Hereditary Thoracic Aortic Diseases
- PMID: 38201421
- PMCID: PMC10795846
- DOI: 10.3390/diagnostics14010112
Hereditary Thoracic Aortic Diseases
Abstract
Advances in both imaging techniques and genetics have led to the recognition of a wide variety of aortic anomalies that can be grouped under the term 'hereditary thoracic aortic diseases'. The present review aims to summarize this very heterogeneous population's clinical, genetic, and imaging characteristics and to discuss the implications of the diagnosis for clinical counselling (on sports activity or pregnancy), medical therapies and surgical management.
Keywords: aortic dilation; genetics; hereditary aortopathies; multimodality imaging; thoracic aortic disease.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
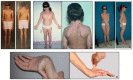
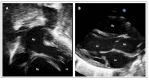
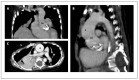
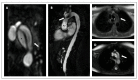
References
-
- Baumgartner H., De Backer J., Babu-Narayan S.V., Budts W., Chessa M., Diller G.-P., Lung B., Kluin J., Lang I.M., Meijboom F., et al. 2020 ESC Guidelines for the management of adult congenital heart disease. The Task Force for the management of adult congenital heart disease of the European Society of Cardiology (ESC) Eur. Heart J. 2021;42:563–645. doi: 10.1093/eurheartj/ehaa554. - DOI - PubMed
-
- Renner S., Schüler H., Alawi M., Kolbe V., Rybczynski M., Woitschach R., Sheikhzadeh S., Stark V.C., Olfe J., Roser E., et al. Next-generation sequencing of 32 genes associated with hereditary aortopathies and related disorders of connective tissue in a cohort of 199 patients. Gen. Med. 2019;21:1832–1841. doi: 10.1038/s41436-019-0435-z. - DOI - PubMed
-
- Isselbacher E.M., Preventza O., Hamilton Black J., 3rd, Augoustides J.G., Beck A.W., Bolen M.A., Braverman A.C., Bray B.E., Brown-Zimmerman M.M., Chen E.P., et al. 2022 ACC/AHA guideline for the diagnosis and management of aortic disease: A report of the American Heart Association/American College of Cardiology Joint Committee on Clinical Practice Guidelines. Circulation. 2022;146:e334–e483. doi: 10.1161/CIR.0000000000001106. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources

