Validation of resting full-cycle ratio and diastolic pressure ratio with [15O]H2O positron emission tomography myocardial perfusion
- PMID: 38367040
- PMCID: PMC10920410
- DOI: 10.1007/s00380-023-02356-4
Validation of resting full-cycle ratio and diastolic pressure ratio with [15O]H2O positron emission tomography myocardial perfusion
Abstract
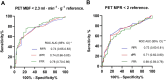
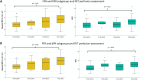
Fractional flow reserve (FFR) and instantaneous wave-free ratio (iFR) are invasive techniques used to evaluate the hemodynamic significance of coronary artery stenosis. These methods have been validated through perfusion imaging and clinical trials. New invasive pressure ratios that do not require hyperemia have recently emerged, and it is essential to confirm their diagnostic efficacy. The aim of this study was to validate the resting full-cycle ratio (RFR) and the diastolic pressure ratio (dPR), against [15O]H2O positron emission tomography (PET) imaging. A total of 129 symptomatic patients with an intermediate risk of coronary artery disease (CAD) were included. All patients underwent cardiac [15O]H2O PET with quantitative assessment of resting and hyperemic myocardial perfusion. Within a 2 week period, coronary angiography was performed. Intracoronary pressure measurements were obtained in 320 vessels and RFR, dPR, and FFR were computed. PET derived regional hyperemic myocardial blood flow (hMBF) and myocardial perfusion reserve (MPR) served as reference standards. In coronary arteries with stenoses (43%, 136 of 320), the overall diagnostic accuracies of RFR, dPR, and FFR did not differ when PET hyperemic MBF < 2.3 ml min-1 (69.9%, 70.6%, and 77.1%, respectively) and PET MPR < 2.5 (70.6%, 71.3%, and 66.9%, respectively) were considered as the reference for myocardial ischemia. Non-significant differences between the areas under the receiver operating characteristic (ROC) curve were found between the different indices. Furthermore, the integration of FFR with RFR (or dPR) does not enhance the diagnostic information already achieved by FFR in the characterization of ischemia via PET perfusion. In conclusion, the novel non-hyperemic pressure ratios, RFR and dPR, have a diagnostic performance comparable to FFR in assessing regional myocardial ischemia. These findings suggest that RFR and dPR may be considered as an FFR alternative for invasively guiding revascularization treatment in symptomatic patients with CAD.
Keywords: FFR; NHPR; Positron emission tomography; RFR; dPR.
© 2024. The Author(s).
Conflict of interest statement
The present work is a researcher-driven investigation, and neither of the authors nor the institutions involved have received any funding for this purpose. JS is the Chief Executive Officer of Coroventis and acted as an unsubsidized corelab for the analysis of dPR and RFR, while being blinded to any patient data, including angiograms, PET scans, hyperemic pressure traces, and FFR results. NvR and TvdH have received speaker fees and institutional research grants from Abbott and Philips. The remaining authors have no conflicts of interest or disclosures to report.
Figures
Similar articles
-
Prevalence of myocardial perfusion scintigraphy derived ischemia in coronary lesions with discordant fractional flow reserve and non-hyperemic pressure ratios.Int J Cardiol. 2022 Jun 15;357:20-25. doi: 10.1016/j.ijcard.2022.02.031. Epub 2022 Feb 24. Int J Cardiol. 2022. PMID: 35219745
-
Physiological and Clinical Assessment of Resting Physiological Indexes.Circulation. 2019 Feb 12;139(7):889-900. doi: 10.1161/CIRCULATIONAHA.118.037021. Circulation. 2019. PMID: 30586749
-
Hemodynamic Insights into Combined Fractional Flow Reserve and Instantaneous Wave-Free Ratio Assessment Through Quantitative [15O]H2O PET Myocardial Perfusion Imaging.J Nucl Med. 2024 Feb 1;65(2):279-286. doi: 10.2967/jnumed.123.265973. J Nucl Med. 2024. PMID: 38176722
-
Instantaneous wave-free ratio as an alternative to fractional flow reserve in assessment of moderate coronary stenoses: A meta-analysis of diagnostic accuracy studies.Cardiovasc Revasc Med. 2018 Jul-Aug;19(5 Pt B):613-620. doi: 10.1016/j.carrev.2017.12.014. Epub 2017 Dec 27. Cardiovasc Revasc Med. 2018. PMID: 29371084 Review.
