Awareness and practice of airway pressure release ventilation mode in acute respiratory distress syndrome patients among nurses in Saudi Arabia
- PMID: 38291421
- PMCID: PMC10826023
- DOI: 10.1186/s12912-024-01763-w
Awareness and practice of airway pressure release ventilation mode in acute respiratory distress syndrome patients among nurses in Saudi Arabia
Abstract
Background: This study aimed to assess the knowledge and current practice of using the airway pressure release ventilation (APRV) mode with acute respiratory distress syndrome (ARDS) patients and identify barriers to not using this mode of ventilation among nurses who work in critical areas in Saudi Arabia.
Methods: Between December 2022 and April 2023, a cross-sectional online survey was disseminated to nurses working in critical care areas in Saudi Arabia. The characteristics of the respondents were analyzed using descriptive statistics. Percentages and frequencies were used to report categorical variables.
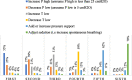
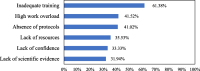
Results: Overall, 1,002 nurses responded to the online survey, of whom 592 (59.1%) were female. Only 248 (24.7%) nurses had ever used APRV mode, whereas only 229 (22.8%) received training on APRV mode. Moreover, 602 (60.0%) nurses did not know whether APRV was utilized in their hospital. Additionally, 658 (65.6%) nurses did not know whether APRV mode was managed using a standard protocol. Prone positioning was the highest recommended intervention by 444 (43.8%) when a conventional MV failed to improve oxygenation in patients with ARDS. 323 (32.2%) respondents stated that the P-high should be set equal to the plateau pressure on a conventional ventilator, while 400 (39.9%) said that the P-low should match PEEP from a conventional ventilator. Almost half of the respondents (446, 44.5%) stated that the T-high should be set between 4 and 6 s, while 415 (41.4%) said that the T-low should be set at 0.4 to 0.8 s. Over half of the nurses (540, 53.9%) thought that the maximum allowed tidal volume during the release phase should be 4-6 ml/kg. Moreover, 475 (47.4%) believed that the maximum allowed P-high setting should be 35 cm H2O. One-third of the responders (329, 32.8%) stated that when weaning patients with ARDS while in APRV mode, the P-high should be reduced gradually to reach a target of 10 cm H2O. However, 444 (44.3%) thought that the T-high should be gradually increased to reach a target of 10 s. Half of the responders (556, 55.5%) felt that the criteria to switch the patient to continuous positive airway pressure (CPAP) were for the patient to have an FiO2 ≤ 0.4, P-high ≤ 10 cm H2O, and T-high ≥ 10 s. Lack of training was the most common barrier to not using APRV by 615 (61.4%).
Conclusion: The majority of nurses who work in critical care units have not received sufficient training in APRV mode. A significant discrepancy was observed regarding the clinical application and management of APRV parameters. Inadequate training was the most frequently reported barrier to the use of APRV in patients with ARDS.
Keywords: APRV; ARDS; Mechanical ventilation; Nursing; Saudi Arabia.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures

Similar articles
-
Current practice of using the airway pressure release ventilation mode in acute respiratory distress syndrome patients among respiratory therapists in Saudi Arabia.SAGE Open Med. 2025 Jan 16;13:20503121241312941. doi: 10.1177/20503121241312941. eCollection 2025. SAGE Open Med. 2025. PMID: 39839159 Free PMC article.
-
Knowledge and practice of using airway pressure release ventilation mode in ARDS patients: A survey of physicians.Heliyon. 2023 Nov 22;9(12):e22725. doi: 10.1016/j.heliyon.2023.e22725. eCollection 2023 Dec. Heliyon. 2023. PMID: 38125512 Free PMC article.
-
Early application of airway pressure release ventilation may reduce the duration of mechanical ventilation in acute respiratory distress syndrome.Intensive Care Med. 2017 Nov;43(11):1648-1659. doi: 10.1007/s00134-017-4912-z. Epub 2017 Sep 22. Intensive Care Med. 2017. PMID: 28936695 Free PMC article.
-
Does airway pressure release ventilation offer new hope for treating acute respiratory distress syndrome?J Intensive Med. 2022 Mar 28;2(4):241-248. doi: 10.1016/j.jointm.2022.02.003. eCollection 2022 Oct. J Intensive Med. 2022. PMID: 36785647 Free PMC article. Review.
-
Should Airway Pressure Release Ventilation Be the Primary Mode in ARDS?Respir Care. 2016 Jun;61(6):761-73. doi: 10.4187/respcare.04653. Respir Care. 2016. PMID: 27235312 Review.
Cited by
-
Current practice of using the airway pressure release ventilation mode in acute respiratory distress syndrome patients among respiratory therapists in Saudi Arabia.SAGE Open Med. 2025 Jan 16;13:20503121241312941. doi: 10.1177/20503121241312941. eCollection 2025. SAGE Open Med. 2025. PMID: 39839159 Free PMC article.
References
-
- Roth A. Mechanical Ventilation: Airway Pressure Release Ventilation (Respiratory Therapy). Elsevier Clinical Skills; 2020: p. 1-6. chrome-extension://efaidnbmnnnibpcajpcglclefindmkaj/http://repository.ph....
LinkOut - more resources
Full Text Sources
Miscellaneous

