Treatment seeking behaviours, antibiotic use and relationships to multi-drug resistance: A study of urinary tract infection patients in Kenya, Tanzania and Uganda
- PMID: 38363770
- PMCID: PMC10871516
- DOI: 10.1371/journal.pgph.0002709
Treatment seeking behaviours, antibiotic use and relationships to multi-drug resistance: A study of urinary tract infection patients in Kenya, Tanzania and Uganda
Abstract
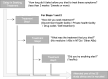
Antibacterial resistance (ABR) is a major public health threat. An important accelerating factor is treatment-seeking behaviour, including inappropriate antibiotic (AB) use. In many low- and middle-income countries (LMICs) this includes taking ABs with and without prescription sourced from various providers, including health facilities and community drug sellers. However, investigations of complex treatment-seeking, AB use and drug resistance in LMICs are scarce. The Holistic Approach to Unravel Antibacterial Resistance in East Africa (HATUA) Consortium collected questionnaire and microbiological data from adult outpatients with urinary tract infection (UTI)-like symptoms presenting at healthcare facilities in Kenya, Tanzania and Uganda. Using data from 6,388 patients, we analysed patterns of self-reported treatment seeking behaviours ('patient pathways') using process mining and single-channel sequence analysis. Among those with microbiologically confirmed UTI (n = 1,946), we used logistic regression to assess the relationship between treatment seeking behaviour, AB use, and the likelihood of having a multi-drug resistant (MDR) UTI. The most common treatment pathway for UTI-like symptoms in this sample involved attending health facilities, rather than other providers like drug sellers. Patients from sites in Tanzania and Uganda, where over 50% of patients had an MDR UTI, were more likely to report treatment failures, and have repeat visits to providers than those from Kenyan sites, where MDR UTI proportions were lower (33%). There was no strong or consistent relationship between individual AB use and likelihood of MDR UTI, after accounting for country context. The results highlight the hurdles East African patients face in accessing effective UTI care. These challenges are exacerbated by high rates of MDR UTI, suggesting a vicious cycle of failed treatment attempts and sustained selection for drug resistance. Whilst individual AB use may contribute to the risk of MDR UTI, our data show that factors related to context are stronger drivers of variations in ABR.
Copyright: © 2024 Sado et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures






Update of
-
Treatment seeking behaviours, antibiotic use and relationships to multi-drug resistance: A study of urinary tract infection patients in Kenya, Tanzania and Uganda.medRxiv [Preprint]. 2023 Mar 20:2023.03.04.23286801. doi: 10.1101/2023.03.04.23286801. medRxiv. 2023. Update in: PLOS Glob Public Health. 2024 Feb 16;4(2):e0002709. doi: 10.1371/journal.pgph.0002709. PMID: 36945627 Free PMC article. Updated. Preprint.
References
-
- O’Neill J. Antimicrobial Resistance: Tackling a crisis for the health and wealth of nations. 2014.
Grants and funding
LinkOut - more resources
Full Text Sources
