Patient burden and joint inflammation during development of RA from arthralgia: is it similar in ACPA-positive and ACPA-negative disease?
- PMID: 38261628
- PMCID: PMC11371371
- DOI: 10.1093/rheumatology/keae044
Patient burden and joint inflammation during development of RA from arthralgia: is it similar in ACPA-positive and ACPA-negative disease?
Abstract
Objectives: ACPA-positive and ACPA-negative RA differ in underlying risk factors but have a similar clinical presentation at RA diagnosis. It is unknown what the ACPA-associated differences or similarities are during the symptomatic at-risk stage of RA, i.e. clinically suspect arthralgia (CSA). To deepen insights into these differences/similarities, we compared the course of symptoms/impairments and subclinical joint inflammation in the CSA phase during progression to inflammatory arthritis (IA) or to CSA resolution.
Methods: A total of 845 CSA patients were followed for a median of 24 months; 136 patients developed IA and an additional 355/505 patients had resolution of CSA according to rheumatologists. Patient burden (pain, morning stiffness, fatigue, functional disabilities, presenteeism) was assessed at baseline and 4, 12 and 24 months and at IA development. Subclinical joint inflammation in the hands and feet was assessed over time with 1.5T MRI. Linear and Poisson mixed models were used.
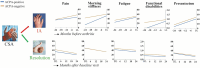
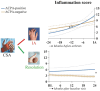
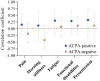
Results: In both ACPA-positive and ACPA-negative patients, patient burden increased towards IA development and decreased towards CSA resolution. However, patient burden was lower in ACPA-positive vs ACPA-negative disease at all timepoints. Conversely, subclinical joint inflammation tended to increase more rapidly during development of ACPA-positive IA [incidence rate ratio (IRR) 1.52 (95% CI 0.94, 2.47), P = 0.089] and remained higher over time in ACPA-positive CSA patients achieving resolution compared with ACPA-negative patients [IRR 1.52 (95% CI 1.07, 2.15), P = 0.018]. Although correlation coefficients between changes in patient burden and subclinical joint inflammation during progression to IA were weak, they were consistently higher in ACPA-positive than ACPA-negative disease, e.g. ρ = 0.29 vs 0.12 for functional disabilities.
Conclusion: During RA development and CSA resolution, ACPA-positive CSA patients have lower patient burden but more subclinical joint inflammation than ACPA-negative CSA patients. These data strengthen the notion that the development of ACPA-positive and ACPA-negative RA is pathophysiologically different and encourage further research on these differences.
Keywords: anti-citrullinated protein antibody; clinically suspect arthralgia; joint inflammation; patient burden; rheumatoid arthritis.
© The Author(s) 2024. Published by Oxford University Press on behalf of the British Society for Rheumatology.
Figures
Similar articles
-
Sequence of joint tissue inflammation during rheumatoid arthritis development.Arthritis Res Ther. 2018 Nov 21;20(1):260. doi: 10.1186/s13075-018-1756-z. Arthritis Res Ther. 2018. PMID: 30463603 Free PMC article.
-
Joint involvement in RA starts predominantly in the hands: functional, clinical and imaging studies in clinically suspect arthralgia and during progression to RA.RMD Open. 2023 Jun;9(2):e003107. doi: 10.1136/rmdopen-2023-003107. RMD Open. 2023. PMID: 37328293 Free PMC article.
-
Shorter reproductive time span and early menopause increase the risk of ACPA-negative inflammatory arthritis in postmenopausal women with clinically suspect arthralgia.Rheumatology (Oxford). 2025 Jun 1;64(6):3451-3457. doi: 10.1093/rheumatology/keaf083. Rheumatology (Oxford). 2025. PMID: 39951288 Free PMC article.
-
Determining in which pre-arthritis stage HLA-shared epitope alleles and smoking exert their effect on the development of rheumatoid arthritis.Ann Rheum Dis. 2022 Jan;81(1):48-55. doi: 10.1136/annrheumdis-2021-220546. Epub 2021 Jul 20. Ann Rheum Dis. 2022. PMID: 34285049 Free PMC article. Review.
-
The pre-clinical phase of rheumatoid arthritis: From risk factors to prevention of arthritis.Autoimmun Rev. 2021 May;20(5):102797. doi: 10.1016/j.autrev.2021.102797. Epub 2021 Mar 18. Autoimmun Rev. 2021. PMID: 33746022 Review.
Cited by
-
Are seronegative patients with rheumatoid arthritis and clinically suspect arthralgia properly represented in randomized clinical trials?Clin Rheumatol. 2025 Jan;44(1):515-519. doi: 10.1007/s10067-024-07187-w. Epub 2024 Oct 26. Clin Rheumatol. 2025. PMID: 39455473 Free PMC article. Review.
-
The natural course of health-related quality of life in patients with clinically suspect arthralgia: a longitudinal study in progressors and non-progressors to rheumatoid arthritis.Rheumatol Int. 2025 Apr 19;45(5):112. doi: 10.1007/s00296-025-05865-9. Rheumatol Int. 2025. PMID: 40252120 Free PMC article.
-
Do MRI-detected erosions in the RA-risk phase of arthralgia reflect current or imminent radiographic erosions? A large longitudinal imaging study.Rheumatology (Oxford). 2025 Jul 1;64(7):4200-4206. doi: 10.1093/rheumatology/keaf149. Rheumatology (Oxford). 2025. PMID: 40097268 Free PMC article.
-
Windows for intervention in the prearthritis phase of rheumatoid arthritis? A narrative review of key triggering events and potential preventive strategies.RMD Open. 2025 Jul 10;11(3):e005778. doi: 10.1136/rmdopen-2025-005778. RMD Open. 2025. PMID: 40639878 Free PMC article. Review.
References
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

