Postpartum pharmacologic thromboprophylaxis and complications in a US cohort
- PMID: 38346912
- PMCID: PMC11194157
- DOI: 10.1016/j.ajog.2023.11.013
Postpartum pharmacologic thromboprophylaxis and complications in a US cohort
Abstract
Background: Venous thromboembolism accounts for approximately 9% of pregnancy-related deaths in the United States. National guidelines recommend postpartum risk stratification and pharmacologic prophylaxis in at-risk individuals. Knowledge on modern rates of postpartum pharmacologic thromboprophylaxis and its associated risks is limited.
Objective: This study aimed to describe the rate of, and factors associated with, initiation of postpartum pharmacologic prophylaxis for venous thromboembolism, and to assess associated adverse outcomes.
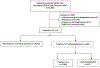
Study design: This was a secondary analysis of a multicenter cohort of individuals delivering on randomly selected days at 17 US hospitals (2019-2020). Medical records were reviewed by trained and certified personnel. Those with an antepartum diagnosis of venous thromboembolism, receiving antepartum anticoagulation, or known SARS-CoV-2 infection were excluded. The primary outcome was use of postpartum pharmacologic thromboprophylaxis. Secondary outcomes included bleeding complications, surgical site infection, hospital readmission, and venous thromboembolism through 6 weeks postpartum. The rate of thromboprophylaxis administration was assessed by mode of delivery, institution, and continuance to the outpatient setting. Multivariable regression models were developed using k-fold cross-validation with stepwise backward elimination to evaluate factors associated with thromboprophylaxis administration. Univariable and multivariable logistic models with propensity score covariate adjustment were performed to assess the association between thromboprophylaxis administration and adverse outcomes.
Results: Of 21,114 individuals in the analytical cohort, 11.9% (95% confidence interval, 11.4%-12.3%) received postpartum pharmacologic thromboprophylaxis; the frequency of receipt was 29.8% (95% confidence interval, 28.7%-30.9%) following cesarean and 3.5% (95% confidence interval, 3.2%-3.8%) following vaginal delivery. Institutional rates of prophylaxis varied from 0.21% to 34.8%. Most individuals (83.3%) received thromboprophylaxis only as inpatients. In adjusted analysis, cesarean delivery (adjusted odds ratio, 19.17; 95% confidence interval, 16.70-22.00), hysterectomy (adjusted odds ratio, 15.70; 95% confidence interval, 4.35-56.65), and obesity (adjusted odds ratio, 3.45; 95% confidence interval, 3.02-3.95) were the strongest factors associated with thromboprophylaxis administration. Thromboprophylaxis administration was not associated with surgical site infection (0.9% vs 0.6%; odds ratio, 1.48; 95% confidence interval, 0.80-2.74), bleeding complications (0.2% vs 0.1%; odds ratio, 2.60; 95% confidence interval, 0.99-6.80), or postpartum readmission (0.9% vs 0.3%; adjusted odds ratio, 1.38; 95% confidence interval, 0.68-2.81). The overall rate of venous thromboembolism was 0.06% (95% confidence interval, 0.03%-0.10%) and was higher in those receiving prophylaxis (0.2%) compared with those not receiving prophylaxis (0.04%).
Conclusion: Approximately 1 in 10 patients received postpartum pharmacologic thromboprophylaxis in this US cohort. Rates of prophylaxis varied widely by institution. Cesarean delivery, hysterectomy, and obesity were predominant factors associated with postpartum thromboprophylaxis administration.
Keywords: bleeding complications; heparin-based prophylaxis; postcesarean thromboprophylaxis; postpartum thromboembolism; rates of prophylaxis; wound complications.
Copyright © 2023. Published by Elsevier Inc.
Conflict of interest statement
Figures
References
-
- Clark SL, Belfort MA. The Case for a National Maternal Mortality Review Committee. Obstet Gynecol 2017;130:198–202. - PubMed
-
- Thromboembolism in Pregnancy. ACOG Practice Bulletin No. 196. American College of Obstetricians and Gynecologists. Obstet Gynecol 2018;132:e1–e17. - PubMed
-
- Farmakis LT, Barco S, Hobohm L, Braekkan SK, Connors JM, Giannakoulas G, et al. Maternal mortality related to pulmonary embolism in the United States, 2003–2020. Am J Obstet Gynecol MFM 2022;5:100754. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- UG1 HD027869/HD/NICHD NIH HHS/United States
- UG1 HD040560/HD/NICHD NIH HHS/United States
- UG1 HD087230/HD/NICHD NIH HHS/United States
- UG1 HD053097/HD/NICHD NIH HHS/United States
- K12 HD085816/HD/NICHD NIH HHS/United States
- UG1 HD040545/HD/NICHD NIH HHS/United States
- UG1 HD112063/HD/NICHD NIH HHS/United States
- UG1 HD040485/HD/NICHD NIH HHS/United States
- U10 HD040560/HD/NICHD NIH HHS/United States
- UG1 HD040500/HD/NICHD NIH HHS/United States
- UL1 TR001873/TR/NCATS NIH HHS/United States
- U24 HD036801/HD/NICHD NIH HHS/United States
- UG1 HD027915/HD/NICHD NIH HHS/United States
- UG1 HD087192/HD/NICHD NIH HHS/United States
- UG1 HD040544/HD/NICHD NIH HHS/United States
- UG1 HD034208/HD/NICHD NIH HHS/United States
- UG1 HD040512/HD/NICHD NIH HHS/United States
LinkOut - more resources
Full Text Sources
Miscellaneous