Neuroimaging features of primary central nervous system post-transplantation lymphoproliferative disorder following hematopoietic stem cell transplant in patients with β-thalassemia: a case series and review of literature
- PMID: 38353902
- PMCID: PMC10866827
- DOI: 10.1186/s13244-024-01605-y
Neuroimaging features of primary central nervous system post-transplantation lymphoproliferative disorder following hematopoietic stem cell transplant in patients with β-thalassemia: a case series and review of literature
Abstract
Purpose: Primary central nervous system post-transplantation lymphoproliferative disorder (PCNS-PTLD) is a rare but serious complication of hematopoietic stem cell transplantation (HSCT) in patients with severe β-thalassemia. This study aimed to assess the clinical presentation, pathological characteristics, neuroimaging findings, and treatment strategies in patients with β-thalassemia who developed PCNS-PTLD and to compare a case series from our transplant center to reported cases from literature.
Methods: We retrospectively reviewed our hospital database and identified four cases of pathologically confirmed PCNS-PTLD without a history of systemic PTLD in patients with severe β-thalassemia after HSCT. We also performed a relevant literature review on PCNS-PTLD.
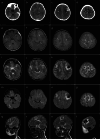
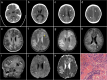
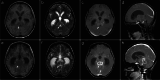
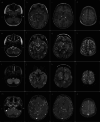
Results: The median time from transplantation to diagnosis of PCNS-PTLD was 5.5 months. Intracerebral lesions were usually multiple involving both supratentorial and infratentorial regions with homogeneous or rim enhancement. All patients had pathologically confirmed PCNS-PTLD with three patients having diffuse large B-cell lymphoma and the fourth patient having plasmacytic hyperplasia. There was low response to treatment with a median survival of 83 days.
Conclusion: PCNS-PTLD should be considered in the differential diagnosis of patients with β-thalassemia who had an intracranial lesion on neuroimaging after HSCT.
Critical relevance statement: This case series with a comprehensive review of neuroimaging and clinical characteristics of children with primary central nervous system post-transplantation lymphoproliferative disorder should advance our understanding and improve management of this rare yet severe complication following transplant for β-thalassemia.
Key points: • We assessed clinical presentation, treatment strategies, and neuroimaging characteristics of PCNS-PTLD in patients with β-thalassemia after transplantation. • Patients with β-thalassemia may have post-transplantation lymphoproliferative disorder presenting as brain lesions on neuroimaging. • Neuroimaging findings of the brain lesions are helpful for prompt diagnosis and proper management.
Keywords: Central nervous system; Hematopoietic stem cell transplantation; Magnetic resonance imaging; Post-transplantation lymphoproliferative disorder; β-thalassemia.
© 2024. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
References
-
- Styczynski J, Van Der Velden W, Fox CP, et al. Management of Epstein-Barr virus infections and post-transplant lymphoproliferative disorders in patients after allogeneic hematopoietic stem cell transplantation: Sixth European Conference on Infections in Leukemia (ECIL-6) guidelines. Haematologica. 2016;101:803–811. doi: 10.3324/haematol.2016.144428. - DOI - PMC - PubMed
-
- Bonney DK, Htwe EE, Turner A, et al. Sustained response to intrathecal rituximab in EBV associated Post-transplant lymphoproliferative disease confined to the central nervous system following haematopoietic stem cell transplant: intrathecal rituximab in CNS PTLD. Pediatr Blood Cancer. 2012;58:459–461. doi: 10.1002/pbc.23134. - DOI - PubMed
LinkOut - more resources
Full Text Sources

