Effects of menstrual disorders and dysmenorrhea on cardiovascular disease: a Mendelian randomization study
- PMID: 38375191
- PMCID: PMC10875084
- DOI: 10.3389/fendo.2024.1302312
Effects of menstrual disorders and dysmenorrhea on cardiovascular disease: a Mendelian randomization study
Abstract
Background: Observational studies have demonstrated associations between menstrual disorders, dysmenorrhea, and cardiovascular disease (CVD). However, it remains unclear whether these associations are causal. This study is to investigate whether menstrual disorders and dysmenorrhea causally affect the risk of CVD.
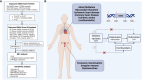
Methods: The summary data for menstrual disorders (excessive menstruation and irregular menses) and dysmenorrhea were obtained from FinnGen study, summary data for CVD were obtained from UK Biobank and meta-analysis. The inverse-variance-weighted method was mainly used in the Mendelian randomization for causality analysis. Sensitivity analyses were performed by several methods under different model assumptions.
Results: Genetic liability to excessive menstruation was associated with higher risk of atrial fibrillation (odds ratio (OR), 1.078 [95% confidence interval (CI), 1.015-1.145]; P=0.014), but a lower risk of hypertension (OR, 0.994 [95% CI: 0.989-0.999]; P=0.016). Irregular menses was associated with higher risk of atrial fibrillation (OR, 1.095 [95% CI: 1.015-1.182]; P=0.02), hypertension (OR, 1.007 [95% CI: 1.000-1.013]; P=0.047), myocardial infarction (OR, 1.172 [95% CI: 1.060-1.295]; P=0.02), ischemic heart disease, (OR, 1.005 [95% CI: 1.000-1.010]; P=0.037) and coronary heart disease (OR, 1.004 [95% CI: 1.001-1.008]; P=0.026). Dysmenorrhea was associated with higher risk of atrial fibrillation (OR, 1.052 [95% CI: 1.014-1.092]; P=0.008) and Ischemic stroke (cardioembolic) (OR, 1.122 [95% CI: 1.002-1.257]; P=0.046). After Benjamini-Hochberg correction, irregular menses was associated with higher risk of myocardial infarction.
Conclusion: We confirmed a causal relationship of excessive menstruation, irregular menses and dysmenorrhea on cardiovascular outcomes independent of sex hormone levels, with an emphasis on the link between irregular menses and myocardial infarction. These clinical features can be utilized as markers to identify women at higher risk of developing CVD in the future, recommending early clinical intervention of menstrual diseases.
Keywords: FinnGen; Mendelian randomization; cardiovascular disease; dysmenorrhea; menstrual disorders.
Copyright © 2024 Lai, Jin, Wang, Li and Wang.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

Similar articles
-
Causal Association Between Anemia and Cardiovascular Disease: A 2-Sample Bidirectional Mendelian Randomization Study.J Am Heart Assoc. 2023 Jun 20;12(12):e029689. doi: 10.1161/JAHA.123.029689. Epub 2023 Jun 10. J Am Heart Assoc. 2023. PMID: 37301769 Free PMC article.
-
Evaluation of the two-way associations between mental disorders and menstrual irregularities: A Mendelian randomization study from both directions.J Affect Disord. 2025 Jul 1;380:232-241. doi: 10.1016/j.jad.2025.03.128. Epub 2025 Mar 24. J Affect Disord. 2025. PMID: 40132666
-
Genetic liability to age at first sex and birth in relation to cardiovascular diseases: a Mendelian randomization study.BMC Med Genomics. 2023 Apr 6;16(1):75. doi: 10.1186/s12920-023-01496-w. BMC Med Genomics. 2023. PMID: 37024926 Free PMC article.
-
Association between adiposity and cardiovascular outcomes: an umbrella review and meta-analysis of observational and Mendelian randomization studies.Eur Heart J. 2021 Sep 7;42(34):3388-3403. doi: 10.1093/eurheartj/ehab454. Eur Heart J. 2021. PMID: 34333589 Free PMC article.
-
Dysmenorrhea and Sleep: A Review.Sleep Med Clin. 2023 Dec;18(4):449-461. doi: 10.1016/j.jsmc.2023.06.006. Epub 2023 Jul 13. Sleep Med Clin. 2023. PMID: 38501517 Review.
Cited by
-
Mendelian randomization studies on ischemic stroke: a field synopsis and systematic review.J Transl Med. 2025 Aug 22;23(1):955. doi: 10.1186/s12967-025-06992-4. J Transl Med. 2025. PMID: 40847399 Free PMC article. Review.
-
Exploratory Ultrasound Analysis of the Diaphragm and Respiratory Capacity in Women with Primary Dysmenorrhea: A Cross-Sectional Observational Study.Methods Protoc. 2025 Feb 4;8(1):15. doi: 10.3390/mps8010015. Methods Protoc. 2025. PMID: 39997639 Free PMC article.
-
Premenstrual disorders and risk of cardiovascular diseases.Nat Cardiovasc Res. 2025 Aug;4(8):1001-1010. doi: 10.1038/s44161-025-00684-4. Epub 2025 Jul 11. Nat Cardiovasc Res. 2025. PMID: 40646267 Free PMC article.
References
-
- Network GBoDC . Global Burden of Disease Study 2019 (GBD 2019) (2020). Available at: https://vizhub.healthdata.org/gbd-results/.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