-
Pooled diagnostic accuracy of resting distal to aortic coronary pressure referenced to fractional flow reserve: The importance of resting coronary physiology.J Interv Cardiol. 2018 Oct;31(5):588-598. doi: 10.1111/joic.12517. Epub 2018 Apr 29. J Interv Cardiol. 2018. PMID: 29707808 Review.
References
-
- Fearon WF, Nishi T, De Bruyne B, Boothroyd DB, Barbato E, Tonino P, Jüni P, Pijls NHJ, Hlatky MA. Clinical Outcomes and Cost-Effectiveness of Fractional Flow Reserve-Guided Percutaneous Coronary Intervention in Patients With Stable Coronary Artery Disease: Three-Year Follow-Up of the FAME 2 Trial (Fractional Flow Reserve Versus Angiography for Multivessel Evaluation) Circulation. 2018;137(5):480–487. doi: 10.1161/CIRCULATIONAHA.117.031907. - DOI - PubMed
-
- Knuuti J, Wijns W, Saraste A, Capodanno D, Barbato E, Funck-Brentano C, Prescott E, Storey RF, Deaton C, Cuisset T, Agewall S, Dickstein K, Edvardsen T, Escaned J, Gersh BJ, Svitil P, Gilard M, Hasdai D, Hatala R, Mahfoud F, Masip J, Muneretto C, Valgimigli M, Achenbach S, Bax JJ. 2019 ESC Guidelines for the diagnosis and management of chronic coronary syndromes. Eur Heart J. 2020;41(3):407–477. doi: 10.1093/eurheartj/ehz425. - DOI - PubMed
-
- Davies JE, Sen S, Dehbi H-M, Al-Lamee R, Petraco R, Nijjer SS, Bhindi R, Lehman SJ, Walters D, Sapontis J, Janssens L, Vrints CJ, Khashaba A, Laine M, Van Belle E, Krackhardt F, Bojara W, Going O, Härle T, Indolfi C, Niccoli G, Ribichini F, Tanaka N, Yokoi H, Takashima H, Kikuta Y, Erglis A, Vinhas H, Canas Silva P, Baptista SB, Alghamdi A, Hellig F, Koo B-K, Nam C-W, Shin E-S, Doh J-H, Brugaletta S, Alegria-Barrero E, Meuwissen M, Piek JJ, van Royen N, Sezer M, Di Mario C, Gerber RT, Malik IS, Sharp ASP, Talwar S, Tang K, Samady H, Altman J, Seto AH, Singh J, Jeremias A, Matsuo H, Kharbanda RK, Patel MR, Serruys P, Escaned J. Use of the Instantaneous Wave-free Ratio or Fractional Flow Reserve in PCI. N Engl J Med. 2017;376(19):1824–1834. doi: 10.1056/NEJMoa1700445. - DOI - PubMed
-
- Götberg M, Christiansen EH, Gudmundsdottir IJ, Sandhall L, Danielewicz M, Jakobsen L, Olsson S-E, Öhagen P, Olsson H, Omerovic E, Calais F, Lindroos P, Maeng M, Tödt T, Venetsanos D, James SK, Kåregren A, Nilsson M, Carlsson J, Hauer D, Jensen J, Karlsson A-C, Panayi G, Erlinge D, Fröbert O. Instantaneous Wave-free Ratio versus Fractional Flow Reserve to Guide PCI. N Engl J Med. 2017;376(19):1813–1823. doi: 10.1056/NEJMoa1616540. - DOI - PubMed
-
- de Waard GA, Danad I, Petraco R, Driessen RS, Raijmakers PG, Teunissen PF, van de Ven PM, van Leeuwen MAH, Nap A, Harms HJ, Lammertsma AA, Davies JE, Knaapen P, van Royen N. Fractional flow reserve, instantaneous wave-free ratio, and resting Pd/Pa compared with [15O]H2O positron emission tomography myocardial perfusion imaging: a PACIFIC trial sub-study. Eur Heart J. 2018;39(46):4072–4081. doi: 10.1093/eurheartj/ehy632. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

