the semi-isolated Yanomami Amazonian indigenous community
Abstract
Background: Viral hepatitis is a significant health concern among indigenous population in the Americas. In Brazil, reports find high endemicity of HBV and HDV infections has been reported in several indigenous groups. However, few studies have documented the prevalence of HBV, HCV and HDV in the Yanomami. In this study, the prevalence of hepatitis B, C, and D serological markers and potential risk factors were investigated to provide guidance for the development of strategies aimed at reducing viral transmission in the Yanomami indigenous villages.
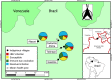
Methods: This cross-sectional study was carried out in March 2015 and included 430 individuals from four Yanomami villages: Alapusi (n = 78), Castanha/Ahima (n = 126), Gasolina (n = 105), and Taibrapa (n = 121). A rapid test was used for detection of HBsAg and anti-HCV and chemiluminescent immunoassay for anti-HBs, anti-HBc, and anti-HDV antibodies.
Results: HBsAg, anti-HBc, and anti-HBs were detected in 8.8, 45.5, and 49.4% of the participants, respectively. The estimated HBV status: current infection 9.6% (38/395); resolved infection 43.3% (171/395); vaccine immunity 20.5% (81/395), and susceptible to HBV 26.6% (105/395). Gasolina presented the lowest prevalence of HBV infection (6.5%) and the highest prevalence of vaccine immunity (26.9%). Children < 15 years old were highly susceptible to infection, as 53.1% did not have antibodies to HBV, while more than 80% of individuals over 45 years of age had been exposed to HBV. The markers for HDV were founded among 12.5% (4/32) of the HBsAg carriers. Anti-HCV was identified in all villages, with the highest prevalence in Alapusi (5.1%). Possible risk factors such as the use of piercings, tattoos, and contact with prospectors showed no statistical difference between the groups.
Conclusions: Viral hepatitis B and serological markers for HCV and HDV were found to be widely distributed among the Yanomami indigenous community, while the prevalence of vaccine immunity to HBV was low. This finding reinforces the importance of promoting systematized diagnostic and vaccination strategies in indigenous communities. Our data confirm that isolated and difficult-to-reach indigenous communities lack appropriate access to diagnosis, treatment, and vaccination.
Keywords: HBV; HCV; HDV; Viral hepatitis; Yanomami.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
Similar articles
-
A comparative epidemiological study of hepatitis B and hepatitis D virus infections in Yanomami and Piaroa Amerindians of Amazonas State, Venezuela.Trop Med Int Health. 2010 Aug;15(8):924-33. doi: 10.1111/j.1365-3156.2010.02560.x. Epub 2010 Jun 15. Trop Med Int Health. 2010. PMID: 20561309
-
[Seroprevalence and Risk Factors of Hepatitis B, C and D in Adults in Trabzon, Türkiye].Mikrobiyol Bul. 2024 Jul;58(3):293-308. doi: 10.5578/mb.20249762. Mikrobiyol Bul. 2024. PMID: 39046211 Turkish.
-
[Prevalence of infections by hepatitis B, C, D and E viruses in Bolivia].Rev Panam Salud Publica. 1999 Mar;5(3):144-51. doi: 10.1590/s1020-49891999000300002. Rev Panam Salud Publica. 1999. PMID: 10355311 Review. Spanish.
-
Hepatitis B, C, and delta in the general population in Mayotte: hepatitis B as a major public health concern.BMC Infect Dis. 2022 Aug 29;22(1):716. doi: 10.1186/s12879-022-07679-7. BMC Infect Dis. 2022. PMID: 36038821 Free PMC article.
-
Epidemiology, Genotype Distribution, Prognosis, Control, and Management of Viral Hepatitis B, C, D, and Hepatocellular Carcinoma in Mongolia.Euroasian J Hepatogastroenterol. 2018 Jan-Jun;8(1):57-62. doi: 10.5005/jp-journals-10018-1260. Epub 2018 May 1. Euroasian J Hepatogastroenterol. 2018. PMID: 29963464 Free PMC article. Review.
References
-
- WHO . Hepatitis B. World Health Organization; 2022.
-
- WHO . Hepatitis C. World Health Organization; 2022.
-
- WHO . Hepatitis D. World Health Organization; 2022.
-
- Brasil. Boletim Epidemiológico de Hepatites Virais 2022. Secretaria de Vigilância em Saúde. Ministério da Saúde do Brasil. Brasília: 2022;Número Especial.
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical