The value of coordinated analysis of multimodal atherosclerotic plaque imaging in the assessment of cardiovascular and cerebrovascular events
- PMID: 38333417
- PMCID: PMC10850297
- DOI: 10.3389/fcvm.2024.1320222
The value of coordinated analysis of multimodal atherosclerotic plaque imaging in the assessment of cardiovascular and cerebrovascular events
Abstract
Background: Although atherosclerosis (AS) can affect multiple vascular beds, previous studies have focused on the analysis of single-site AS plaques.
Objective: The aim of this study is to explore the differences or similarities in the characteristics of atherosclerotic plaque found in the internal carotid artery, cerebral artery, and coronary artery between patients with atherosclerotic cardiovascular disease (ASCVD) and those without events.
Methods: Patients aged ≥ 18 years who underwent both high-resolution vessel wall imaging (HR-VWI) and coronary computed tomography angiography (CCTA) were retrospectively collected and categorized into the ASCVD group and the non-event group. The plaques were then categorized into culprit plaques, non-culprit plaques, and non-event plaques. Plaque morphological data such as stenosis, stenosis grades, plaque length (PL), plaque volume (PV), minimal lumen area (MLA), enhancement grade, and plaque composition data such as calcified plaque volume (CPV), fibrotic plaque volume (FPV), fibro-lipid plaque volume (FLPV), lipid plaque volume (LPV), calcified plaque volume ratio (CPR), fibrotic plaque volume ratio (FPR), fibro-lipid plaque ratio (FLPR), lipid plaque volume ratio (LPR), intraplaque hemorrhage volume (IPHV), and intraplaque hemorrhage volume ratio (IPHR)were recorded and analyzed.
Results: A total of 44 patients (mean age 66 years, SD 9 years, 28 men) were included. In cervicocephalic plaques, the ASCVD group had more severe stenosis grades (p = 0.030) and demonstrated significant differences in LPV, LPR, and CPV (p = 0.044, 0.030, 0.020) compared with the non-event group. In coronary plaques, the ASCVD group had plaques with greater stenosis (p < 0.001), more severe stenosis grades (p < 0.001), larger volumes (p = 0.001), longer length (p = 0.008), larger FLPV (p = 0.012), larger FPV (p = 0.002), and higher FPR (p = 0.043) compared with the non-event group. There were significant differences observed in stenosis (HR-VWI, CCTA: p < 0.001, p < 0.001), stenosis grades (HR-VWI, CCTA: p < 0.001, p < 0.001), plaque length (HR-VWI, CCTA: p = 0.028, p < 0.001), and plaque volume (HR-VWI, CCTA: p = 0.013, p = 0.018) between the non-event plaque, non-culprit plaque, and culprit plaque. In the image analysis of HR-VWI, there were differences observed between IPHR (p < 0.001), LPR (p = 0.001), FPV (p = 0.011), and CPV (p = 0.015) among the three groups of plaques. FLPV and FPV were significantly different among the three different plaque types from the coronary artery (p = 0.043, p = 0.022).
Conclusion: There is a consistent pattern of change in plaque characteristics between the cervicocephalic and coronary arteries in the same patient.
Keywords: atherosclerotic cardiovascular disease (ASCVD); coronary computed tomography angiography (CCTA); high-resolution vessel wall imaging (HR-VWI); stroke, coronary heart disease (CHD).
© 2024 Yu, Zheng, Dai, Chen, Yang, Ma, Huang and Zhu.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
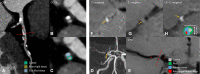
Figures

Similar articles
-
[Value of fractional flow reserve derived from coronary computed tomographic angiography and plaque quantitative analysis in predicting adverse outcomes of non-obstructive coronary heart disease].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2023 Jun;35(6):615-619. doi: 10.3760/cma.j.cn121430-20230215-00092. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2023. PMID: 37366128 Chinese.
-
Detection and Quantification of Symptomatic Atherosclerotic Plaques With High-Resolution Imaging in Cryptogenic Stroke.Stroke. 2020 Dec;51(12):3623-3631. doi: 10.1161/STROKEAHA.120.031167. Epub 2020 Oct 1. Stroke. 2020. PMID: 32998652
-
High resolution 7T MR imaging in characterizing culprit intracranial atherosclerotic plaques.Interv Neuroradiol. 2025 Feb;31(1):24-31. doi: 10.1177/15910199221145760. Epub 2022 Dec 26. Interv Neuroradiol. 2025. PMID: 36573263 Free PMC article.
-
Systematic Review on Magnetic Resonance Angiography with Vessel Wall Imaging for the Characterization of Symptomatic Carotid Artery Plaque.Ann Vasc Surg. 2023 Sep;95:224-232. doi: 10.1016/j.avsg.2023.04.026. Epub 2023 May 8. Ann Vasc Surg. 2023. PMID: 37164170
-
Advances in Artificial Intelligence-Assisted Coronary Computed Tomographic Angiography for Atherosclerotic Plaque Characterization.Rev Cardiovasc Med. 2024 Jan 15;25(1):27. doi: 10.31083/j.rcm2501027. eCollection 2024 Jan. Rev Cardiovasc Med. 2024. PMID: 39077649 Free PMC article. Review.
References
-
- Mach F, Baigent C, Catapano AL, Koskinas KC, Casula M, Badimon L, et al. 2019 ESC/EAS guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk: the task force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and European Atherosclerosis Society (EAS). Eur Heart J. (2020) 41:111–88. 10.1093/eurheartj/ehz455 - DOI - PubMed
-
- Arnett DK, Blumenthal RS, Albert MA, Buroker AB, Goldberger ZD, Hahn EJ, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the American College of Cardiology/American Heart Association task force on clinical practice guidelines. Circulation. (2019) 140:e596–646. 10.1161/CIR.0000000000000678 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

