Laparoscopic resection and endoscopic submucosal dissection for treating gastric ectopic pancreas
- PMID: 38222013
- PMCID: PMC10784817
- DOI: 10.4240/wjgs.v15.i12.2799
Laparoscopic resection and endoscopic submucosal dissection for treating gastric ectopic pancreas
Abstract
Background: Gastric ectopic pancreas (GEP) is a rare developmental abnormality that refers to the existence of pancreatic tissue in the stomach with no anatomical relationship with the main pancreas. It is usually difficult to diagnose through histological examination, and the choice of treatment method is crucial.
Aim: To describe the endoscopic ultrasound characteristics of GEP and evaluate the value of laparoscopic resection (LR) and endoscopic submucosal dissection (ESD).
Methods: Forty-nine patients with GEP who underwent ESD and LR in the Second Affiliated Hospital of Fujian Medical University from May 2018 to July 2023 were retrospectively included. Data on clinical characteristics, endoscopic ultrasonography (EUS), ESD, and LR were collected and analyzed. The characteristics of EUS and the efficacy of the two treatments were analyzed.
Results: The average age of the patients was 43.31 ± 13.50 years, and the average maximum diameter of the lesions was 1.55 ± 0.70 cm. The lesion originated from the mucosa in one patient (2.04%), from the submucosa in 42 patients (85.71%), and from the muscularis propria in 6 patients (12.25%). Twenty-nine patients (59.20%) with GEP showed umbilical depression on endoscopy. The most common initial symptom of GEP was abdominal pain (40.82%). Tumor markers, including carcinoembryonic antigen (CEA) and carbohydrate antigen 19-9 (CA-19-9), were generally within the normal range. One patient (2.04%) with GEP had increased CEA and CA-19-9 levels. However, no cancer tissue was found on postoperative pathological examination, and tumor markers returned to normal levels after resecting the lesion. There was no significant difference in surgery duration (72.42 ± 23.84 vs 74.17 ± 12.81 min) or hospital stay (3.70 ± 0.91 vs 3.83 ± 0.75 d) between the two methods. LR was more often used for patients with larger tumors and deeper origins. The amount of bleeding was significantly higher in LR than in ESD (11.28 ± 16.87 vs 16.67 ± 8.76 mL, P < 0.05). Surgery was associated with complete resection of the lesion without any serious complications; there were no cases of recurrence during the follow-up period.
Conclusion: GEP has unique characteristics in EUS. LR and ESD seem to be good choices for treating GEP. LR is better for large GEP with a deep origin. However, due to the rarity of GEP, multicenter large-scale studies are needed to describe its characteristics and evaluate the safety of LR and ESD.
Keywords: Ectopic pancreas; Endoscopic submucosal dissection; Endoscopic ultrasonography; Laparoscopic resection.
©The Author(s) 2023. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: We have no financial relationships to disclose.
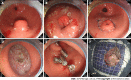
Figures



Similar articles
-
Feasibility of endoscopic submucosal dissection for upper gastrointestinal submucosal tumors treatment and value of endoscopic ultrasonography in pre-operation assess and post-operation follow-up: a prospective study of 224 cases in a single medical center.Surg Endosc. 2016 Oct;30(10):4206-13. doi: 10.1007/s00464-015-4729-1. Epub 2016 Jan 28. Surg Endosc. 2016. PMID: 26823060
-
The effect of endoscopic ultrasound on the precise selection of endoscopic treatment for submucosal tumors in the upper gastrointestinal tract.BMC Surg. 2023 Aug 27;23(1):255. doi: 10.1186/s12893-023-02164-7. BMC Surg. 2023. PMID: 37635257 Free PMC article.
-
Endoscopic submucosal dissection for foregut neuroendocrine tumors: an initial study.World J Gastroenterol. 2012 Oct 28;18(40):5799-806. doi: 10.3748/wjg.v18.i40.5799. World J Gastroenterol. 2012. PMID: 23155323 Free PMC article.
-
AGA Institute Clinical Practice Update: Endoscopic Submucosal Dissection in the United States.Clin Gastroenterol Hepatol. 2019 Jan;17(1):16-25.e1. doi: 10.1016/j.cgh.2018.07.041. Epub 2018 Aug 2. Clin Gastroenterol Hepatol. 2019. PMID: 30077787 Review.
-
Updated evaluation of endoscopic submucosal dissection versus surgery for early gastric cancer: A systematic review and meta-analysis.Int J Surg. 2020 Jan;73:28-41. doi: 10.1016/j.ijsu.2019.11.027. Epub 2019 Nov 26. Int J Surg. 2020. PMID: 31783166
Cited by
-
New frontiers in ectopic pancreatic tissue management.World J Gastrointest Surg. 2024 Apr 27;16(4):1215-1217. doi: 10.4240/wjgs.v16.i4.1215. World J Gastrointest Surg. 2024. PMID: 38690036 Free PMC article.
-
Overview of ectopic pancreas.World J Gastrointest Surg. 2024 Feb 27;16(2):284-288. doi: 10.4240/wjgs.v16.i2.284. World J Gastrointest Surg. 2024. PMID: 38463359 Free PMC article.
References
-
- Barila Lompe P, Gine C, Laín A, Garcia-Martinez L, Diaz Hervas M, López M. Esophageal Atresia and Gastric Ectopic Pancreas: Is There a Real Association? Eur J Pediatr Surg. 2023 - PubMed
-
- Rodríguez-Seguel E, Villamayor L, Arroyo N, De Andrés MP, Real FX, Martín F, Cano DA, Rojas A. Loss of GATA4 causes ectopic pancreas in the stomach. J Pathol. 2020;250:362–373. - PubMed
-
- Trifan A, Târcoveanu E, Danciu M, Huţanaşu C, Cojocariu C, Stanciu C. Gastric heterotopic pancreas: an unusual case and review of the literature. J Gastrointestin Liver Dis. 2012;21:209–212. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

