Intestinal Oxalate Absorption, Enteric Hyperoxaluria, and Risk of Urinary Stone Formation in Patients with Crohn's Disease
- PMID: 38257157
- PMCID: PMC10821467
- DOI: 10.3390/nu16020264
Intestinal Oxalate Absorption, Enteric Hyperoxaluria, and Risk of Urinary Stone Formation in Patients with Crohn's Disease
Abstract
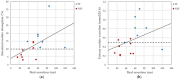
Nephrolithiasis is a common urologic manifestation of Crohn's disease. The purpose of this study was to investigate the clinical characteristics, intestinal oxalate absorption, and risk factors for urinary stone formation in these patients. In total, 27 patients with Crohn's disease and 27 healthy subjects were included in the present study. Anthropometric, clinical, and 24 h urinary parameters were determined, and the [13C2]oxalate absorption test was performed. Among all patients, 18 had undergone ileal resection, 9 of whom had a history of urinary stones. Compared to healthy controls, the urinary excretion values of calcium, magnesium, potassium, sulfate, creatinine, and citrate were significantly lower in patients with Crohn's disease. Intestinal oxalate absorption, the fractional and 24 h urinary oxalate excretion, and the risk of calcium oxalate stone formation were significantly higher in patients with urolithiasis than in patients without urolithiasis or in healthy controls. Regardless of the group, between 83% and 96% of the [13C2]oxalate was detected in the urine within the first 12 h after ingestion. The length of ileum resection correlated significantly with the intestinal absorption and urinary excretion of oxalate. These findings suggest that enteric hyperoxaluria can be attributed to the hyperabsorption of oxalate following extensive ileal resection. Oral supplementation of calcium and magnesium, as well as alkali citrate therapy, should be considered as treatment options for urolithiasis.
Keywords: Crohn’s disease; bowel resection; calcium; diet; fat malabsorption; intestinal oxalate absorption; kidney stones; oxalate; secondary hyperoxaluria; urolithiasis.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

