Sustainability in Internal Medicine: A Year-Long Ward-Wide Observational Study
- PMID: 38276237
- PMCID: PMC10820757
- DOI: 10.3390/jpm14010115
Sustainability in Internal Medicine: A Year-Long Ward-Wide Observational Study
Abstract
Population aging and multimorbidity challenge health system sustainability, but the role of assistance-related variables rather than individual pathophysiological factors in determining patient outcomes is unclear. To identify assistance-related determinants of sustainable hospital healthcare, all patients hospitalised in an Internal Medicine Unit (n = 1073) were enrolled in a prospective year-long observational study and split 2:1 into a training (n = 726) and a validation subset (n = 347). Demographics, comorbidities, provenance setting, estimates of complexity (cumulative illness rating scale, CIRS: total, comorbidity, CIRS-CI, and severity, CIRS-SI subscores) and intensity of care (nine equivalents of manpower score, NEMS) were analysed at individual and Unit levels along with variations in healthcare personnel as determinants of in-hospital mortality, length of stay and nosocomial infections. Advanced age, higher CIRS-SI, end-stage cancer, and the absence of immune-mediated diseases were correlated with higher mortality. Admission from nursing homes or intensive care units, dependency on activity of daily living, community- or hospital-acquired infections, oxygen support and the number of exits from the Unit along with patient/physician ratios were associated with prolonged hospitalisations. Upper gastrointestinal tract disorders, advanced age and higher CIRS-SI were associated with nosocomial infections. In addition to demographic variables and multimorbidity, physician number and assistance context affect hospitalisation outcomes and healthcare sustainability.
Keywords: general internal medicine; healthcare resources; hospital-acquired infections; in-hospital mortality; length of stay; sustainability.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

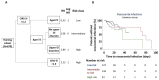
Similar articles
-
Multimorbidity in elderly hospitalised patients and risk of Clostridium difficile infection: a retrospective study with the Cumulative Illness Rating Scale (CIRS).BMJ Open. 2015 Oct 26;5(10):e009316. doi: 10.1136/bmjopen-2015-009316. BMJ Open. 2015. PMID: 26503394 Free PMC article.
-
Comorbidity does not mean clinical complexity: evidence from the RePoSI register.Intern Emerg Med. 2020 Jun;15(4):621-628. doi: 10.1007/s11739-019-02211-3. Epub 2019 Oct 24. Intern Emerg Med. 2020. PMID: 31650434
-
Hyperglycemia at admission, comorbidities, and in-hospital mortality in elderly patients hospitalized in internal medicine wards: data from the RePoSI Registry.Acta Diabetol. 2021 Sep;58(9):1225-1236. doi: 10.1007/s00592-021-01716-8. Epub 2021 Apr 22. Acta Diabetol. 2021. PMID: 33890176 Free PMC article.
-
Hypovitaminosis D: A Disease Marker in Hospitalized Very Old Persons at Risk of Malnutrition.Nutrients. 2019 Jan 9;11(1):128. doi: 10.3390/nu11010128. Nutrients. 2019. PMID: 30634546 Free PMC article.
-
[Evaluation of Infections in Intensive Care Units: A Multicentre Point-Prevalence Study].Mikrobiyol Bul. 2019 Oct;53(4):364-373. doi: 10.5578/mb.68665. Mikrobiyol Bul. 2019. PMID: 31709934 Review. Turkish.
Cited by
-
Sustainable development goals: a call for future internal medicine.Intern Emerg Med. 2025 Aug;20(5):1329-1338. doi: 10.1007/s11739-025-03941-3. Epub 2025 Apr 11. Intern Emerg Med. 2025. PMID: 40214923 Free PMC article. Review.
References
-
- Haklai Z., Glick S., Benbassat J. Determinants of hospital utilization: The content of medical inpatient care in Israel. Isr. Med. Assoc. J. 2000;2:339–342. - PubMed
-
- Henderson L., Maniam B., Leavell H. The silver tsunami: Evaluating the impact of population aging in the US. J. Bus. Behav. Sci. 2017;29:153–169.
Grants and funding
LinkOut - more resources
Full Text Sources

