Aberrant MET Receptor Tyrosine Kinase Signaling in Glioblastoma: Targeted Therapy and Future Directions
- PMID: 38334610
- PMCID: PMC10854665
- DOI: 10.3390/cells13030218
Aberrant MET Receptor Tyrosine Kinase Signaling in Glioblastoma: Targeted Therapy and Future Directions
Abstract
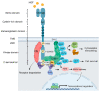
Brain tumors represent a heterogeneous group of neoplasms characterized by a high degree of aggressiveness and a poor prognosis. Despite recent therapeutic advances, the treatment of brain tumors, including glioblastoma (GBM), an aggressive primary brain tumor associated with poor prognosis and resistance to therapy, remains a significant challenge. Receptor tyrosine kinases (RTKs) are critical during development and in adulthood. Dysregulation of RTKs through activating mutations and gene amplification contributes to many human cancers and provides attractive therapeutic targets for treatment. Under physiological conditions, the Met RTK, the hepatocyte growth factor/scatter factor (HGF/SF) receptor, promotes fundamental signaling cascades that modulate epithelial-to-mesenchymal transition (EMT) involved in tissue repair and embryogenesis. In cancer, increased Met activity promotes tumor growth and metastasis by providing signals for proliferation, survival, and migration/invasion. Recent clinical genomic studies have unveiled multiple mechanisms by which MET is genetically altered in GBM, including focal amplification, chromosomal rearrangements generating gene fusions, and a splicing variant mutation (exon 14 skipping, METex14del). Notably, MET overexpression contributes to chemotherapy resistance in GBM by promoting the survival of cancer stem-like cells. This is linked to distinctive Met-induced pathways, such as the upregulation of DNA repair mechanisms, which can protect tumor cells from the cytotoxic effects of chemotherapy. The development of MET-targeted therapies represents a major step forward in the treatment of brain tumours. Preclinical studies have shown that MET-targeted therapies (monoclonal antibodies or small molecule inhibitors) can suppress growth and invasion, enhancing the efficacy of conventional therapies. Early-phase clinical trials have demonstrated promising results with MET-targeted therapies in improving overall survival for patients with recurrent GBM. However, challenges remain, including the need for patient stratification, the optimization of treatment regimens, and the identification of mechanisms of resistance. This review aims to highlight the current understanding of mechanisms underlying MET dysregulation in GBM. In addition, it will focus on the ongoing preclinical and clinical assessment of therapies targeting MET dysregulation in GBM.
Keywords: MET exon 14 skipping; MET-targeted therapies; glioblastoma (GBM); hepatocyte growth factor/scatter factor (HGF/SF).
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

Similar articles
-
The plasticity of oncogene addiction: implications for targeted therapies directed to receptor tyrosine kinases.Neoplasia. 2009 May;11(5):448-58, 2 p following 458. doi: 10.1593/neo.09230. Neoplasia. 2009. PMID: 19412429 Free PMC article.
-
Expression of hepatocyte growth factor/scatter factor and its receptor c-Met in brain tumors: evidence for a role in progression of astrocytic tumors (Review).Int J Mol Med. 1999 May;3(5):531-6. doi: 10.3892/ijmm.3.5.531. Int J Mol Med. 1999. PMID: 10202187 Review.
-
The Role of EGFR-Met Interactions in the Pathogenesis of Glioblastoma and Resistance to Treatment.Curr Cancer Drug Targets. 2017;17(3):297-302. doi: 10.2174/1568009616666161215162515. Curr Cancer Drug Targets. 2017. PMID: 28004613 Review.
-
MET in glioma: signaling pathways and targeted therapies.J Exp Clin Cancer Res. 2019 Jun 20;38(1):270. doi: 10.1186/s13046-019-1269-x. J Exp Clin Cancer Res. 2019. PMID: 31221203 Free PMC article. Review.
-
Foretinib induces G2/M cell cycle arrest, apoptosis, and invasion in human glioblastoma cells through c-MET inhibition.Cancer Chemother Pharmacol. 2021 Jun;87(6):827-842. doi: 10.1007/s00280-021-04242-0. Epub 2021 Mar 10. Cancer Chemother Pharmacol. 2021. PMID: 33688998
Cited by
-
Targeting c-Met in Cancer Therapy: Unravelling Structure-activity Relationships and Docking Insights for Enhanced Anticancer Drug Design.Curr Top Med Chem. 2025;25(4):409-433. doi: 10.2174/0115680266331025241015084546. Curr Top Med Chem. 2025. PMID: 39484763 Review.
-
Chitosan-Coated Liposome Formulations for Encapsulation of Ciprofloxacin and Etoposide.Pharmaceutics. 2024 Aug 2;16(8):1036. doi: 10.3390/pharmaceutics16081036. Pharmaceutics. 2024. PMID: 39204381 Free PMC article.
-
Recent Treatment Strategies and Molecular Pathways in Resistance Mechanisms of Antiangiogenic Therapies in Glioblastoma.Cancers (Basel). 2024 Aug 27;16(17):2975. doi: 10.3390/cancers16172975. Cancers (Basel). 2024. PMID: 39272834 Free PMC article. Review.
-
Evolution of Molecular Biomarkers and Precision Molecular Therapeutic Strategies in Glioblastoma.Cancers (Basel). 2024 Oct 29;16(21):3635. doi: 10.3390/cancers16213635. Cancers (Basel). 2024. PMID: 39518074 Free PMC article. Review.
-
The MET Oncogene: Thirty Years of Insights into Molecular Mechanisms Driving Malignancy.Pharmaceuticals (Basel). 2024 Mar 30;17(4):448. doi: 10.3390/ph17040448. Pharmaceuticals (Basel). 2024. PMID: 38675409 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

