Assessment of COVID-19 Morbidity and Mortality Among Patients With Autoimmune Diseases at King Abdulaziz University Hospital
- PMID: 38370992
- PMCID: PMC10874129
- DOI: 10.7759/cureus.52492
Assessment of COVID-19 Morbidity and Mortality Among Patients With Autoimmune Diseases at King Abdulaziz University Hospital
Abstract
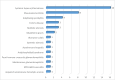
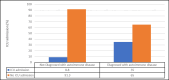
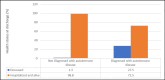
Background The coronavirus disease 2019 (COVID-19) pandemic has raised significant concerns about the effects of the virus on patients with autoimmune diseases. Therefore, understanding the COVID-19 outcomes in this population is crucial for effective prevention and management. Objective This study aimed to investigate the association between autoimmune diseases and the severity of COVID-19 in terms of mortality and morbidity. Despite substantial advancements in pandemic-related research concerning COVID-19 and autoimmune diseases, there remain noteworthy gaps in our comprehension of this association, particularly due to limited investigations conducted in Saudi Arabia. Methods This was a retrospective record review of a tertiary center from January 2020 to January 2022. We included 120 patients, among whom 40 were diagnosed with autoimmune diseases, and 80 were age- and sex-matched controls. Afterward, we assessed their demographics, year of admission, intensive care unit (ICU) admission, health status, length of hospitalization, comorbidities, diagnosis of autoimmune diseases, and type of immunosuppressant therapy. Results Most of the included patients (mean age: 45.4 years) were females (65.8%). The ratio of non-autoimmune diseases to autoimmune diseases was 2:1, the mean length of hospitalization was 8.83 ± 8.16 days, and the median was seven days (interquartile range (IQR) = 3 to 11 days). Among them, 17.5% were admitted to the ICU and 10% died. The prevalence of autoimmune diseases was higher in women than in men (77.5%). The most common diseases were systemic lupus erythematosus (40%), rheumatoid arthritis (20%), and ankylosing spondylitis (10%). Regarding COVID-19 outcomes, ICU admissions were higher among patients with autoimmune diseases than those with non-autoimmune diseases (35% vs. 8.8%) (p<0.05). This trend was also observed in mortality, with a higher percentage of deaths among patients with autoimmune diseases (27.5% vs. 1.7%) (p<0.05). In addition, there were no significant differences between genders in terms of ICU admission, health status outcomes, or length of hospitalization among patients with autoimmune diseases (p>0.05). Notably, 25 patients were administered immunosuppressants. Of these, 18 (72%) used steroids only, while seven (28%) used both biological and steroid therapy. However, no significant associations were observed between the type of treatment used and outcomes such as ICU admission, health status at discharge, and length of hospitalization (p>0.05). Conclusion This study suggests that individuals with autoimmune diseases have more severe COVID-19 outcomes, as shown by ICU admission and mortality rates, than patients with non-autoimmune diseases. Furthermore, we observed that the use of immunosuppressant medications among patients with autoimmune diseases showed no noticeable effect on these outcomes.
Keywords: autoimmune diseases; covid-19; immunosuppressants; rheumatoid arthritis; systemic lupus erythematosus.
Copyright © 2024, Altuwairqi et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
COVID-19 in patients with rheumatological diseases in the Eastern Province of Saudi Arabia.J Med Life. 2023 Jun;16(6):873-882. doi: 10.25122/jml-2023-0037. J Med Life. 2023. PMID: 37675163 Free PMC article.
-
Risk Factors Associated With Mortality Among Patients With COVID-19 in Intensive Care Units in Lombardy, Italy.JAMA Intern Med. 2020 Oct 1;180(10):1345-1355. doi: 10.1001/jamainternmed.2020.3539. JAMA Intern Med. 2020. PMID: 32667669 Free PMC article.
-
Association of COVID-19 Vaccinations With Intensive Care Unit Admissions and Outcome of Critically Ill Patients With COVID-19 Pneumonia in Lombardy, Italy.JAMA Netw Open. 2022 Oct 3;5(10):e2238871. doi: 10.1001/jamanetworkopen.2022.38871. JAMA Netw Open. 2022. PMID: 36301541 Free PMC article.
-
A Trial of Favipiravir and Hydroxychloroquine combination in Adults Hospitalized with moderate and severe Covid-19: A structured summary of a study protocol for a randomised controlled trial.Trials. 2020 Oct 31;21(1):904. doi: 10.1186/s13063-020-04825-x. Trials. 2020. PMID: 33129363 Free PMC article.
-
Convalescent plasma or hyperimmune immunoglobulin for people with COVID-19: a rapid review.Cochrane Database Syst Rev. 2020 May 14;5(5):CD013600. doi: 10.1002/14651858.CD013600. Cochrane Database Syst Rev. 2020. Update in: Cochrane Database Syst Rev. 2020 Jul 10;7:CD013600. doi: 10.1002/14651858.CD013600.pub2. PMID: 32406927 Free PMC article. Updated.
References
-
- SARS-CoV-2, immunosenescence and inflammaging: partners in the COVID-19 crime. Domingues R, Lippi A, Setz C, Outeiro TF, Krisko A. https://pubmed.ncbi.nlm.nih.gov/32991323/. Aging (Albany NY) 2020;12:18778–18789. - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
