Circulating biomarkers of airflow limitation across the life span
- PMID: 38253260
- PMCID: PMC11162345
- DOI: 10.1016/j.jaci.2023.12.026
Circulating biomarkers of airflow limitation across the life span
Abstract
Background: Airflow limitation is a hallmark of chronic obstructive pulmonary disease, which can develop through different lung function trajectories across the life span. There is a need for longitudinal studies aimed at identifying circulating biomarkers of airflow limitation across different stages of life.
Objectives: This study sought to identify a signature of serum proteins associated with airflow limitation and evaluate their relation to lung function longitudinally in adults and children.
Methods: This study used data from 3 adult cohorts (TESAOD [Tucson Epidemiological Study of Airway Obstructive Disease], SAPALDIA [Swiss Cohort Study on Air Pollution and Lung and Heart Diseases in Adults], LSC [Lovelace Smoker Cohort]) and 1 birth cohort (TCRS [Tucson Children's Respiratory Study]) (N = 1940). In TESAOD, among 46 circulating proteins, we identified those associated with FEV1/forced vital capacity (FVC) percent (%) predicted levels and generated a score based on the sum of their z-scores. Cross-sectional analyses were used to test the score for association with concomitant lung function. Longitudinal analyses were used to test the score for association with subsequent lung function growth in childhood and decline in adult life.
Results: After false discovery rate adjustment, serum levels of 5 proteins (HP, carcinoembryonic antigen, ICAM1, CRP, TIMP1) were associated with percent predicted levels of FEV1/FVC and FEV1 in TESAOD. In cross-sectional multivariate analyses the 5-biomarker score was associated with FEV1 % predicted in all adult cohorts (meta-analyzed FEV1 decrease for 1-SD score increase: -2.9%; 95% CI: -3.9%, -1.9%; P = 2.4 × 10-16). In multivariate longitudinal analyses, the biomarker score at 6 years of age was inversely associated with FEV1 and FEV1/FVC levels attained by young adult life (P = .02 and .005, respectively). In adults, persistently high levels of the biomarker score were associated with subsequent accelerated decline of FEV1 and FEV1/FVC (P = .01 and .001).
Conclusions: A signature of 5 circulating biomarkers of airflow limitation was associated with both impaired lung function growth in childhood and accelerated lung function decline in adult life, indicating that these proteins may be involved in multiple lung function trajectories leading to chronic obstructive pulmonary disease.
Keywords: Airflow limitation; biomarkers; lung function.
Copyright © 2024 American Academy of Allergy, Asthma & Immunology. Published by Elsevier Inc. All rights reserved.
Figures


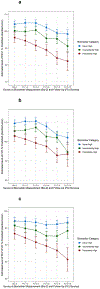

References
-
- Lange P, Celli B, Agusti A, Boje Jensen G, Divo M, Faner R, et al. Lung-Function Trajectories Leading to Chronic Obstructive Pulmonary Disease. N Engl J Med 2015; 373:111–22. - PubMed
-
- US Department of Health and Human Services. How Tobacco Smoke Causes Disease: The Biology and Behavioral Basis for Smoking-Attributable Disease. A Report of the Surgeon General. Atlanta, GA: US Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health. 2010.
-
- Exposure and biomarker assessment in humans. In: Stratton K, Shetty P, Wallace R, Bondurant S, editors. Clearing the Smoke: Assessing the Science Base for Tobacco Harm Reduction. Washington (DC): National Academy Press; 2001. p. 309–66. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

