Mechanistic Modeling of Intrathecal Chemotherapy Pharmacokinetics in the Human Central Nervous System
- PMID: 38289997
- PMCID: PMC10984761
- DOI: 10.1158/1078-0432.CCR-23-3062
Mechanistic Modeling of Intrathecal Chemotherapy Pharmacokinetics in the Human Central Nervous System
Abstract
Purpose: The pharmacokinetics of intrathecally administered antibody or small-molecule drugs in the human central nervous system (CNS) remains poorly understood. This study aimed to provide mechanistic and quantitative perspectives on the CNS pharmacokinetics of intrathecal chemotherapy, by using a physiologically based pharmacokinetic (PBPK) modeling approach.
Experimental design: A novel CNS PBPK model platform was developed and verified, which accounted for the human CNS general anatomy and physiologic processes governing drug distribution and disposition. The model was used to predict CNS pharmacokinetics of antibody (trastuzumab) and small-molecule drugs (methotrexate, abemaciclib, tucatinib) following intraventricular injection or intraventricular 24-hour infusion, and to assess the key determinants of drug penetration into the deep brain parenchyma.
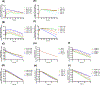
Results: Intraventricularly administered antibody and small-molecule drugs exhibited distinct temporal and spatial distribution and disposition in human CNS. Both antibody and small-molecule drugs achieved supratherapeutic or therapeutic concentrations in the cerebrospinal fluid (CSF) compartments and adjacent brain tissue. While intrathecal small-molecule drugs penetrated the deep brain parenchyma to a negligible extent, intrathecal antibodies may achieve therapeutic concentrations in the deep brain parenchyma. Intraventricular 24-hour infusion enabled prolonged CNS exposure to therapeutically relevant concentrations while avoiding excessively high and potentially neurotoxic drug concentrations.
Conclusions: CNS PBPK modeling, in line with available clinical efficacy data, confirms the therapeutic value of intrathecal chemotherapy with antibody or small-molecule drugs for treating neoplastic meningitis and warrants further clinical investigation of intrathecal antibody drugs to treat brain parenchyma tumors. Compared with intraventricular injection, intraventricular 24-hour infusion may mitigate neurotoxicity while retaining potential efficacy.
©2024 American Association for Cancer Research.
Conflict of interest statement
Figures



Similar articles
-
SpatialCNS-PBPK: An R/Shiny Web-Based Application for Physiologically Based Pharmacokinetic Modeling of Spatial Pharmacokinetics in the Human Central Nervous System and Brain Tumors.CPT Pharmacometrics Syst Pharmacol. 2025 May;14(5):864-880. doi: 10.1002/psp4.70026. Epub 2025 Apr 4. CPT Pharmacometrics Syst Pharmacol. 2025. PMID: 40183989 Free PMC article.
-
Cerebrospinal Fluid Flow Enhancement (CFE) Increases the Spatial Distribution of Methotrexate after Intracerebroventricular Administration in a Sheep Model.Mol Pharm. 2025 Jul 7;22(7):3654-3665. doi: 10.1021/acs.molpharmaceut.4c01030. Epub 2025 Jun 10. Mol Pharm. 2025. PMID: 40494817
-
The Black Book of Psychotropic Dosing and Monitoring.Psychopharmacol Bull. 2024 Jul 8;54(3):8-59. Psychopharmacol Bull. 2024. PMID: 38993656 Free PMC article. Review.
-
Uncommon Non-MS Demyelinating Disorders of the Central Nervous System.Curr Neurol Neurosci Rep. 2025 Jul 1;25(1):45. doi: 10.1007/s11910-025-01432-8. Curr Neurol Neurosci Rep. 2025. PMID: 40591029 Review.
-
A rapid and systematic review of the clinical effectiveness and cost-effectiveness of paclitaxel, docetaxel, gemcitabine and vinorelbine in non-small-cell lung cancer.Health Technol Assess. 2001;5(32):1-195. doi: 10.3310/hta5320. Health Technol Assess. 2001. PMID: 12065068
Cited by
-
Mechanistic Modeling of Spatial Heterogeneity of Drug Penetration and Exposure in the Human Central Nervous System and Brain Tumors.Clin Pharmacol Ther. 2025 Mar;117(3):690-703. doi: 10.1002/cpt.3505. Epub 2024 Nov 22. Clin Pharmacol Ther. 2025. PMID: 39575553
-
Young rat vascular endothelial cells promote neurological recovery of stroke aged rat via HIF-1α.iScience. 2025 Apr 29;28(6):112552. doi: 10.1016/j.isci.2025.112552. eCollection 2025 Jun 20. iScience. 2025. PMID: 40487449 Free PMC article.
-
SpatialCNS-PBPK: An R/Shiny Web-Based Application for Physiologically Based Pharmacokinetic Modeling of Spatial Pharmacokinetics in the Human Central Nervous System and Brain Tumors.CPT Pharmacometrics Syst Pharmacol. 2025 May;14(5):864-880. doi: 10.1002/psp4.70026. Epub 2025 Apr 4. CPT Pharmacometrics Syst Pharmacol. 2025. PMID: 40183989 Free PMC article.
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

