Multimodality radiomics for tumor prognosis in nasopharyngeal carcinoma
- PMID: 38346058
- PMCID: PMC10861073
- DOI: 10.1371/journal.pone.0298111
Multimodality radiomics for tumor prognosis in nasopharyngeal carcinoma
Abstract
Background: The prognosis of nasopharyngeal carcinoma (NPC) is challenging due to late-stage identification and frequently undetectable Epstein-Barr virus (EBV) DNA. Incorporating radiomic features, which quantify tumor characteristics from imaging, may enhance prognosis assessment.
Purpose: To investigate the predictive power of radiomic features on overall survival (OS), progression-free survival (PFS), and distant metastasis-free survival (DMFS) in NPC.
Materials and methods: A retrospective analysis of 183 NPC patients treated with chemoradiotherapy from 2010 to 2019 was conducted. All patients were followed for at least three years. The pretreatment CT images with contrast medium, MR images (T1W and T2W), as well as gross tumor volume (GTV) contours, were used to extract radiomic features using PyRadiomics v.2.0. Robust and efficient radiomic features were chosen using the intraclass correlation test and univariate Cox proportional hazard regression analysis. They were then combined with clinical data including age, gender, tumor stage, and EBV DNA level for prognostic evaluation using Cox proportional hazard regression models with recursive feature elimination (RFE) and were optimized using 20 repetitions of a five-fold cross-validation scheme.
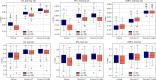
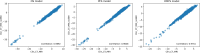
Results: Integrating radiomics with clinical data significantly enhanced the predictive power, yielding a C-index of 0.788 ± 0.066 to 0.848 ± 0.079 for the combined model versus 0.745 ± 0.082 to 0.766 ± 0.083 for clinical data alone (p<0.05). Multimodality radiomics combined with clinical data offered the highest performance. Despite the absence of EBV DNA, radiomics integration significantly improved survival predictions (C-index ranging from 0.770 ± 0.070 to 0.831 ± 0.083 in combined model versus 0.727 ± 0.084 to 0.734 ± 0.088 in clinical model, p<0.05).
Conclusions: The combination of multimodality radiomic features from CT and MR images could offer superior predictive performance for OS, PFS, and DMFS compared to relying on conventional clinical data alone.
Copyright: © 2024 Khongwirotphan et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

Similar articles
-
Prognostic values of the integrated model incorporating the volume of metastatic regional cervical lymph node and pretreatment serum Epstein-Barr virus DNA copy number in predicting distant metastasis in patients with N1 nasopharyngeal carcinoma.Chin J Cancer. 2017 Dec 29;36(1):98. doi: 10.1186/s40880-017-0264-x. Chin J Cancer. 2017. PMID: 29284539 Free PMC article.
-
Proposed modifications and incorporation of plasma Epstein-Barr virus DNA improve the TNM staging system for Epstein-Barr virus-related nasopharyngeal carcinoma.Cancer. 2019 Jan 1;125(1):79-89. doi: 10.1002/cncr.31741. Epub 2018 Oct 23. Cancer. 2019. PMID: 30351466
-
Combination of Tumor Volume and Epstein-Barr Virus DNA Improved Prognostic Stratification of Stage II Nasopharyngeal Carcinoma in the Intensity Modulated Radiotherapy Era: A Large-Scale Cohort Study.Cancer Res Treat. 2018 Jul;50(3):861-871. doi: 10.4143/crt.2017.237. Epub 2017 Sep 13. Cancer Res Treat. 2018. PMID: 28903550 Free PMC article.
-
Prognostic value of Epstein-Barr virus DNA load in nasopharyngeal carcinoma: a meta-analysis.Pan Afr Med J. 2022 Jan 3;41:6. doi: 10.11604/pamj.2022.41.6.28946. eCollection 2022. Pan Afr Med J. 2022. PMID: 35145598 Free PMC article. Review.
-
Epstein-Barr Virus DNA in Nasopharyngeal Carcinoma: A Brief Review.Methods Mol Biol. 2020;2204:99-107. doi: 10.1007/978-1-0716-0904-0_9. Methods Mol Biol. 2020. PMID: 32710318 Review.
Cited by
-
Radiomics for differential diagnosis of ischemic and dilated cardiomyopathy using non-contrast-enhanced cine cardiac magnetic resonance imaging.Radiol Med. 2025 May;130(5):650-661. doi: 10.1007/s11547-025-01979-z. Epub 2025 Mar 10. Radiol Med. 2025. PMID: 40063167
-
A bibliometric analysis of nasopharyngeal carcinoma radiomics: trends and insights.Front Oncol. 2025 Mar 25;15:1506778. doi: 10.3389/fonc.2025.1506778. eCollection 2025. Front Oncol. 2025. PMID: 40201350 Free PMC article.
-
Enhanced MRI Radiomics Based Model for Predicting Recurrence or Metastasis of Nasopharyngeal Cancer (NC) Undergoing Concurrent Chemoradiotherapy: A Retrospective Study.Cancer Control. 2024 Jan-Dec;31:10732748241250208. doi: 10.1177/10732748241250208. Cancer Control. 2024. PMID: 38716756 Free PMC article.
-
Deciphering the Prognostic Efficacy of MRI Radiomics in Nasopharyngeal Carcinoma: A Comprehensive Meta-Analysis.Diagnostics (Basel). 2024 Apr 29;14(9):924. doi: 10.3390/diagnostics14090924. Diagnostics (Basel). 2024. PMID: 38732337 Free PMC article.
-
Integrating Radiomics and Deep-Learning for Prognostic Evaluation in Nasopharyngeal Carcinoma.Medicina (Kaunas). 2025 Jul 21;61(7):1310. doi: 10.3390/medicina61071310. Medicina (Kaunas). 2025. PMID: 40731938 Free PMC article. Review.
References
-
- Wei WI, Sham JS. Nasopharyngeal carcinoma. The Lancet. 2005;365(9476):2041–54. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

