Evaluation of surgical treatment strategies and outcome for cerebral arachnoid cysts in children and adults
- PMID: 38280116
- PMCID: PMC10821836
- DOI: 10.1007/s00701-024-05950-1
Evaluation of surgical treatment strategies and outcome for cerebral arachnoid cysts in children and adults
Abstract
Objective: The best treatment strategies for cerebral arachnoid cysts (CAC) are still up for debate. In this study, we present CAC management, outcome data, and risk factors for recurrence after surgical treatment, focusing on microscopic/endoscopic approaches as compared to minimally invasive stereotactic procedures in children and adults.
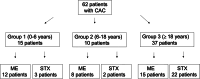
Methods: In our single-institution retrospective database, we identified all patients treated surgically for newly diagnosed CAC between 2000 and 2022. Microscopic/endoscopic surgery (ME) aimed for safe cyst wall fenestration. Stereotactic implantation of an internal shunt catheter (STX) to drain CAC into the ventricles and/or cisterns was used as an alternative procedure in patients aged ≥ 3 years. Treatment decisions in favor of ME vs. STX were made by interdisciplinary consensus. The primary study endpoint was time to CAC recurrence (TTR). Secondary endpoints were outcome metrics including clinical symptoms and MR-morphological analyses. Data analysis included subdivision of the total cohort into three distinct age groups (AG1, < 6 years; AG2, 6-18 years; AG3, ≥ 18 years).
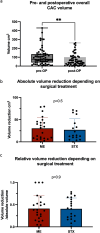
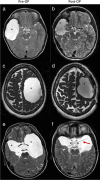
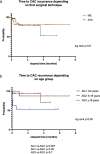
Results: Sixty-two patients (median age 26.5 years, range 0-82 years) were analyzed. AG1 included 15, AG2 10, and AG3 37 patients, respectively. The main presenting symptoms were headache and vertigo. In AG1 hygromas, an increase in head circumference and thinning of cranial calvaria were most frequent. Thirty-five patients underwent ME and 27 STX, respectively; frequency did not differ between AGs. There were two (22.2%) periprocedural venous complications in infants (4- and 10-month-old) during an attempt at prepontine fenestration of a complex CAC, one with fatal outcome in a 10-month-old boy. Other complications included postoperative bleeding (2, 22.2%), CSF leaks (4, 44.4%), and meningitis (1, 11.1%). Overall, clinical improvement and significant volume reduction (p = 0.008) were seen in all other patients; this did not differ between AGs. Median follow-up for all patients was 25.4 months (range, 3.1-87.1 months). Recurrent cysts were seen in 16.1%, independent of surgical procedure used (p = 0.7). In cases of recurrence, TTR was 7.9 ± 12.7 months. Preoperative ventricular expansion (p = 0.03), paresis (p = 0.008), and age under 6 years (p = 0.03) were significant risk factors for CAC recurrence in multivariate analysis.
Conclusions: In patients suffering from CAC, both ME and STX can improve clinical symptoms at low procedural risk, with equal extent of CAC volume reduction. However, in infants and young children, CAC are more often associated with severe clinical symptoms, stereotactic procedures have limited use, and microsurgery in the posterior fossa may bear the risk of severe venous bleeding.
Keywords: Arachnoid cysts; Hydrocephalus; Microsurgery; Stereotaxy.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
References
-
- Ali M, Bennardo M, Almenawer SA, Zagzoog N, Smith AA, Dao D, Ajani O, Farrokhyar F, Singh SK (2015) Exploring predictors of surgery and comparing operative treatment approaches for pediatric intracranial arachnoid cysts: a case series of 83 patients. J Neurosurg Pediatr 16:275–282. 10.3171/2015.2.Peds14612 - PubMed
-
- Ali ZS, Lang SS, Bakar D, Storm PB, Stein SC (2014) Pediatric intracranial arachnoid cysts: comparative effectiveness of surgical treatment options. Childs Nerv Syst 30:461–469. 10.1007/s00381-013-2306-2 - PubMed
-
- Arai H, Sato K, Wachi A, Okuda O, Takeda N (1996) Arachnoid cysts of the middle cranial fossa: experience with 77 patients who were treated with cystoperitoneal shunting Neurosurgery 39:1108–1112. discussion 1112–1103 10.1097/00006123-199612000-00007 - PubMed
-
- Artico M, Cervoni L, Salvati M, Fiorenza F, Caruso R (1995) Supratentorial arachnoid cysts: clinical and therapeutic remarks on 46 cases. Acta Neurochir (Wien) 132:75–78. 10.1007/bf01404851 - PubMed
-
- Boutarbouch M, El Ouahabi A, Rifi L, Arkha Y, Derraz S, El Khamlichi A (2008) Management of intracranial arachnoid cysts: institutional experience with initial 32 cases and review of the literature. Clin Neurol Neurosurg 110:1–7. 10.1016/j.clineuro.2007.08.009 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

