Aberrant brain-heart coupling is associated with the severity of post cardiac arrest brain injury
- PMID: 38243640
- PMCID: PMC11021613
- DOI: 10.1002/acn3.52000
Aberrant brain-heart coupling is associated with the severity of post cardiac arrest brain injury
Abstract
Objective: To investigate autonomic nervous system activity measured by brain-heart interactions in comatose patients after cardiac arrest in relation to the severity and prognosis of hypoxic-ischemic brain injury.
Methods: Strength and complexity of bidirectional interactions between EEG frequency bands (delta, theta, and alpha) and ECG heart rate variability frequency bands (low frequency, LF and high frequency, HF) were computed using a synthetic data generation model. Primary outcome was the severity of brain injury, assessed by (i) standardized qualitative EEG classification, (ii) somatosensory evoked potentials (N20), and (iii) neuron-specific enolase levels. Secondary outcome was the 3-month neurological status, assessed by the Cerebral Performance Category score [good (1-2) vs. poor outcome (3-4-5)].
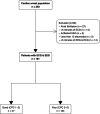
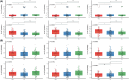
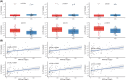
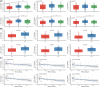
Results: Between January 2007 and July 2021, 181 patients were admitted to ICU for a resuscitated cardiac arrest. Poor neurological outcome was observed in 134 patients (74%). Qualitative EEG patterns suggesting high severity were associated with decreased LF/HF. Severity of EEG changes were proportional to higher absolute values of brain-to-heart coupling strength (p < 0.02 for all brain-to-heart frequencies) and lower values of alpha-to-HF complexity (p = 0.049). Brain-to-heart coupling strength was significantly higher in patients with bilateral absent N20 and correlated with neuron-specific enolase levels at Day 3. This aberrant brain-to-heart coupling (increased strength and decreased complexity) was also associated with 3-month poor neurological outcome.
Interpretation: Our results suggest that autonomic dysfunctions may well represent hypoxic-ischemic brain injury post cardiac arrest pathophysiology. These results open avenues for integrative monitoring of autonomic functioning in critical care patients.
© 2024 The Authors. Annals of Clinical and Translational Neurology published by Wiley Periodicals LLC on behalf of American Neurological Association.
Conflict of interest statement
Nothing to report.
Figures


Similar articles
-
Heart rate variability for neuro-prognostication after CA: Insight from the Parisian registry.Resuscitation. 2024 Sep;202:110294. doi: 10.1016/j.resuscitation.2024.110294. Epub 2024 Jun 24. Resuscitation. 2024. PMID: 38925291
-
Neuron-Specific Enolase Predicts Poor Outcome After Cardiac Arrest and Targeted Temperature Management: A Multicenter Study on 1,053 Patients.Crit Care Med. 2017 Jul;45(7):1145-1151. doi: 10.1097/CCM.0000000000002335. Crit Care Med. 2017. PMID: 28426467
-
Neurological pupil index and its association with other prognostic tools after cardiac arrest: A post hoc analysis.Resuscitation. 2022 Oct;179:259-266. doi: 10.1016/j.resuscitation.2022.07.030. Epub 2022 Jul 30. Resuscitation. 2022. PMID: 35914656
-
Assessing brain injury after cardiac arrest, towards a quantitative approach.Curr Opin Crit Care. 2019 Jun;25(3):211-217. doi: 10.1097/MCC.0000000000000611. Curr Opin Crit Care. 2019. PMID: 31022084 Review.
-
Prognostication after cardiac arrest.Crit Care. 2018 Jun 5;22(1):150. doi: 10.1186/s13054-018-2060-7. Crit Care. 2018. PMID: 29871657 Free PMC article. Review.
Cited by
-
A framework for quantifying the coupling between brain connectivity and heartbeat dynamics: Insights into the disrupted network physiology in Parkinson's disease.Hum Brain Mapp. 2024 Apr;45(5):e26668. doi: 10.1002/hbm.26668. Hum Brain Mapp. 2024. PMID: 38520378 Free PMC article.
-
Explainable machine learning model based on EEG, ECG, and clinical features for predicting neurological outcomes in cardiac arrest patient.Sci Rep. 2025 Apr 3;15(1):11498. doi: 10.1038/s41598-025-93579-0. Sci Rep. 2025. PMID: 40181037 Free PMC article.
-
Predictive Performance of Neuron-Specific Enolase (NSE) for Survival after Resuscitation from Cardiac Arrest: A Systematic Review and Meta-Analysis.J Clin Med. 2023 Dec 13;12(24):7655. doi: 10.3390/jcm12247655. J Clin Med. 2023. PMID: 38137724 Free PMC article. Review.
-
Dynamic brain-heart-gut coupling during sleep: a continuous physiological signal analysis.Front Neurosci. 2025 May 26;19:1594759. doi: 10.3389/fnins.2025.1594759. eCollection 2025. Front Neurosci. 2025. PMID: 40491939 Free PMC article.
-
Dynamic brain-heart interaction in sleep characterized by variational phase-amplitude coupling framework.Commun Biol. 2025 Aug 16;8(1):1235. doi: 10.1038/s42003-025-08685-6. Commun Biol. 2025. PMID: 40818995 Free PMC article.
References
-
- Perkins GD, Callaway CW, Haywood K, et al. Brain injury after cardiac arrest. Lancet. 2021;398(10307):1269‐1278. - PubMed
-
- Lemiale V, Dumas F, Mongardon N, et al. Intensive care unit mortality after cardiac arrest: the relative contribution of shock and brain injury in a large cohort. Intensive Care Med. 2013;39(11):1972‐1980. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous
