Postoperative systemic inflammatory response syndrome predicts increased mortality in patients after elective craniotomy
- PMID: 38239666
- PMCID: PMC10794578
- DOI: 10.3389/fsurg.2023.1331073
Postoperative systemic inflammatory response syndrome predicts increased mortality in patients after elective craniotomy
Abstract
Introduction: Patients undergoing craniotomy are at high risk of perioperative morbidity and mortality due to excessive inflammatory responses. The purpose of the present study is to evaluate the prognostic utility of postoperative systemic inflammatory response syndrome (SIRS) in patients undergoing craniotomy.
Methods: We performed a retrospective cohort study of patients who underwent craniotomy between January 2011 and March 2021. SIRS was diagnosed based on two or more criteria (hypo-/hyperthermia, tachypnea, leukopenia/leukocytosis, tachycardia). We used univariate and multivariate analysis for the development of SIRS with postoperative 30-day mortality.
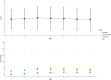
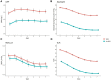
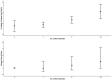
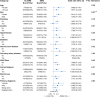
Results: Of 12,887 patients who underwent craniotomy, more than half of the patients (n = 6,725; 52.2%) developed SIRS within the first 7 days after surgery, and 157 (1.22%) patients died within 30 days after surgery. In multivariable analyses, SIRS (OR, 1.57; 95% CI, 1.12-2.21) was associated with 30-day mortality. Early SIRS was not predictive of 30-day mortality, whereas delayed SIRS was predictive of 30-day mortality. Abnormal white blood cell (WBC) counts contributed the most to the SIRS score, followed by abnormal body temperature, respiratory rate, and heart rate.
Conclusion: Postoperative SIRS commonly occurs after craniotomy and is an independent predictor of postoperative 30-day mortality. This association was seen only in delayed SIRS but not early SIRS. Moreover, increased WBC counts contributed the most to the SIRS score.
Keywords: craniotomy; mortality; postoperative; prognosis; systemic inflammatory response syndrome.
© 2024 Peng, Gan, Xiao, He, Cheng, Wang, Chen, Li, He, Chong, Hai, You, Fang and Zhang.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

References
LinkOut - more resources
Full Text Sources

