U-fiber analysis: a toolbox for automated quantification of U-fibers and white matter hyperintensities
- PMID: 38223048
- PMCID: PMC10784071
- DOI: 10.21037/qims-23-847
U-fiber analysis: a toolbox for automated quantification of U-fibers and white matter hyperintensities
Abstract
Background: Whether white matter hyperintensities (WMHs) involve U-fibers is of great value in understanding the different etiologies of cerebral white matter (WM) lesions. However, clinical practice currently relies only on the naked eye to determine whether WMHs are in the vicinity of U-fibers, and there is a lack of good neuroimaging tools to quantify WMHs and U-fibers.
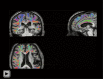
Methods: Here, we developed a multimodal neuroimaging toolbox named U-fiber analysis (UFA) that can automatically extract WMHs and quantitatively characterize the volume and number of WMHs in different brain regions. In addition, we proposed an anatomically constrained U-fiber tracking scheme and quantitatively characterized the microstructure diffusion properties, fiber length, and number of U-fibers in different brain regions to help clinicians to quantitatively determine whether WMHs in the proximal cortex disrupt the microstructure of U-fibers. To validate the utility of the UFA toolbox, we analyzed the neuroimaging data from 246 patients with cerebral small vessel disease (cSVD) enrolled at Zhongshan Hospital between March 2018 and November 2019 in a cross-sectional study.
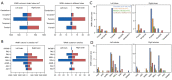
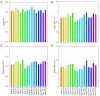
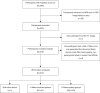
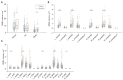
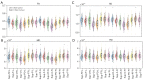
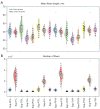
Results: According to the manual judgment of the clinician, the patients with cSVD were divided into a WMHs involved U-fiber group (U-fiber-involved group, 51 cases) and WMHs not involved U-fiber group (U-fiber-spared group, 163 cases). There were no significant differences between the U-fiber-spared group and the U-fiber-involved group in terms of age (P=0.143), gender (P=0.462), education (P=0.151), Mini-Mental State Examination (MMSE) scores (P=0.151), and Montreal Cognitive Assessment (MoCA) scores (P=0.411). However, patients in the U-fiber-involved group had higher Fazekas scores (P<0.001) and significantly higher whole brain WMHs (P=0.046) and deep WMH volumes (P<0.001) compared to patients in the U-fiber-spared group. Moreover, the U-fiber-involved group had higher WMH volumes in the bilateral frontal [P(left) <0.001, P(right) <0.001] and parietal lobes [P(left) <0.001, P(right) <0.001]. On the other hand, patients in the U-fiber-involved group had higher mean diffusivity (MD) and axial diffusivity (AD) in the bilateral parietal [P(left, MD) =0.048, P(right, MD) =0.045, P(left, AD) =0.015, P(right, AD) =0.015] and right frontal-parietal regions [P(MD) =0.048, P(AD) =0.027], and had significantly reduced mean fiber length and number in the right parietal [P(length) =0.013, P(number) =0.028] and right frontal-parietal regions [P(length) =0.048] compared to patients in the U-fiber-spared group.
Conclusions: Our results suggest that WMHs in the proximal cortex may disrupt the microstructure of U-fibers. Our tool may provide new insights into the understanding of WM lesions of different etiologies in the brain.
Keywords: MATLAB toolbox; U-fiber tractography; cerebral small vessel disease (cSVD); diffusion magnetic resonance imaging (dMRI); white matter hyperintensities (WMHs).
2024 Quantitative Imaging in Medicine and Surgery. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://qims.amegroups.com/article/view/10.21037/qims-23-847/coif). The authors have no conflicts of interest to declare.
Figures



References
-
- Schüz A, Miller R. Cortical areas: unity and diversity. London: CRC press; 2002.
-
- Kirilina E, Helbling S, Morawski M, Pine K, Reimann K, Jankuhn S, Dinse J, Deistung A, Reichenbach JR, Trampel R, Geyer S, Müller L, Jakubowski N, Arendt T, Bazin PL, Weiskopf N. Superficial white matter imaging: Contrast mechanisms and whole-brain in vivo mapping. Sci Adv 2020;6:eaaz9281. 10.1126/sciadv.aaz9281 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
