A Patient Survey Exploring the Burden of Inflammatory Back Pain in Patients With Known Psoriasis
- PMID: 38333437
- PMCID: PMC10853012
- DOI: 10.7759/cureus.51968
A Patient Survey Exploring the Burden of Inflammatory Back Pain in Patients With Known Psoriasis
Abstract
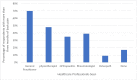
Background In the United Kingdom, diagnostic delay remains a challenge in axial spondyloarthritis (axSpA). Psoriasis is a frequently identified extra-musculoskeletal manifestation associated with axSpA. In this study, we aimed to determine the prevalence of inflammatory back pain (IBP) in psoriasis patients at a specialized psoriasis dermatology clinic in a London NHS Trust. Our primary goal was to identify psoriasis patients with IBP who were not referred to a rheumatologist, potentially leading to axSpA diagnostic delays. Additionally, we aimed to investigate factors contributing to these delays and strategies to address them. Methodology A patient survey consisting of 22 questions was used to assess the prevalence of IBP among 66 psoriasis patients attending a weekly specialized psoriasis dermatology clinic within a London NHS Trust between May and July 2023. The survey comprised patient demographic information along with inquiries about the existence of back pain exceeding three months. The Berlin Criteria was utilized to identify IBP among patients who reported experiencing back pain for over three months. Additionally, the survey sought information on prior diagnosis of axSpA and whether participants had consulted healthcare professionals regarding their back pain. Results Of the 66 patients invited, 51 (77%) completed the survey. The average age of the patients was 50 years (range = 19-74 years), with 58.8% being female. The mean duration of psoriasis was 15.7 years (range = 2-44 years). Overall, 45% (23/51) reported back pain lasting over three months. Among the patients who reported back pain for more than three months, 13 met the Berlin Criteria for IBP (25% of the total surveyed), and only four of these patients had a diagnosis of axSpA. Notably, seven patients (14% of the total surveyed) potentially had undiagnosed axSpA. General practitioners (GPs) were commonly consulted for back pain, yet only 39% of those with prolonged back pain had seen a rheumatologist. Despite experiencing prolonged back pain, 17% of patients had not sought healthcare advice for their symptoms. Conclusions This study highlights that IBP is a common yet underdiagnosed comorbidity in psoriasis patients. Dermatologists, GPs, and other allied healthcare professionals play a crucial role in detecting early axSpA. However, limited awareness of IBP hinders its identification in psoriasis patients and subsequent referral to rheumatologists. This highlights the need for improving awareness and education regarding axSpA among dermatologists and allied healthcare professionals as well as the public and patients to ensure timely diagnosis. The development of simple and easy-to-administer screening questionnaires to aid non-rheumatologists in identifying patients with IBP together with simplified referral pathways would increase onward referrals of appropriate patients to rheumatologists.
Keywords: ankylosing spondylitis; arthritis; axial spondyloarthritis; inflammatory back pain; psoriasis.
Copyright © 2024, Watts et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Patient Survey Exploring the Burden of Inflammatory Back Pain in Patients With Uveitis.Cureus. 2023 Apr 12;15(4):e37473. doi: 10.7759/cureus.37473. eCollection 2023 Apr. Cureus. 2023. PMID: 37187633 Free PMC article.
-
A Survey Exploring Inflammatory Back Pain in Patients With Inflammatory Bowel Disease.Cureus. 2024 Feb 29;16(2):e55264. doi: 10.7759/cureus.55264. eCollection 2024 Feb. Cureus. 2024. PMID: 38558651 Free PMC article.
-
The prevalence and clinical characteristics of nonradiographic axial spondyloarthritis among patients with inflammatory back pain in rheumatology practices: a multinational, multicenter study.Arthritis Res Ther. 2016 Jun 7;18(1):132. doi: 10.1186/s13075-016-1027-9. Arthritis Res Ther. 2016. PMID: 27267875 Free PMC article.
-
Recognizing Axial Spondyloarthritis: A Guide for Primary Care.Mayo Clin Proc. 2020 Nov;95(11):2499-2508. doi: 10.1016/j.mayocp.2020.02.007. Epub 2020 Jul 29. Mayo Clin Proc. 2020. PMID: 32736944 Review.
-
Axial Spondyloarthritis in the Chiropractic Care Setting: A Systematic Literature Review.J Clin Rheumatol. 2022 Mar 1;28(2):e589-e595. doi: 10.1097/RHU.0000000000001776. J Clin Rheumatol. 2022. PMID: 34294660 Free PMC article.
Cited by
-
Inhibition of the JAK-STAT Pathway in the Treatment of Psoriasis: A Review of the Literature.Int J Mol Sci. 2024 Apr 25;25(9):4681. doi: 10.3390/ijms25094681. Int J Mol Sci. 2024. PMID: 38731900 Free PMC article. Review.
References
-
- Diagnostic delay in axial spondyloarthritis: a systematic review and meta-analysis. Zhao SS, Pittam B, Harrison NL, Ahmed AE, Goodson NJ, Hughes DM. Rheumatology (Oxford) 2021;60:1620–1628. - PubMed
-
- Delayed diagnosis is linked to worse outcomes and unfavourable treatment responses in patients with axial spondyloarthritis. Seo MR, Baek HL, Yoon HH, Ryu HJ, Choi HJ, Baek HJ, Ko KP. Clin Rheumatol. 2015;34:1397–1405. - PubMed
-
- Axial disease in psoriatic arthritis and ankylosing spondylitis: a critical comparison. Feld J, Chandran V, Haroon N, Inman R, Gladman D. Nat Rev Rheumatol. 2018;14:363–371. - PubMed
-
- Prevalence of psoriatic arthritis in patients with psoriasis: a systematic review and meta-analysis of observational and clinical studies. Alinaghi F, Calov M, Kristensen LE, et al. J Am Acad Dermatol. 2019;80:251–265. - PubMed
-
- Prevalence of rheumatologist-diagnosed psoriatic arthritis in patients with psoriasis in European/North American dermatology clinics. Mease PJ, Gladman DD, Papp KA, et al. J Am Acad Dermatol. 2013;69:729–735. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous