Effect of intraoperative blood loss on postoperative complications and prognosis of patients with colorectal cancer: A meta‑analysis
- PMID: 38169991
- PMCID: PMC10758914
- DOI: 10.3892/br.2023.1710
Effect of intraoperative blood loss on postoperative complications and prognosis of patients with colorectal cancer: A meta‑analysis
Abstract
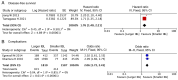
The purpose of the present study was to evaluate whether the amount of intraoperative blood loss (IBL) affects the complications and prognosis of patients with colorectal cancer (CRC). The PubMed, EMBASE and the Cochrane Library databases were used to search for eligible studies from inception to November 30, 2020. Hazard ratios (HRs) and 95% confidence intervals (Cls) were pooled up. The overall survival (OS) and disease-free survival (DFS) were compared between the larger IBL group and the smaller IBL group. The present study was performed with RevMan 5.3 (The Cochrane Collaboration). A total of seven studies involving 1,540 patients with CRC were included in the present study. The smaller IBL group had a higher rate of OS (HR=1.45, 95% CI=1.17 to 1.8, P=0.0007) and a higher rate of DFS (HR=1.76, 95% CI=1.40 to 2.21, P<0.00001). Furthermore, the larger IBL group had a higher rate of postoperative complications than the smaller IBL group (odds ratio=2.06, 95% CI=1.72 to 2.15, P<0.00001). In conclusion, a smaller IBL was associated with better OS and DFS, and a lower risk of postoperative complications compared with a larger IBL in patients with CRC, suggesting that surgeons should pay more attention during perioperative management and surgical operation to reduce IBL.
Keywords: colorectal cancer; complications; disease-free survival; intraoperative blood loss; overall survival.
Copyright: © Li et al.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures


References
-
- Liu XY, Li ZW, Kang B, Cheng YX, Tao W, Zhang B, Zhang H, Wei ZQ, Peng D. Does preoperative waiting time affect the short-term outcomes and prognosis of colorectal cancer patients? A retrospective study from the West of China. Can J Gastroenterol Hepatol. 2022;2022(8235736) doi: 10.1155/2022/8235736. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
