Early Deep Sedation Practices Worsened During the Pandemic Among Adult Patients Without COVID-19: A Retrospective Cohort Study
- PMID: 38218219
- PMCID: PMC11317814
- DOI: 10.1016/j.chest.2024.01.019
Early Deep Sedation Practices Worsened During the Pandemic Among Adult Patients Without COVID-19: A Retrospective Cohort Study
Abstract
Background: There is substantial evidence that patients with COVID-19 were treated with sustained deep sedation during the pandemic. However, it is unknown whether such guideline-discordant care had spillover effects to patients without COVID-19.
Research question: Did patterns of early deep sedation change during the pandemic for patients on mechanical ventilation without COVID-19?
Study design and methods: We used electronic health record data from 4,237 patients who were intubated without COVID-19. We compared sedation practices in the first 48 h after intubation across prepandemic (February 1, 2018, to January 31, 2020), pandemic (April 1, 2020, to March 31, 2021), and late pandemic (April 1, 2021, to March 31, 2022) periods.
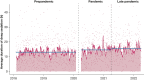
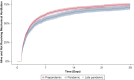
Results: In the prepandemic period, patients spent an average of 13.0 h deeply sedated in the first 48 h after intubation. This increased 1.9 h (95% CI, 1.0-2.8) during the pandemic period and 2.9 h (95% CI, 2.0-3.8) in the late pandemic period. The proportion of patients that spent over one-half of the first 48 h deeply sedated was 18.9% in the prepandemic period, 22.3% during the pandemic period, and 25.9% during the late pandemic period. Ventilator-free days decreased during the pandemic, with a subdistribution hazard ratio of being alive without mechanical ventilation at 28 days of 0.87 (95% CI, 0.79-0.95) compared with the prepandemic period. Tracheostomy placement increased during the pandemic period compared with the prepandemic period (OR, 1.41; 95% CI, 1.08-1.82). In the medical ICU, early deep sedation increased 2.5 h (95% CI, 0.6-4.4) during the pandemic period and 4.9 h (95% CI, 3.0-6.9) during the late pandemic period, compared with the prepandemic period.
Interpretation: We found that among patients on mechanical ventilation without COVID-19, sedation use increased during the pandemic. In the subsequent year, these practices did not return to prepandemic standards.
Keywords: critical care; mechanical ventilation; sedation.
Copyright © 2024 American College of Chest Physicians. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Financial/Nonfinancial Disclosures None declared.
Figures

Similar articles
-
A dual-center cohort study on the association between early deep sedation and clinical outcomes in mechanically ventilated patients during the COVID-19 pandemic: The COVID-SED study.Crit Care. 2022 Jun 15;26(1):179. doi: 10.1186/s13054-022-04042-9. Crit Care. 2022. PMID: 35705989 Free PMC article.
-
Impact of healthcare system strain on the implementation of ICU sedation practices and encephalopathy burden during the early COVID-19 pandemic.Geroscience. 2025 Feb;47(1):189-203. doi: 10.1007/s11357-024-01336-4. Epub 2024 Sep 7. Geroscience. 2025. PMID: 39243283 Free PMC article.
-
A Retrospective, Single-Center Assessment of Changes in Pain, Agitation, and Delirium Management Before and During the COVID-19 Pandemic.Crit Care Explor. 2025 Jan 15;7(1):e1202. doi: 10.1097/CCE.0000000000001202. eCollection 2025 Jan 1. Crit Care Explor. 2025. PMID: 39813020 Free PMC article.
-
Sedation for critically ill patients with COVID-19: Which specificities? One size does not fit all.Anaesth Crit Care Pain Med. 2020 Jun;39(3):341-343. doi: 10.1016/j.accpm.2020.04.010. Epub 2020 Apr 29. Anaesth Crit Care Pain Med. 2020. PMID: 32360979 Free PMC article. Review. No abstract available.
-
Protocol-directed sedation versus non-protocol-directed sedation in mechanically ventilated intensive care adults and children.Cochrane Database Syst Rev. 2018 Nov 12;11(11):CD009771. doi: 10.1002/14651858.CD009771.pub3. Cochrane Database Syst Rev. 2018. PMID: 30480753 Free PMC article.
Cited by
-
The Real-World Effect of Early Screening for Palliative Care Criteria in a Medical Intensive Care Unit: An Instrumental Variable Analysis.Ann Am Thorac Soc. 2025 Feb;22(2):247-254. doi: 10.1513/AnnalsATS.202407-702OC. Ann Am Thorac Soc. 2025. PMID: 39441096
References
-
- Wongtangman K., Santer P., Wachtendorf L.J., et al. Association of sedation, coma, and in-hospital mortality in mechanically ventilated patients with coronavirus disease 2019–related acute respiratory distress syndrome: a retrospective cohort study. Crit Care Med. 2021;49(9):1524–1534. - PubMed
-
- Devlin J.W., Skrobik Y., Gélinas C., et al. Clinical practice guidelines for the prevention and management of pain, agitation/sedation, delirium, immobility, and sleep disruption in adult patients in the ICU. Crit Care Med. 2018;46(9):e825. - PubMed
-
- Halpern S.D., Becker D., Curtis J.R., et al. An Official American Thoracic Society/American Association of Critical-Care Nurses/American College of Chest Physicians/Society of Critical Care Medicine Policy Statement: The Choosing Wisely® Top 5 List in Critical Care Medicine. Am J Respir Crit Care Med. 2014;190(7):818–826. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

