CD4/CD8 ratio and CD8+ T-cell count as prognostic markers for non-AIDS mortality in people living with HIV. A systematic review and meta-analysis
- PMID: 38361925
- PMCID: PMC10868578
- DOI: 10.3389/fimmu.2024.1343124
CD4/CD8 ratio and CD8+ T-cell count as prognostic markers for non-AIDS mortality in people living with HIV. A systematic review and meta-analysis
Erratum in
-
Corrigendum: CD4/CD8 ratio and CD8+ T-cell count as prognostic markers for non-AIDS mortality in people living with HIV. A systematic review and meta-analysis.Front Immunol. 2024 Feb 20;15:1383117. doi: 10.3389/fimmu.2024.1383117. eCollection 2024. Front Immunol. 2024. PMID: 38444860 Free PMC article.
Abstract
Background: In people living with HIV (PLHIV), the CD4/CD8 ratio has been proposed as a useful marker for non-AIDS events. However, its predictive ability on mortality over CD4 counts, and the role of CD8+ T-cell counts remain controversial.
Methods: We conducted a systematic review and meta-analysis of published studies from 1996 to 2023, including PLHIV on antiretroviral treatment, and reporting CD4/CD8 ratio or CD8+ counts. The primary outcome was non-AIDS mortality or all-cause mortality. We performed a standard random-effects pairwise meta-analysis comparing low versus high CD4/CD8 ratio with a predefined cut-off point of 0.5. (CRD42020170931).
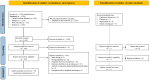
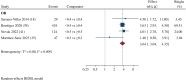
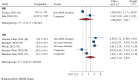
Findings: We identified 2,479 studies for screening. 20 studies were included in the systematic review. Seven studies found an association between low CD4/CD8 ratio categories and increased mortality risk, with variable cut-off points between 0.4-1. Four studies were selected for meta-analysis, including 12,893 participants and 618 reported deaths. Patients with values of CD4/CD8 ratio below 0.5 showed a higher mortality risk (OR 3.65; 95% CI 3.04 - 4.35; I2 = 0.00%) compared to those with higher values. While the meta-analysis of CD8+ T-cell counts was not feasible due to methodological differences between studies, the systematic review suggests a negative prognostic impact of higher values (>1,138 to 1,500 cells/uL) in the long term.
Conclusions: Our results support the use of the CD4/CD8 ratio as a prognostic marker in clinical practice, especially in patients with values below 0.5, but consensus criteria on ratio timing measurement, cut-off values, and time to event are needed in future studies to get more robust conclusions.
Systematic review registration: https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42020170931, identifier CRD42020170931.
Keywords: CD4/CD8 ratio; HIV; comorbidities; mortality; non-AIDS events.
Copyright © 2024 Ron, Martínez-Sanz, Herrera, Ramos-Ruperto, Díez, Sainz, Álvarez-Díaz, Correa-Pérez, Muriel, López-Alcalde, Pérez-Molina, Moreno and Serrano-Villar.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Predictive value of CD8+ T cell and CD4/CD8 ratio at two years of successful ART in the risk of AIDS and non-AIDS events.EBioMedicine. 2022 Jun;80:104072. doi: 10.1016/j.ebiom.2022.104072. Epub 2022 May 26. EBioMedicine. 2022. PMID: 35644125 Free PMC article.
-
Low blood CD8+ T-lymphocytes and high circulating monocytes are predictors of HIV-1-associated progressive encephalopathy in children.Pediatrics. 2003 Feb;111(2):E168-75. doi: 10.1542/peds.111.2.e168. Pediatrics. 2003. PMID: 12563091
-
CD4+:CD8+ T-cell ratio changes in people with HIV receiving antiretroviral treatment.Antivir Ther. 2020;25(2):91-100. doi: 10.3851/IMP3354. Antivir Ther. 2020. PMID: 32338638
-
Weight loss and mortality in people living with HIV: a systematic review and meta-analysis.BMC Infect Dis. 2024 Jan 2;24(1):34. doi: 10.1186/s12879-023-08889-3. BMC Infect Dis. 2024. PMID: 38166819 Free PMC article.
-
T-Cell Subsets and Interleukin-10 Levels Are Predictors of Severity and Mortality in COVID-19: A Systematic Review and Meta-Analysis.Front Med (Lausanne). 2022 Apr 28;9:852749. doi: 10.3389/fmed.2022.852749. eCollection 2022. Front Med (Lausanne). 2022. PMID: 35572964 Free PMC article.
Cited by
-
Markers of T-cell dysfunction and not inflammaging predict the waning of humoral responses to SARS-CoV-2 mRNA booster vaccination in people with HIV.AIDS. 2024 Nov 15;38(14):1987-1990. doi: 10.1097/QAD.0000000000004010. Epub 2024 Oct 31. AIDS. 2024. PMID: 39474654 Free PMC article.
-
Changes in the immune index before and after surgery in urinary malignancy patients with AIDS.Sci Rep. 2025 Apr 4;15(1):11569. doi: 10.1038/s41598-025-96606-2. Sci Rep. 2025. PMID: 40185921 Free PMC article.
-
Long-term immune responses to SARS-CoV-2 Omicron BA.4/5 mRNA booster in people living with HIV.Commun Med (Lond). 2025 Mar 27;5(1):92. doi: 10.1038/s43856-025-00799-6. Commun Med (Lond). 2025. PMID: 40148493 Free PMC article.
-
Circulating Biomarker Panorama in HIV-Associated Lymphoma: A Bridge from Early Risk Warning to Prognostic Stratification.Biomolecules. 2025 Jul 11;15(7):993. doi: 10.3390/biom15070993. Biomolecules. 2025. PMID: 40723865 Free PMC article. Review.
-
Enhanced metabolic health and immune response with bictegravir/emtricitabine/TAF: Insights from a 96‑week retrospective study.Biomed Rep. 2024 Oct 2;21(6):179. doi: 10.3892/br.2024.1867. eCollection 2024 Dec. Biomed Rep. 2024. PMID: 39387001 Free PMC article.
References
-
- Collins LF, Sheth AN, Mehta CC, Naggie S, Golub ET, Anastos K, et al. . The prevalence and burden of non-AIDS comorbidities among women living with or at risk for human immunodeficiency virus infection in the United States. Clin Infect Dis (2021) 72(8):1301–11. doi: 10.1093/cid/ciaa204 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

