Protein biomarkers GDF15 and FGF21 to differentiate mitochondrial hepatopathies from other pediatric liver diseases
- PMID: 38180987
- PMCID: PMC10781130
- DOI: 10.1097/HC9.0000000000000361
Protein biomarkers GDF15 and FGF21 to differentiate mitochondrial hepatopathies from other pediatric liver diseases
Erratum in
-
Erratum: Protein biomarkers GDF15 and FGF21 to differentiate mitochondrial hepatopathies from other pediatric liver diseases.Hepatol Commun. 2024 Jan 29;8(2):e0390. doi: 10.1097/HC9.0000000000000390. eCollection 2024 Feb 1. Hepatol Commun. 2024. PMID: 38285878 Free PMC article. No abstract available.
Abstract
Background: Mitochondrial hepatopathies (MHs) are primary mitochondrial genetic disorders that can present as childhood liver disease. No recognized biomarkers discriminate MH from other childhood liver diseases. The protein biomarkers growth differentiation factor 15 (GDF15) and fibroblast growth factor 21 (FGF21) differentiate mitochondrial myopathies from other myopathies. We evaluated these biomarkers to determine if they discriminate MH from other liver diseases in children.
Methods: Serum biomarkers were measured in 36 children with MH (17 had a genetic diagnosis); 38 each with biliary atresia, α1-antitrypsin deficiency, and Alagille syndrome; 20 with NASH; and 186 controls.
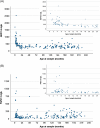
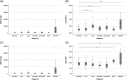
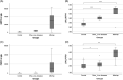
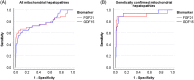
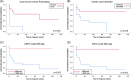
Results: GDF15 levels compared to controls were mildly elevated in patients with α1-antitrypsin deficiency, Alagille syndrome, and biliary atresia-young subgroup, but markedly elevated in MH (p<0.001). FGF21 levels were mildly elevated in NASH and markedly elevated in MH (p<0.001). Both biomarkers were higher in patients with MH with a known genetic cause but were similar in acute and chronic presentations. Both markers had a strong performance to identify MH with a molecular diagnosis with the AUC for GDF15 0.93±0.04 and for FGF21 0.90±0.06. Simultaneous elevation of both markers >98th percentile of controls identified genetically confirmed MH with a sensitivity of 88% and specificity of 96%. In MH, independent predictors of survival without requiring liver transplantation were international normalized ratio and either GDF15 or FGF21 levels, with levels <2000 ng/L predicting survival without liver transplantation (p<0.01).
Conclusions: GDF15 and FGF21 are significantly higher in children with MH compared to other childhood liver diseases and controls and, when combined, were predictive of MH and had prognostic implications.
Copyright © 2024 The Author(s). Published by Wolters Kluwer Health, Inc. on behalf of the American Association for the Study of Liver Diseases.
Conflict of interest statement
Ronald J. Sokol is on advisory committees of Mirum and Albireo and consults with Astellas. Johan L.K. Van Hove has been an advisor to Stealth Biotherapeutics. Philip Rosenthal receives research support from Abbvie, Albireo, Arrowhead, Gilead, Merck, Mirum, Takeda, and Travere, and is a consultant for Albireo, Ambys, Audentes, BioMarin, Dicerna, Encoded, MedinCell, Mirum, Takeda, and Travere. Kathleen M. Loomes participated in advisory committees for Mirum and Albireo, and is a consultant for Travere Therapeutics. Binita M. Kamath is a consultant of Mirum, Albireo, and Audentes, and has unrestricted education grants from Mirum and Albireo. Rene Romero is a consultant for Mirum and Albireo and has a clinical trial with Gilead. Jean P. Molleston receives research funding from Albireo, Abbvie, Mirum, Gilead, and the CF Foundation. Rohit Sharma has equity in bluebird bio. Simon Horslen consults for Albireo, Ipsen and iEcure and received grants from Mirum. Rohit Kohli consults and advises Mirum, Albireo, Sanofi, Epigen, and Intercept. Alexander G. Miethke consults and received grants from Mirum. Pamela L. Valentino is on the speakers’ bureau for Mirum. Shikha S. Sundaram advises Mirum and Albireo. The remaining authors have no conflicts to report.
Figures
References
-
- Gorman GS, Chinnery PF, DiMauro S, Hirano M, Koga Y, McFarland R, et al. . Mitochondrial diseases. Nat Rev Dis Primers. 2016;2:16080. - PubMed
-
- Rahman J, Rahman S. Mitochondrial medicine in the omics era. Lancet. 2018;391:2560–2574. - PubMed
-
- Emmanuele V, Ganesh J, Vladutiu G, Haas R, Kerr D, Saneto RP, et al. and the North American Mitochondrial Disease Consortium (NAMDC) . Time to harmonize mitochondrial syndrome nomenclature and classification: A consensus from the North American Mitochondrial Disease Consortium (NAMDC). Mol Genet Metab. 2022;162:125–131. - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- U01 DK062481/DK/NIDDK NIH HHS/United States
- U01 DK062470/DK/NIDDK NIH HHS/United States
- P30 DK048520/DK/NIDDK NIH HHS/United States
- P30 DK078392/DK/NIDDK NIH HHS/United States
- U54 NS078059/NS/NINDS NIH HHS/United States
- UM1 TR004399/TR/NCATS NIH HHS/United States
- U01 DK103149/DK/NIDDK NIH HHS/United States
- U24 DK062456/DK/NIDDK NIH HHS/United States
- U01 DK103140/DK/NIDDK NIH HHS/United States
- UL1 TR001878/TR/NCATS NIH HHS/United States
- U01 DK084538/DK/NIDDK NIH HHS/United States
- U01 DK062453/DK/NIDDK NIH HHS/United States
- U01 DK062500/DK/NIDDK NIH HHS/United States
- U01 DK062497/DK/NIDDK NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

