Analysis of fibrocalcific aortic valve stenosis: computational pre-and-post TAVR haemodynamics behaviours
- PMID: 38384780
- PMCID: PMC10878817
- DOI: 10.1098/rsos.230905
Analysis of fibrocalcific aortic valve stenosis: computational pre-and-post TAVR haemodynamics behaviours
Abstract
Fibro-calcific aortic valve (AV) diseases are characterized by calcium growth or accumulation of fibrosis in the AV tissues. Fibrocalcific aortic stenosis (FAS) rises specifically in females, like calcification-induced aortic stenosis (CAS), may eventually necessitate valve replacement. Fluid-structure-interaction (FSI) computational models for severe CAS and FAS patients were developed using lattice Boltzmann method and multi-scale finite elements (FE). Three parametric AV models were introduced: pathology-free of non-calcified tri-and-bicuspid AVs with healthy collagen fibre network (CFN), a FAS model incorporated a thickened CFN with embedded small calcification volumes, and a CAS model employs healthy CFN with embedded high calcification volumes. The results indicate that the interaction between calcium deposits, adjacent tissue and fibres crucially influences haemodynamics and structural reactions. A fourth model of transcatheter aortic valve replacement (TAVR) post-procedure outcomes was created to study both CAS and FAS. TAVR-CAS had a higher maximum contact pressure and lower anchoring area than TAVR-FAS, making it prone to aortic tissue damage and migration. Finally, although the TAVR-CAS offered a larger opening area, its paravalvular leakage was higher. This may be attributed to a similar thrombogenicity potential characterizing both models. The computational framework emphasizes the significance of mechanobiology in FAS and underscores the requirement for tissue modelling at multiple scales.
Keywords: calcific aortic valve; fibrosis; finite element; fluid–structure interaction; lattice Boltzmann method.
© 2024 The Authors.
Conflict of interest statement
Karin Lavon is an employee of Edwards Lifesciences Ltd. Danny Bluestein has an equity interest in PolyNova Cardiovascular Inc. All other authors declare no financial or personal affiliations with individuals or organizations that could potentially influence or bias the publication of this study.
Figures


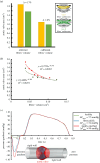





References
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
