Melatonin treatment has consistent but transient beneficial effects on sleep measures and pain in patients with severe chronic pain: the DREAM-CP randomised controlled trial
- PMID: 38355388
- PMCID: PMC10925889
- DOI: 10.1016/j.bja.2024.01.012
Melatonin treatment has consistent but transient beneficial effects on sleep measures and pain in patients with severe chronic pain: the DREAM-CP randomised controlled trial
Abstract
Background: Sleep disturbance is a major issue for patients with chronic pain. Melatonin has been shown to improve symptoms of fibromyalgia, but its efficacy in other chronic non-malignant pain conditions is not fully known. Hence, we determined the effect of melatonin in patients with severe noncancer chronic pain.
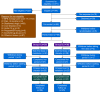
Methods: This was a randomised double-blinded crossover trial of modified-release melatonin as Circadin™ compared with placebo. Sixty male and female subjects with chronic severe pain were randomised to receive either 2 mg of Circadin™ or placebo before sleep for 6 weeks, followed by a >4 week washout, then crossing over to the other treatment. Sleep disturbance, quality, and latency were measured using three different validated sleep assessment tools. The primary outcome measure was self-reported sleep disturbance after 6 weeks of treatment. Adverse events were also recorded.
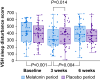
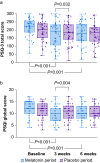
Results: Sleep disturbance after 6 weeks was not significantly altered by melatonin treatment, but differences between melatonin and placebo treatment periods after 3 weeks were seen: sleep disturbance (P=0.014), latency (P=0.04), overall sleep quality (P=0.004), and effect of pain on sleep (P=0.032). Pain intensity scores improved during both treatment periods (both P<0.001). There were no differences in adverse events between treatment periods.
Conclusions: Circadin™ treatment did not improve sleep disturbance in patients with severe chronic pain compared with placebo at 6 weeks, but there were consistent improvements in aspects of sleep in the shorter term. Given its favourable safety profile, it could be beneficial for some patients with chronic pain.
Clinical trial registration: ISRCTN12861060.
Keywords: chronic pain; clinical trial; crossover; melatonin; sleep.
Copyright © 2024 The Author(s). Published by Elsevier Ltd.. All rights reserved.
Conflict of interest statement
HFG is a trustee and director of the
Figures

Similar articles
-
Phase II double-blind randomised controlled trial of exogenous administration of melatonin in chronic pain (DREAM-CP): a study protocol.BMJ Open. 2020 Mar 16;10(3):e034443. doi: 10.1136/bmjopen-2019-034443. BMJ Open. 2020. PMID: 32184313 Free PMC article. Clinical Trial.
-
Efficacy of melatonin for sleep disturbance following traumatic brain injury: a randomised controlled trial.BMC Med. 2018 Jan 19;16(1):8. doi: 10.1186/s12916-017-0995-1. BMC Med. 2018. PMID: 29347988 Free PMC article. Clinical Trial.
-
Efficacy of melatonin with behavioural sleep-wake scheduling for delayed sleep-wake phase disorder: A double-blind, randomised clinical trial.PLoS Med. 2018 Jun 18;15(6):e1002587. doi: 10.1371/journal.pmed.1002587. eCollection 2018 Jun. PLoS Med. 2018. PMID: 29912983 Free PMC article. Clinical Trial.
-
Adverse Events Associated with Melatonin for the Treatment of Primary or Secondary Sleep Disorders: A Systematic Review.CNS Drugs. 2019 Dec;33(12):1167-1186. doi: 10.1007/s40263-019-00680-w. CNS Drugs. 2019. PMID: 31722088
-
Hypnotic and Melatonin/Melatonin-Receptor Agonist Treatment in Bipolar Disorder: A Systematic Review and Meta-Analysis.CNS Drugs. 2022 Apr;36(4):345-363. doi: 10.1007/s40263-022-00911-7. Epub 2022 Mar 19. CNS Drugs. 2022. PMID: 35305257
Cited by
-
Melatonin supplementation: new insights into health and disease.Sleep Breath. 2025 Apr 25;29(2):169. doi: 10.1007/s11325-025-03331-1. Sleep Breath. 2025. PMID: 40278958 Review.
-
Melatonin and sleep parameters in infertile women with endometriosis: first results from the triple-blind randomized controlled trial of administration of melatonin in chronic pelvic pain and sleep disturbance.PLoS One. 2025 Apr 16;20(4):e0321635. doi: 10.1371/journal.pone.0321635. eCollection 2025. PLoS One. 2025. PMID: 40238733 Free PMC article. Clinical Trial.
References
-
- Menefee L.A., Cohen M.J.M., Anderson W.R., Doghramji K., Frank E.D., Lee H. Sleep disturbance and nonmalignant chronic pain: a comprehensive review of the literature. Pain Med. 2000;1:156–172. - PubMed
-
- Sun Y., Laksono I., Selvanathan J., et al. Prevalence of sleep disturbances in patients with chronic non-cancer pain: a systematic review and meta-analysis. Sleep Med Rev. 2021;57 - PubMed
-
- Smith M.T., Haythornthwaite J.A. How do sleep disturbance and chronic pain inter-relate? Insights from the longitudinal and cognitive-behavioral clinical trials literature. Sleep Med Rev. 2004;8:119–132. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

