Analysis of Predictors and Risk Factors of Postpolypectomy Syndrome
- PMID: 38248004
- PMCID: PMC10814321
- DOI: 10.3390/diagnostics14020127
Analysis of Predictors and Risk Factors of Postpolypectomy Syndrome
Abstract
Background and aims: Postpolypectomy syndrome (PPS) is a relevant adverse event that can appear after polypectomy. Several publications mention postpolypectomy syndrome using different criteria to define it. The aim of this study is to detect potential risk factors and predictors for developing PPS and to define the main criteria of PPS.
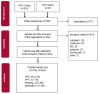
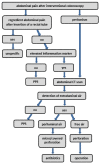
Methods: In this retrospective monocentric study, 475 out of 966 patients who underwent colonoscopy with polypectomy from October 2015 to June 2020 were included. The main criterion of PPS is defined as the development of postinterventional abdominal pain lasting more than six hours.
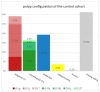
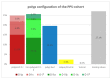
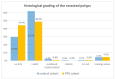
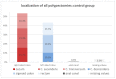
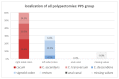
Results: A total of 9.7% of the patients developed PPS, which was defined as local abdominal pain around the polypectomy area after six hours. A total of 8.6% of the study population had abdominal pain within six hours postintervention. A total of 3.7% had an isolated triad of fever, leukocytosis, and increased CRP in the absence of abdominal pain. Increased CRP combined with an elevated temperature over 37.5 °C seems to be a positive predictor for developing PPS. Four independent risk factors could be detected: serrated polyp morphology, polypoid configurated adenomas, polyp localization in the cecum, and the absence of intraepithelial neoplasia.
Conclusions: Four independent risk factors for developing PPS were detected. The combination of increased CRP levels with elevated temperature seems to be a predictor for this pathology. As expected, the increasing use of cold snare polypectomies will reduce the incidence of this syndrome. Key summary: Our monocentric study on 966 patients detected four independent risk factors for developing PPS: pedunculated polyp, resected polyps in the cecum, absence of IEN, and serrated polyp morphology. The combination of increased CRP levels with elevated temperature seems to be a predictor for this pathology.
Keywords: PPS; abdominal pain; adenoma; colonoscopy; polyp; postpolypectomy syndrome.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
Similar articles
-
Postpolypectomy Syndrome Without the Use of Hot Snare.Cureus. 2025 Feb 14;17(2):e79010. doi: 10.7759/cureus.79010. eCollection 2025 Feb. Cureus. 2025. PMID: 40091948 Free PMC article.
-
Snaring large serrated polyps.Surg Endosc. 2013 May;27(5):1622-7. doi: 10.1007/s00464-012-2640-6. Epub 2012 Dec 13. Surg Endosc. 2013. PMID: 23239298
-
Bleeding Risk With Cold Snare Polypectomy of ≤10 mm Pedunculated Colon Polyps.J Clin Gastroenterol. 2023 Mar 1;57(3):294-299. doi: 10.1097/MCG.0000000000001699. J Clin Gastroenterol. 2023. PMID: 35470299
-
Korean Guidelines for Postpolypectomy Colonoscopic Surveillance: 2022 revised edition.Intest Res. 2023 Jan;21(1):20-42. doi: 10.5217/ir.2022.00096. Epub 2023 Jan 31. Intest Res. 2023. PMID: 36751043 Free PMC article. Review.
-
Korean guidelines for postpolypectomy colonoscopic surveillance: 2022 revised edition.Clin Endosc. 2022 Nov;55(6):703-725. doi: 10.5946/ce.2022.136. Epub 2022 Oct 13. Clin Endosc. 2022. PMID: 36225130 Free PMC article. Review.
Cited by
-
Postpolypectomy Syndrome Without the Use of Hot Snare.Cureus. 2025 Feb 14;17(2):e79010. doi: 10.7759/cureus.79010. eCollection 2025 Feb. Cureus. 2025. PMID: 40091948 Free PMC article.
References
-
- Ito S., Hotta K., Imai K., Yamaguchi Y., Kishida Y., Takizawa K., Kakushima N., Tanaka M., Kawata N., Yoshida M., et al. Risk factors of post-endoscopic submucosal dissection electrocoagulation syndrome for colorectal neoplasm. J. Gastroenterol. Hepatol. 2018;33:2001–2006. doi: 10.1111/jgh.14302. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

