Diffuse-Type Tenosynovial Giant Cell Tumor: What Are the Important Findings on the Initial and Follow-Up MRI?
- PMID: 38254890
- PMCID: PMC10814250
- DOI: 10.3390/cancers16020402
Diffuse-Type Tenosynovial Giant Cell Tumor: What Are the Important Findings on the Initial and Follow-Up MRI?
Abstract
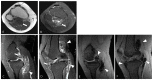
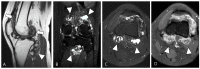
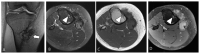
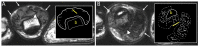
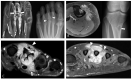
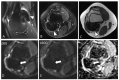
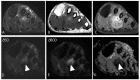
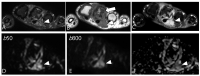
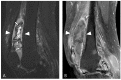
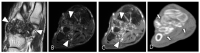
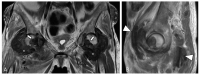
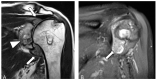
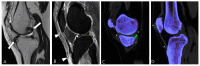
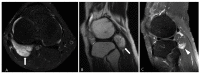
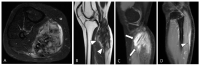
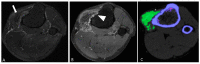
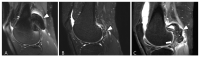
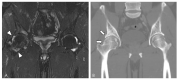
Tenosynovial giant cell tumor (TSGCT) is a rare soft tissue tumor that involves the synovial lining of joints, bursae, and tendon sheaths, primarily affecting young patients (usually in the fourth decade of life). The tumor comprises two subtypes: the localized type (L-TSGCT) and the diffuse type (D-TSGCT). Although these subtypes share histological and genetic similarities, they present a different prognosis. D-TSGCT tends to exhibit local aggressiveness and a higher recurrence rate compared to L-TSGCT. Magnetic resonance imaging (MRI) is the preferred diagnostic tool for both the initial diagnosis and for treatment planning. When interpreting the initial MRI of a suspected TSGCT, it is essential to consider: (i) the characteristic findings of TSGCT-evident as low to intermediate signal intensity on both T1- and T2-weighted images, with a blooming artifact on gradient-echo sequences due to hemosiderin deposition; (ii) the possibility of D-TSGCT-extensive involvement of the synovial membrane with infiltrative margin; and (iii) the resectability and extent-if resectable, synovectomy is performed; if not, a novel systemic therapy involving colony-stimulating factor 1 receptor inhibitors is administered. In the interpretation of follow-up MRIs of D-TSGCTs after treatment, it is crucial to consider both tumor recurrence and potential complications such as osteoarthritis after surgery as well as the treatment response after systemic treatment. Given its prevalence in young adult patents and significant impact on patients' quality of life, clinical trials exploring new agents targeting D-TSGCT are currently underway. Consequently, understanding the characteristic MRI findings of D-TSGCT before and after treatment is imperative.
Keywords: diffuse type; local recurrence; magnetic resonance imaging; osteoarthritis; targeted therapy; tenosynovial giant cell tumor; treatment response.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

References
-
- Spierenburg G., Suevos Ballesteros C., Stoel B.C., Navas Canete A., Gelderblom H., van de Sande M.A.J., van Langevelde K. MRI of diffuse-type tenosynovial giant cell tumour in the knee: A guide for diagnosis and treatment response assessment. Insights Imaging. 2023;14:22. doi: 10.1186/s13244-023-01367-z. - DOI - PMC - PubMed
-
- Sciot R., Rosai J., Dal Cin P., de Wever I., Fletcher C.D., Mandahl N., Mertens F., Mitelman F., Rydholm A., Tallini G., et al. Analysis of 35 cases of localized and diffuse tenosynovial giant cell tumor: A report from the Chromosomes and Morphology (CHAMP) study group. Mod. Pathol. 1999;12:576–579. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

