Pneumonia in the first week after polytrauma is associated with reduced blood levels of soluble herpes virus entry mediator
- PMID: 38187375
- PMCID: PMC10770833
- DOI: 10.3389/fimmu.2023.1259423
Pneumonia in the first week after polytrauma is associated with reduced blood levels of soluble herpes virus entry mediator
Abstract
Background: Pneumonia develops frequently after major surgery and polytrauma and thus in the presence of systemic inflammatory response syndrome (SIRS) and organ dysfunction. Immune checkpoints balance self-tolerance and immune activation. Altered checkpoint blood levels were reported for sepsis. We analyzed associations of pneumonia incidence in the presence of SIRS during the first week of critical illness and trends in checkpoint blood levels.
Materials and methods: Patients were studied from day two to six after admission to a surgical intensive care unit (ICU). Blood was sampled and physician experts retrospectively adjudicated upon the presence of SIRS and Sepsis-1/2 every eight hours. We measured the daily levels of immune checkpoints and inflammatory markers by bead arrays for polytrauma patients developing pneumonia. Immune checkpoint time series were additionally determined for clinically highly similar polytrauma controls remaining infection-free during follow-up. We performed cluster analyses. Immune checkpoint time trends in cases and controls were compared with hierarchical linear models. For patients with surgical trauma and with and without sepsis, selected immune checkpoints were determined in study baseline samples.
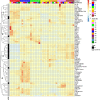
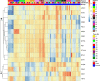
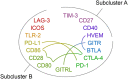
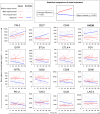
Results: In polytrauma patients with post-injury pneumonia, eleven immune checkpoints dominated subcluster 3 that separated subclusters 1 and 2 of myeloid markers from subcluster 4 of endothelial activation, tissue inflammation, and adaptive immunity markers. Immune checkpoint blood levels were more stable in polytrauma cases than controls, where they trended towards an increase in subcluster A and a decrease in subcluster B. Herpes virus entry mediator (HVEM) levels (subcluster A) were lower in cases throughout. In unselected surgical patients, sepsis was not associated with altered HVEM levels at the study baseline.
Conclusion: Pneumonia development after polytrauma until ICU-day six was associated with decreased blood levels of HVEM. HVEM signaling may reduce pneumonia risk by strengthening myeloid antimicrobial defense and dampening lymphoid-mediated tissue damage. Future investigations into the role of HVEM in pneumonia and sepsis development and as a predictive biomarker should consider the etiology of critical illness and the site of infection.
Keywords: critical illness; herpesvirus entry mediator; immune checkpoint; immunosuppression; pneumonia; polytrauma; sepsis; systemic inflammatory response syndrome.
Copyright © 2023 Schaefer, Lindner, Hahn, Schefzik, Velásquez, Schulte, Fuderer, Centner, Schoettler, Himmelhan, Sturm, Thiel, Schneider-Lindner and Coulibaly.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures



Similar articles
-
Utilizing predictive machine-learning modelling unveils feature-based risk assessment system for hyperinflammatory patterns and infectious outcomes in polytrauma.Front Immunol. 2023 Dec 12;14:1281674. doi: 10.3389/fimmu.2023.1281674. eCollection 2023. Front Immunol. 2023. PMID: 38193076 Free PMC article.
-
Herpesvirus entry mediator on radiation-resistant cell lineages promotes ocular herpes simplex virus 1 pathogenesis in an entry-independent manner.mBio. 2015 Oct 20;6(5):e01532-15. doi: 10.1128/mBio.01532-15. mBio. 2015. PMID: 26489863 Free PMC article.
-
Infections and the inflammatory response in acute respiratory distress syndrome.Chest. 1997 May;111(5):1306-21. doi: 10.1378/chest.111.5.1306. Chest. 1997. PMID: 9149588
-
The epidemiology of the systemic inflammatory response.Intensive Care Med. 2000;26 Suppl 1(Suppl 1):S64-74. doi: 10.1007/s001340051121. Intensive Care Med. 2000. PMID: 10786961 Free PMC article. Review.
-
Microbiome in Critical Care: An Unconventional and Unknown Ally.Curr Med Chem. 2022;29(18):3179-3188. doi: 10.2174/0929867328666210915115056. Curr Med Chem. 2022. PMID: 34525908 Review.
Cited by
-
Identifying biomarkers distinguishing sepsis after trauma from trauma-induced SIRS based on metabolomics data: a retrospective study.Sci Rep. 2025 Apr 21;15(1):13748. doi: 10.1038/s41598-025-94701-y. Sci Rep. 2025. PMID: 40258847 Free PMC article.
-
Biomarkers for pneumonia after major trauma: A systematic review and meta-analysis.J Intensive Care Soc. 2025 Jun 13:17511437251344068. doi: 10.1177/17511437251344068. Online ahead of print. J Intensive Care Soc. 2025. PMID: 40520925 Free PMC article.
References
-
- Fleischmann-Struzek C, Mellhammar L, Rose N, Cassini A, Rudd KE, Schlattmann P, et al. . Incidence and mortality of hospital- and ICU-treated sepsis: results from an updated and expanded systematic review and meta-analysis. Intensive Care Med (2020) 46(8):1552–62. doi: 10.1007/s00134-020-06151-x - DOI - PMC - PubMed
-
- Bone RC, Balk RA, Cerra FB, Dellinger RP, Fein AM, Knaus WA, et al. . Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest (1992) 101(6):1644–55. doi: 10.1378/chest.101.6.1644 - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

