Post-Coronary Artery Bypass Grafting Outcomes of Patients with/without Type-2 Diabetes Mellitus and Chronic Kidney Disease Treated with SGLT2 Inhibitor Dapagliflozin: A Single-Center Experience Analysis
- PMID: 38201325
- PMCID: PMC10871095
- DOI: 10.3390/diagnostics14010016
Post-Coronary Artery Bypass Grafting Outcomes of Patients with/without Type-2 Diabetes Mellitus and Chronic Kidney Disease Treated with SGLT2 Inhibitor Dapagliflozin: A Single-Center Experience Analysis
Abstract
Introduction: Increasingly, SGLT2 inhibitors save patients with heart failure and comorbidities such as type-2 diabetes mellitus (T2DM) and chronic kidney disease (CKD); the inhibition of sodium-glucose cotransporter 2 (SGLT2) was first studied in patients with diabetes as a solution to lower glucose levels by preventing glucose reabsorption and facilitating its elimination; in the process, researchers took notice of how SGLT2 inhibitors also seemed to have beneficial cardiovascular effects in patients with both diabetes and cardiovascular disease.
Aim: Our single-center prospective study assesses outcomes of post-coronary artery bypass grafting (CABG) rehabilitation and SLGT2 inhibition in CABG patients with/without T2DM and with/without CKD.
Materials and methods: One hundred twenty consecutive patients undergoing CABG were included in the analysis. Patients were divided into four subgroups: diabetes patients with chronic kidney disease (T2DM + CKD), diabetes patients without chronic kidney disease (T2DM-CKD), prediabetes patients with chronic kidney disease (PreD+CKD), and prediabetes patients without chronic kidney disease (PreD-CKD). Echocardiographic and laboratory investigations post-surgery (phase I) and 6 months later (phase II) included markers for cardiac ischemia, glycemic status, and renal function, and metabolic equivalents were investigated.
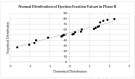
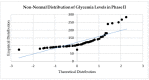
Results: One hundred twenty patients participated, mostly men, overweight/obese, hypertensive, smokers; 65 had T2DM (18 with CKD), and 55 were prediabetic (17 with CKD). The mean ejection fraction increased by 8.43% overall but significantly more in the prediabetes group compared to the T2DM group (10.14% vs. 6.98%, p < 0.05). Overall, mean heart-type fatty-acid-binding protein (H-FABP) levels returned to normal levels, dropping from 68.40 ng/mL to 4.82 ng/mL (p = 0.000), and troponin data were more nuanced relative to an overall, strongly significant decrease of 44,458 ng/L (p = 0.000). Troponin levels in patients with CKD dropped more, both in the presence of T2DM (by 82,500 ng/L, p = 0.000) and in patients without T2DM (by 73,294 ng/L, p = 0.047). As expected, the overall glycated hemoglobin (HbA1c) levels improved significantly in those with prediabetes (from 6.54% to 5.55%, p = 0.000); on the other hand, the mean HbA1c changed from 7.06% to 6.06% (p = 0.000) in T2DM, and the presence or absence of CKD did not seem to make any difference: T2DM+CKD 7.01-6.08% (p = 0.000), T2DM-CKD 7.08-6.04% (p = 0.000), PreD+CKD 5.66-4.98% (p = 0.014), and PreD-CKD 6.03-4.94% (p = 0.00). Compared to an overall gain of 11.51, the GFRs of patients with CKD improved by 18.93 (68.15-87.07%, p = 0.000) in the presence of established diabetes and 14.89 (64.75-79.64%, p = 0.000) in the prediabetes group.
Conclusions: Regarding the patients' cardiac statuses, the results from our single-center analysis revealed a significant decrease in ischemic risk (H-FABP and hs-cTnI levels) with improvements in mean ejection fraction, glycemic status, and renal function in patients post-CABG with/without T2DM, with/without CKD, and with SGLT2 inhibitor dapagliflozin treatment while undergoing cardiac rehabilitation.
Keywords: CABG; H-FABP; SGLT2 inhibitors; heart failure; type-2 diabetes mellitus.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
-
- Verma S., Farkouh M.E., Yanagawa B., Fitchett D.H., Ahsan M.R., Ruel M., Sud S., Gupta M., Singh S., Gupta N., et al. Comparison of coronary artery bypass surgery and percutaneous coronary intervention in patients with diabetes: A meta-analysis of randomised controlled trials. Lancet Diabetes Endocrinol. 2013;1:317–328. doi: 10.1016/S2213-8587(13)70089-5. - DOI - PubMed
-
- Zinman B., Wanner C., Lachin J.M., Fitchett D., Bluhmki E., Hantel S., Mattheus M., Biomath D., Devins T., Johansen O.E., et al. EMPA-REG OUTCOME Investigators. Empagliflozin, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes. N. Engl. J. Med. 2015;373:2117–2128. doi: 10.1056/NEJMoa1504720. - DOI - PubMed
-
- U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and Research Guidance for Industry. Diabetes Mellitus—Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes. [(accessed on 15 October 2023)]; Available online: https://www.fda.gov/media/71297/download.
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous