Epicardial ablation of ventricular tachycardia in ischemic cardiomyopathy: A review and local experience
- PMID: 38340957
- PMCID: PMC11010455
- DOI: 10.1016/j.ipej.2024.02.002
Epicardial ablation of ventricular tachycardia in ischemic cardiomyopathy: A review and local experience
Abstract
Myocardial scar in ischemic cardiomyopathy is predominantly endocardial, however, between 5% and 15% of these patients have an arrhythmogenic epicardial substrate. Percutaneous epicardial ablation should be considered in patients with ICM and VT especially if they failed an endocardial ablation. Simultaneous epicardial and endocardial ablation of VT in ICM may reduce short- and medium-term VT recurrence compared with an endocardial only approach. Cardiac imaging could be used to help guide patient selection for a combined epi-endo approach. Complications related to epicardial access can happen in up to 7% of patients. Epicardial ablation in these patients should be referred to experienced tertiary centers. We review the literature and share interesting cases.
Copyright © 2024 Indian Heart Rhythm Society. Published by Elsevier B.V. All rights reserved.
Conflict of interest statement
Declaration of competing interest Dr Roukoz has received no disclosures related to the content of this manuscript. Dr.Tholakanahalli has no relevant disclosures.
Figures
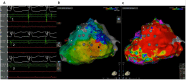
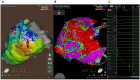
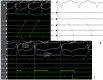



Similar articles
-
Combined Endocardial-Epicardial Versus Endocardial Catheter Ablation Alone for Ventricular Tachycardia in Structural Heart Disease: A Systematic Review and Meta-Analysis.JACC Clin Electrophysiol. 2019 Jan;5(1):13-24. doi: 10.1016/j.jacep.2018.08.010. Epub 2018 Sep 26. JACC Clin Electrophysiol. 2019. PMID: 30678778
-
Epicardial ventricular tachycardia in ischemic cardiomyopathy: Prevalence, electrophysiological characteristics, and long-term ablation outcomes.J Cardiovasc Electrophysiol. 2018 Nov;29(11):1530-1539. doi: 10.1111/jce.13739. Epub 2018 Oct 8. J Cardiovasc Electrophysiol. 2018. PMID: 30230120
-
Endocardial ablation to eliminate epicardial arrhythmia substrate in scar-related ventricular tachycardia.J Am Coll Cardiol. 2014 Apr 15;63(14):1416-26. doi: 10.1016/j.jacc.2013.10.087. Epub 2014 Jan 30. J Am Coll Cardiol. 2014. PMID: 24486269
-
Endocardial Scar-Homogenization With vs Without Epicardial Ablation in VT Patients With Ischemic Cardiomyopathy.JACC Clin Electrophysiol. 2022 Apr;8(4):453-461. doi: 10.1016/j.jacep.2021.12.011. Epub 2022 Feb 23. JACC Clin Electrophysiol. 2022. PMID: 35246406
-
Endo-epicardial ablation vs endocardial ablation for the management of ventricular tachycardia in arrhythmogenic right ventricular cardiomyopathy: A systematic review and meta-analysis.J Cardiovasc Electrophysiol. 2020 Aug;31(8):2022-2031. doi: 10.1111/jce.14593. Epub 2020 Jun 18. J Cardiovasc Electrophysiol. 2020. PMID: 32478430
References
-
- Moss A.J., Schuger C., Beck C.A., Brown M.W., Cannom D.S., Daubert J.P., Estes N.A., 3rd, Greenberg H., Hall W.J., Huang D.T., Kautzner J., Klein H., McNitt S., Olshansky B., Shoda M., Wilber D., Zareba W. Reduction in inappropriate therapy and mortality through ICD programming. N Engl J Med. 2012;367:2275–2283. - PubMed
-
- Kuck K.H., Schaumann A., Eckardt L., Willems S., Ventura R., Delacrétaz E., Pitschner H.F., Kautzner J., Schumacher B., Hansen P.S. Catheter ablation of stable ventricular tachycardia before defibrillator implantation in patients with coronary heart disease (VTACH): a multicentre randomised controlled trial. Lancet (London, England) 2010;375:31–40. - PubMed
-
- Tung R., Michowitz Y., Yu R., Mathuria N., Vaseghi M., Buch E., Bradfield J., Fujimura O., Gima J., Discepolo W., Mandapati R., Shivkumar K. Epicardial ablation of ventricular tachycardia: an institutional experience of safety and efficacy. Heart Rhythm. 2013;10:490–498. - PubMed
-
- Sarkozy A., Tokuda M., Tedrow U.B., Sieria J., Michaud G.F., Couper G.S., John R., Stevenson W.G. Epicardial ablation of ventricular tachycardia in ischemic heart disease. Circulation Arrhythmia and electrophysiology. 2013;6:1115–1122. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
