Non-psychotic Outcomes in Young People at Ultra-High Risk of Developing a Psychotic Disorder: A Long-Term Follow-up Study
- PMID: 38366898
- PMCID: PMC11548927
- DOI: 10.1093/schbul/sbae005
Non-psychotic Outcomes in Young People at Ultra-High Risk of Developing a Psychotic Disorder: A Long-Term Follow-up Study
Abstract
Background: The majority of individuals at ultra-high risk (UHR) for psychosis do not transition to a full threshold psychotic disorder. It is therefore important to understand their longer-term clinical and functional outcomes, particularly given the high prevalence of comorbid mental disorders in this population at baseline.
Aims: This study investigated the prevalence of non-psychotic disorders in the UHR population at entry and long-term follow-up and their association with functional outcomes. Persistence of UHR status was also investigated.
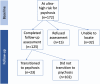
Study design: The sample comprised 102 UHR young people from the Personal Assessment and Crisis Evaluation (PACE) Clinic who had not transitioned to psychosis by long-term follow-up (mean = 8.8 years, range = 6.8-12.1 years since baseline).
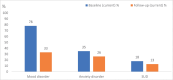
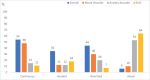
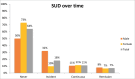
Results: Eighty-eight percent of participants at baseline were diagnosed with at least one mental disorder, the majority of which were mood disorders (78%), anxiety disorders (35%), and substance use disorders (SUDs) (18%). This pattern of disorder prevalence continued at follow-up, though prevalence was reduced, with 52% not meeting criteria for current non-psychotic mental disorder. However, 35% of participants developed a new non-psychotic mental disorder by follow-up. Presence of a continuous non-psychotic mental disorder was associated with poorer functional outcomes at follow-up. 28% of participants still met UHR criteria at follow-up.
Conclusions: The study adds to the evidence base that a substantial proportion of UHR individuals who do not transition to psychosis experience persistent attenuated psychotic symptoms and persistent and incident non-psychotic disorders over the long term. Long-term treatment and re-entry into services is indicated.
Keywords: UHR; comorbid mental disorders; long-term outcomes; ultra-high risk for psychosis.
© The Author(s) 2024. Published by Oxford University Press on behalf of the Maryland Psychiatric Research Center.
Figures

Similar articles
-
Persistence or recurrence of non-psychotic comorbid mental disorders associated with 6-year poor functional outcomes in patients at ultra high risk for psychosis.J Affect Disord. 2016 Oct;203:101-110. doi: 10.1016/j.jad.2016.05.053. Epub 2016 May 31. J Affect Disord. 2016. PMID: 27285723
-
Long-term follow-up of a group at ultra high risk ("prodromal") for psychosis: the PACE 400 study.JAMA Psychiatry. 2013 Aug;70(8):793-802. doi: 10.1001/jamapsychiatry.2013.1270. JAMA Psychiatry. 2013. PMID: 23739772
-
Impact of psychiatric comorbidity in individuals at Ultra High Risk of psychosis - Findings from the Longitudinal Youth at Risk Study (LYRIKS).Schizophr Res. 2015 May;164(1-3):8-14. doi: 10.1016/j.schres.2015.03.007. Epub 2015 Mar 25. Schizophr Res. 2015. PMID: 25818728
-
Prevalence of non-psychotic disorders in ultra-high risk individuals and transition to psychosis: A systematic review.Psychiatry Res. 2018 Dec;270:1-12. doi: 10.1016/j.psychres.2018.09.028. Epub 2018 Sep 15. Psychiatry Res. 2018. PMID: 30243126
-
Early psychotic experiences: Interventions, problems and perspectives.Psychiatriki. 2015 Jan-Mar;26(1):45-54. Psychiatriki. 2015. PMID: 25880383 Review.
Cited by
-
Development and temporal validation of a clinical prediction model of transition to psychosis in individuals at ultra-high risk in the UHR 1000+ cohort.World Psychiatry. 2024 Oct;23(3):400-410. doi: 10.1002/wps.21240. World Psychiatry. 2024. PMID: 39279417 Free PMC article.
References
-
- Yung AR, Phillips LJ, Yuen HP, et al.Psychosis prediction: 12-month follow up of a high-risk (“prodromal”) group. Schizophr Res. 2003;60(1):21–32. - PubMed
-
- de Wit S, Schothorst PF, Oranje B, Ziermans TB, Durston S, Kahn RS.. Adolescents at ultra-high risk for psychosis: long-term outcome of individuals who recover from their at-risk state. Eur Neuropsychopharmacol. 2014;24(6):865–873. - PubMed
-
- Wiltink S, Velthorst E, Nelson B, McGorry PD, Yung AR.. Declining transition rates to psychosis: the contribution of potential changes in referral pathways to an ultra-high-risk service. Early Intervn Psychiatry. 2015;9(3):200–206. - PubMed
-
- Fusar-Poli P, Bonoldi, I, Yung AR, et al.Predicting psychosis: meta-analysis of transition outcomes in individuals at high clinical risk. Arch Gen Psychiatry. 2012;69(3):220–229. - PubMed
-
- Hartmann JA, Yuen HP, McGorry PD, et al.Declining transition rates to psychotic disorder in “ultra-high risk” clients: investigation of a dilution effect. Schizophr Res. 2016;170(1):130–136. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

