Full adherence to cirrhosis quality indicators is associated with lower mortality in acute variceal bleeding: Nationwide audit
- PMID: 38381716
- PMCID: PMC11407775
- DOI: 10.1097/HEP.0000000000000793
Full adherence to cirrhosis quality indicators is associated with lower mortality in acute variceal bleeding: Nationwide audit
Abstract
Background and aims: Acute variceal bleeding (AVB) is a major complication in patients with cirrhosis. Using a nationwide AVB audit, we performed a nested cohort study to determine whether full adherence to the AVB quality indicator (QI) improves clinical outcomes in patients with cirrhosis and AVB.
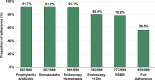
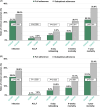
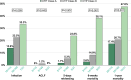
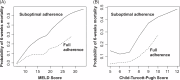
Approach and results: We assessed real-world adherence to AVB QI among patients with cirrhosis admitted for AVB in all public hospitals in Singapore between January 2015 and December 2020. Full adherence was considered when all 5 QIs were fulfilled: prophylactic antibiotics, vasoactive agents, timely endoscopy, endoscopic hemostasis during index endoscopy, and nonselective beta-blockers after AVB. We compare 6-week mortality between the full adherence and suboptimal adherence groups using a propensity-matched cohort.A total of 989 patients with AVB were included. Full adherence to all AVB QI was suboptimal (56.5%). Analysis of the propensity-matched cohort with comparable baseline characteristics showed that full adherence was associated with a lower risk of early infection (20.0% vs. 26.9%), early rebleeding (5.2% vs. 10.2%), and mortality at 6 weeks (8.2% vs. 19.7%) and 1 year (21.3% vs. 35.4%) ( p <0.05 for all). While full adherence was associated with a lower 6-week mortality regardless of the MELD score, nonadherence was associated with a higher 6-week mortality despite a lower predicted risk of 6-week mortality. Despite high adherence to the recommended process measures, patients with CTP-C remain at a higher risk of rebleeding, 6-week and 1-year mortality.
Conclusions: Full adherence to the AVB QI should be the target for quality improvement in patients with cirrhosis.
Copyright © 2024 The Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
Yu Jun Wong is on the speakers’ bureau for AbbVie and Gilead. Juan G. Abraldes consults for 89Bio, Advanz, Astra Zeneca, Boehringer Ingelheim, Boston Pharmaceuticals, and Novo Nordisk. He received grants from Cook and Gilead. The remaining authors have no conflicts to report.
Figures

Comment on
-
Development of Quality Measures in Cirrhosis by the Practice Metrics Committee of the American Association for the Study of Liver Diseases.Hepatology. 2019 Apr;69(4):1787-1797. doi: 10.1002/hep.30489. Epub 2019 Mar 12. Hepatology. 2019. PMID: 30586188
References
-
- Moon AM, Dominitz JA, Ioannou GN, Lowy E, Beste LA. Use of antibiotics among patients with cirrhosis and upper gastrointestinal bleeding is associated with reduced mortality. Clin Gastroenterol Hepatol Off Clin Pract J Am Gastroenterol Assoc. 2016;14:1629–37.e1. - PubMed
-
- Tapper EB, Beste L, Curry M, Bonder A, Waljee A, Saini S. Suboptimal implementation of evidence-based therapy for acute variceal hemorrhage: A systematic review of observational studies. Clin Gastroenterol Hepatol Off Clin Pract J Am Gastroenterol Assoc. 2017;15:1373–81.e7. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

